reSee.it - Tweets Saved By @JanuaryDoNoHarm

@JanuaryDoNoHarm - January Littlejohn
How do @UMichAlumni feel about their university not only promoting gender ideology pseudoscience to their pediatric patients, but also chemically castrating children with puberty blockers & performing double mastectomies on teen girls? Let’s meet one of their doctors. 🧵 https://t.co/kdNrszz3xl

@JanuaryDoNoHarm - January Littlejohn
Boston Children’s Hospital wants you to forget they were proud of poisoning vulnerable children with puberty blockers & cross sex hormones & cutting off their healthy body parts in their marketing videos. Thank you to @BillboardChris for exposing these. Here are all of them.🧵 https://t.co/MYUbcXoAst
@JanuaryDoNoHarm - January Littlejohn
@JanuaryDoNoHarm - January Littlejohn
@JanuaryDoNoHarm - January Littlejohn
@JanuaryDoNoHarm - January Littlejohn
@JanuaryDoNoHarm - January Littlejohn
@JanuaryDoNoHarm - January Littlejohn
@JanuaryDoNoHarm - January Littlejohn
@JanuaryDoNoHarm - January Littlejohn
@JanuaryDoNoHarm - January Littlejohn
@JanuaryDoNoHarm - January Littlejohn
@JanuaryDoNoHarm - January Littlejohn
@JanuaryDoNoHarm - January Littlejohn
@JanuaryDoNoHarm - January Littlejohn
@JanuaryDoNoHarm - January Littlejohn
@JanuaryDoNoHarm - January Littlejohn
@JanuaryDoNoHarm - January Littlejohn
@JanuaryDoNoHarm - January Littlejohn
@JanuaryDoNoHarm - January Littlejohn
@JanuaryDoNoHarm - January Littlejohn
@JanuaryDoNoHarm - January Littlejohn
@JanuaryDoNoHarm - January Littlejohn
@JanuaryDoNoHarm - January Littlejohn
@JanuaryDoNoHarm - January Littlejohn

@JanuaryDoNoHarm - January Littlejohn
I have been sent important research on the effects of estrogen on the male brain by a researcher who wishes to remain anonymous. "Giving estrogen to young males for GD is like giving cyanide to cancer patients just because “someone said it helps.” 🧵1/25 @LeorSapir @jaypgreene
@JanuaryDoNoHarm - January Littlejohn
2/ The effects of estrogen therapy on menopausal women have been studied for some time, but in the last few years, there has been a host of research on the effect of estrogen on trans women (TW). All of such research have been published in reputed medical journals.
@JanuaryDoNoHarm - January Littlejohn
3/ Excess estrogen in the serum in natal males has been associated with depression – studies both among adult men doi.org/10.1016/j.psyn… and adolescent boys doi.org/10.1016/j.jad.… show that.
@JanuaryDoNoHarm - January Littlejohn
4/ Clinical studies (i.e., studies that recruit actual subjects rather than rely on anonymous, online, non-probability surveys) that promote gender medicine fail to show any improvement in psychosocial outcomes among AMAB, e.g., the NEJM study doi.org/10.1056/NEJMoa….
@JanuaryDoNoHarm - January Littlejohn
5/ In the main text, the study finds no improvement in depression, anxiety symptoms, or life satisfaction among natal male youth nejm.org/doi/pdf/10.105… 📷
@JanuaryDoNoHarm - January Littlejohn
6/ Why estrogen causes depression: 12 mths of estrogen treatment among trans women decreased serum BDNF levels doi.org/10.1016/j.euro…. Decrease in BDNF is associated with increased risks of developing major depressive disorder doi.org/10.1186/s13104….
@JanuaryDoNoHarm - January Littlejohn
7/ *Physiologically*, recent research shows that estrogen has far more serious effects.
@JanuaryDoNoHarm - January Littlejohn
8/ In male rats, estrogen changed the brain to resemble those in brains of TW doi.org/10.1016/j.yhbe…. It reduces the water content in the astrocytes, shrinking cortical structures and increasing ventricular volume, which has been observed in other studies among TW. 7/
@JanuaryDoNoHarm - January Littlejohn
9/ Why is that important? Astrocytes control the glutamate (a neurotransmitter) released at the synapses. They optimize neuronal functions and prevent “glutamate excitotoxicity” – a prolonged or exacerbated activation of glutamate receptors https://doi.org/10.3390/cells8020184
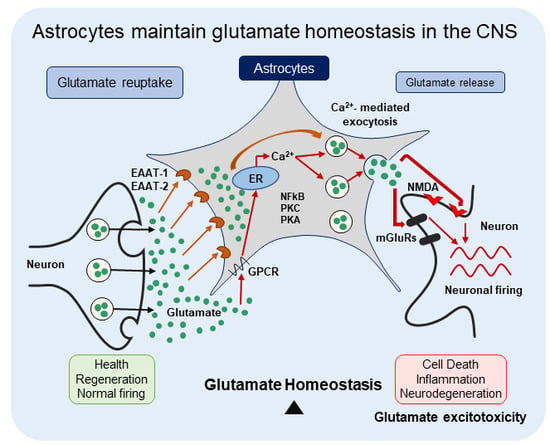
@JanuaryDoNoHarm - January Littlejohn
10/ Glutamate excitotoxicity can start "a cascade of neurotoxicity,” leading to the loss of neuronal function and cell death, which then leads to neurodegenerative diseases doi.org/10.3389/fncel.….
@JanuaryDoNoHarm - January Littlejohn
11/ What does that mean? It turns out that an increase in glutamate in the brain can lead to neurological disorders like Alzheimer's, ALS, Parkinson’s, MS, and fibromyalgia. bit.ly/44DSxMo
@JanuaryDoNoHarm - January Littlejohn
12/ The subcortical changes (decrease in cortical thickness and volume and increase in ventricular structures) brought about by estrogen therapy mentioned above have been linked to many neurological disorders. See the next 4 tweets (12-15)
@JanuaryDoNoHarm - January Littlejohn
13/ Decreasing brain cortical thickness and volume is associated with schizophrenia and bipolar disorder (doi.org/10.1016/j.nicl…) and lower levels of general intelligence (doi.org/10.1016/j.inte…).
@JanuaryDoNoHarm - January Littlejohn
14/ The rodent study found that estrogen treatment reduced white matter integrity, which is associated with cognitive instability (doi.org/10.1523/JNEURO…). And a reduction in gray matter is a prominent feature of Alzheimer's (doi.org/10.3389/fnagi.…).
@JanuaryDoNoHarm - January Littlejohn
15/ The increase in the volume of ventricular structures compresses the brain from within, eventually damaging and destroying brain tissue. aans.org/Patients/Neuro…
@JanuaryDoNoHarm - January Littlejohn
16/ Reduction in hippocampal volume is associated with cognitive dysfunction and is a core symptom in patients with major depression. jpn.ca/content/31/5/3…
@JanuaryDoNoHarm - January Littlejohn
17/ (Estrogen was once believed to be a promising treatment among older menopausal women to delay onset of dementia. The WHIMS study (1996) was designed to test whether HRT reduces incidence of dementia in women 65+. doi.org/10.1016/s0197-… (contd. next 3 tweets)
@JanuaryDoNoHarm - January Littlejohn
18/ (The WHIMS study was discontinued in 2002 as it showed that long-term estrogen-progestin therapy increased the risk of dementia in women aged 65+, leading the researchers to conclude that the risks of HRT outweigh the benefits doi.org/10.1001/jama.2….
@JanuaryDoNoHarm - January Littlejohn
19/ (Now, a new nationwide study from Denmark among menopausal women on estrogen therapy found that it was associated with dementia, even with short-term use (the risks increased with the duration of use), and also among women younger than 65. doi.org/10.1136/bmj-20…
@JanuaryDoNoHarm - January Littlejohn
20/ (In the Danish study, MRI scans of the brain found evidence of brain atrophy, which is associated with cognitive decline and dementia doi.org/10.1148/radiol…. So, two studies associate estrogen therapy with dementia among natal women for its *prescribed* use.)
@JanuaryDoNoHarm - January Littlejohn
21/ Recent research shows that estrogen therapy among trans women has been implicated in various autoimmune diseases, from MS to rheumatoid arthritis and many others (remember that an increase in glutamate is also associated with MS) doi.org/10.1016/j.sema…
@JanuaryDoNoHarm - January Littlejohn
22/ Estrogen increases the risks of prostate cancer (doi.org/10.1586/eem.11…) and breast cancer among natal men (doi.org/10.1200/JCO.20…).
@JanuaryDoNoHarm - January Littlejohn
23/ Among TW, estrogen increases risks of cardiovascular diseases (two separate studies), often by as much as tenfold compared to their cisgender counterparts. doi.org/10.7326/M17-27…, doi.org/10.1161/CIRCUL…
@JanuaryDoNoHarm - January Littlejohn
24/ Validating the abovementioned research, empirically, we see a much higher incidence of many of these physical (doi.org/10.1089/lgbt.2…) and neurological diseases (doi.org/10.1016/j.anne…) in the trans population.
@JanuaryDoNoHarm - January Littlejohn
25/ Not coincidentally, perhaps, population cohort studies (two separate studies) show that trans women, on average, die decades earlier than either cisgender men or women doi.org/10.1016/S2213-…, doi.org/10.1215/007033… @SpencerLndqst @jordanbpeterson