reSee.it - Tweets Saved By @ejustin46

@ejustin46 - Emmanuel
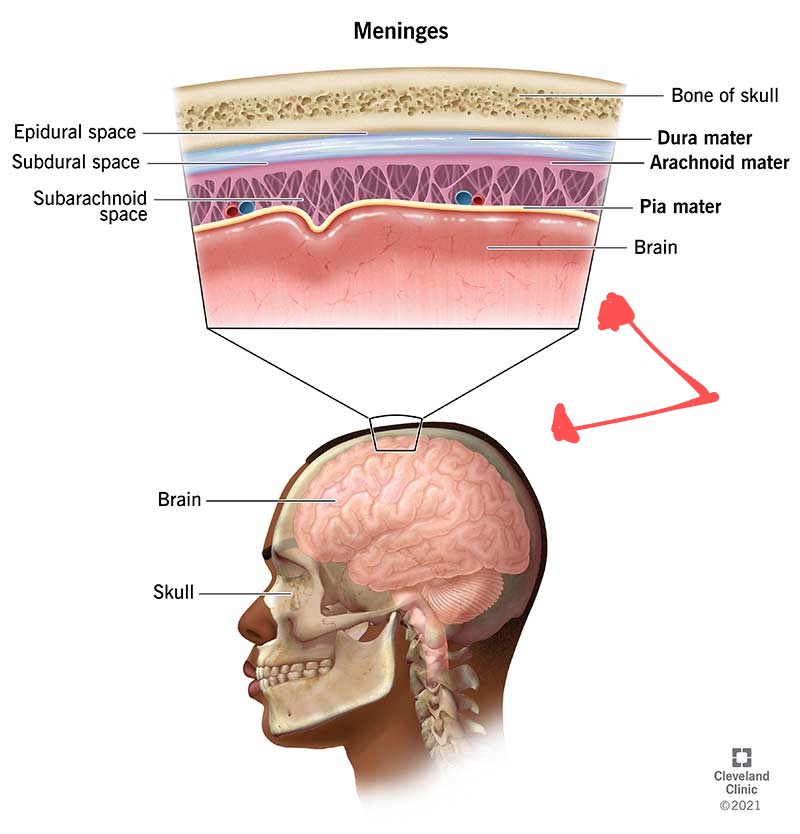
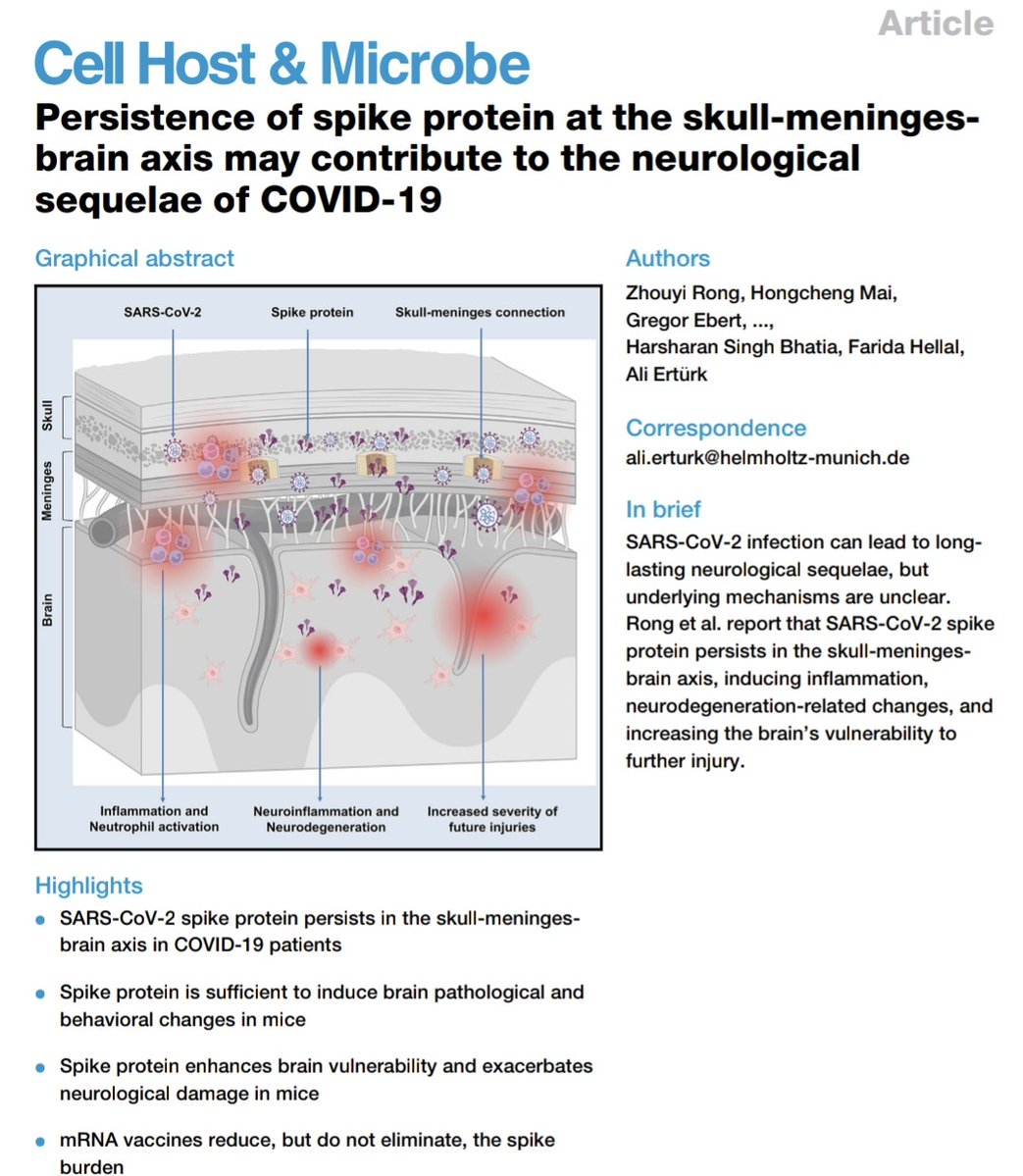
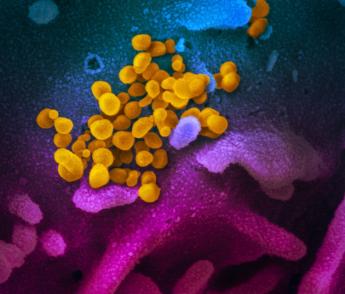
Exploring the Persistence of the Spike Protein along the Skull-Meninges-Brain Axis and the Neurological Effects of COVID-19 This analysis is supported by numerous videos and illustrations. First, let's identify the location of the skull-meninges-brain axis. Here it is 👇 https://t.co/yyUVmpgkW0
@ejustin46 - Emmanuel
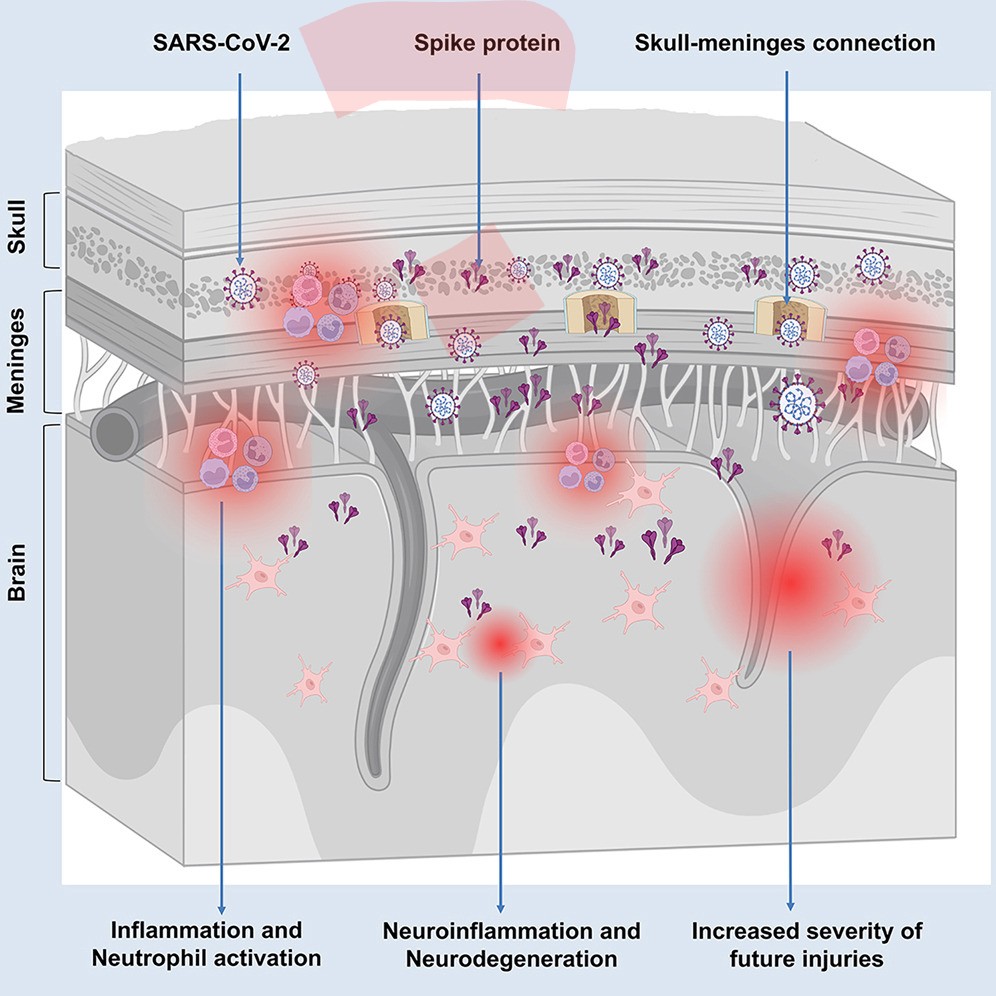
2) Here is where Spike protein persists in skull marrow, meninges, and brain, accumulating in the recently discovered skull-meninges connections 👇 https://t.co/cm6OriqvLy
@ejustin46 - Emmanuel
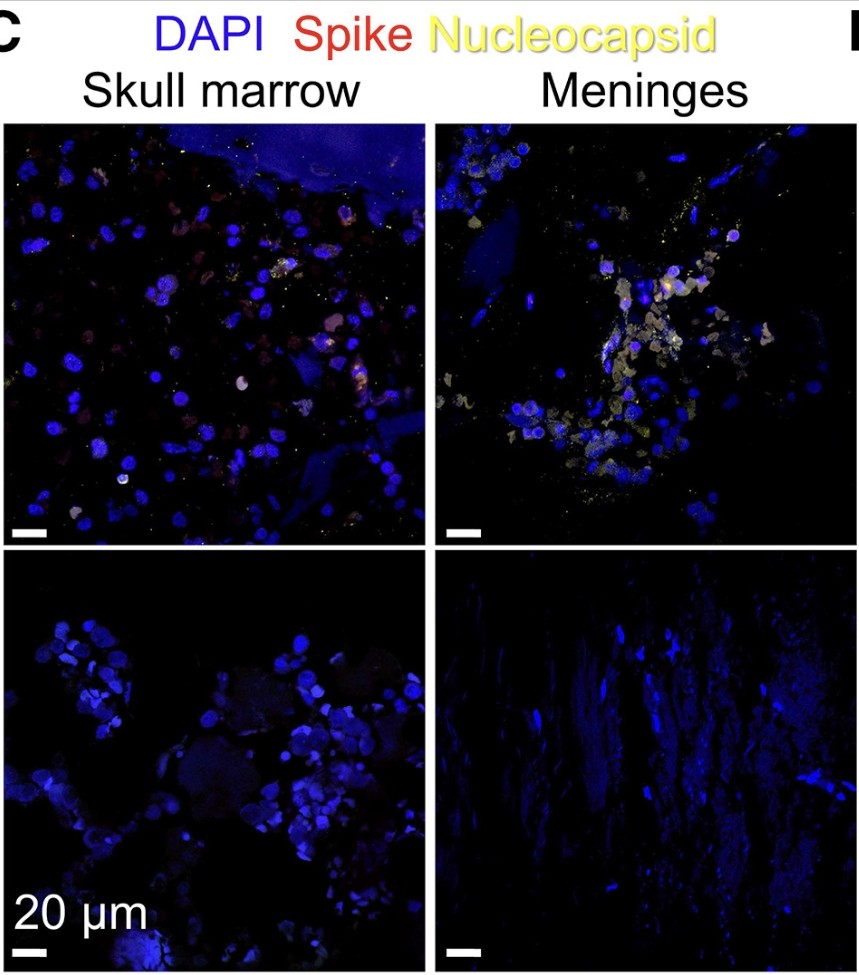
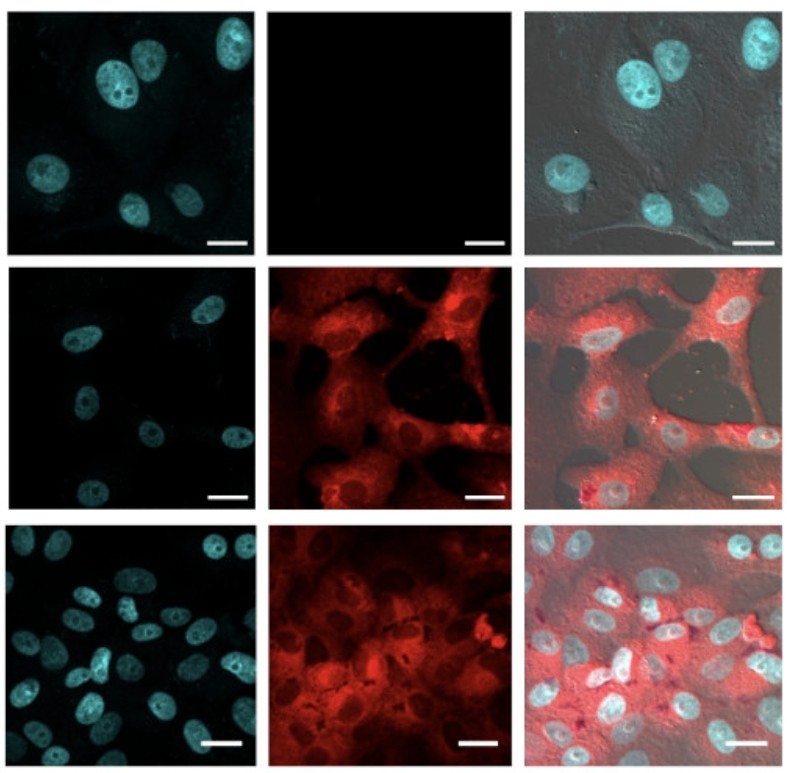
3) Here are the confoncal images showing SARS-CoV-2 spike and nucleocapsid proteins in skull marrow and meninges of COVID-19 patients, indicating viral presence in these brain border regions. https://t.co/pIJpQN2JCr
@ejustin46 - Emmanuel
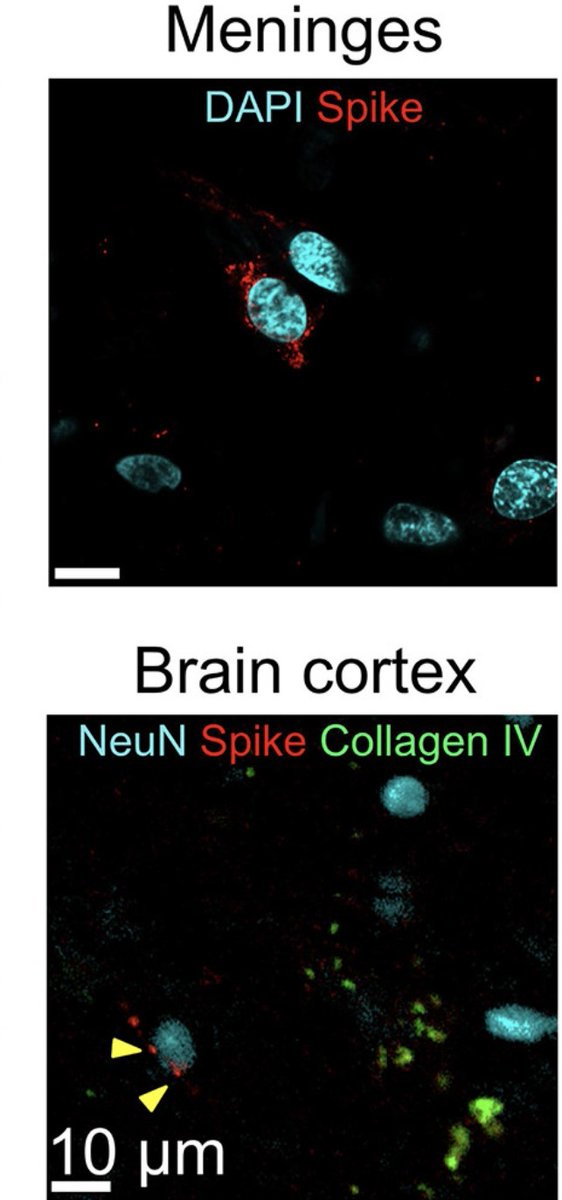
4) This figure shows SARS-CoV-2 spike protein near the nuclei of neurons and meningeal cells in the brain cortex of COVID-19 patients, suggesting viral interaction with brain cells. https://t.co/OZANFOdH5B
@ejustin46 - Emmanuel
5) This video visualizes the distribution of SARS-CoV-2 spike and nucleocapsid proteins throughout the human skull and meninges, highlighting their accumulation in these brain border regions. https://t.co/yqaqaIyT56
@ejustin46 - Emmanuel
6) This video demonstrates the presence of SARS-CoV-2 spike protein in the brain cortex adjacent to the skull in COVID-19 patients, indicating viral entry into the brain parenchyma. https://t.co/3EBqOwuy5n
@ejustin46 - Emmanuel
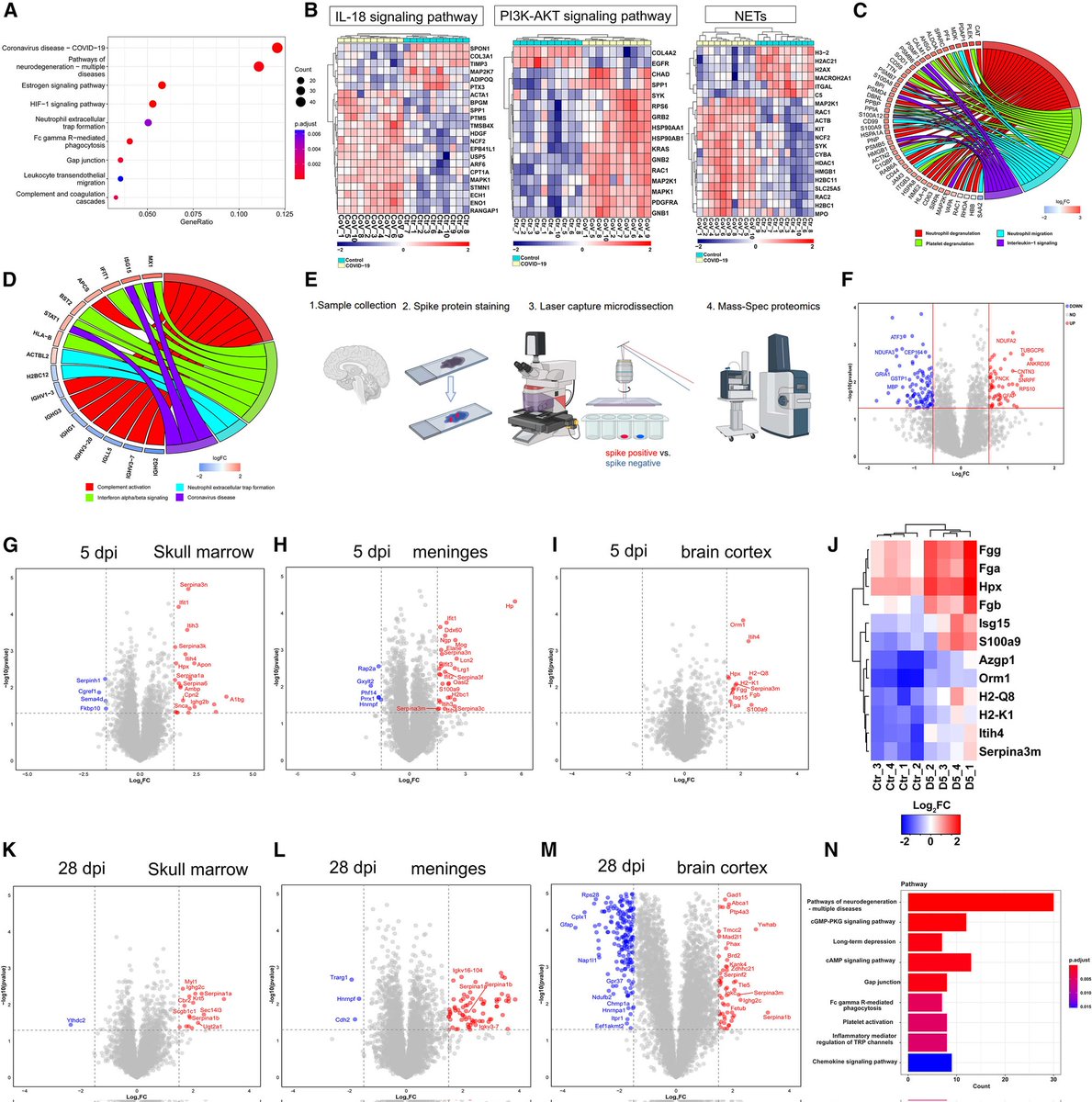
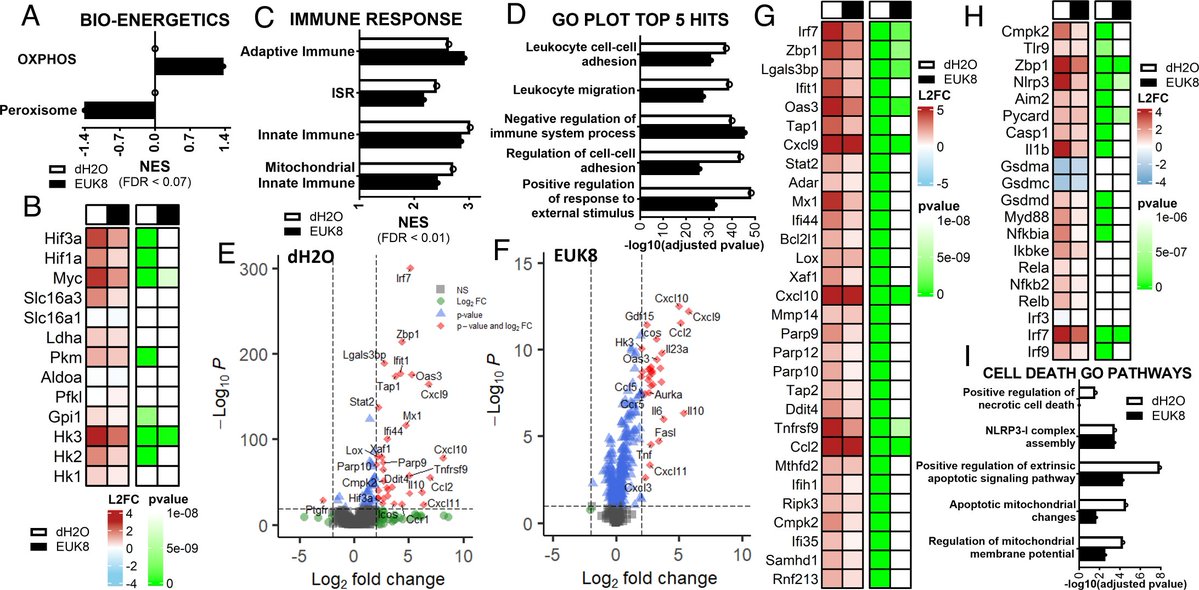
7) The figure 3 shows proteomic changes in the skull, meninges, and brain of COVID-19 patients and mice, revealing dysregulation of immune, inflammatory, and neurodegeneration-related pathways. https://t.co/Vvmctitapy
@ejustin46 - Emmanuel
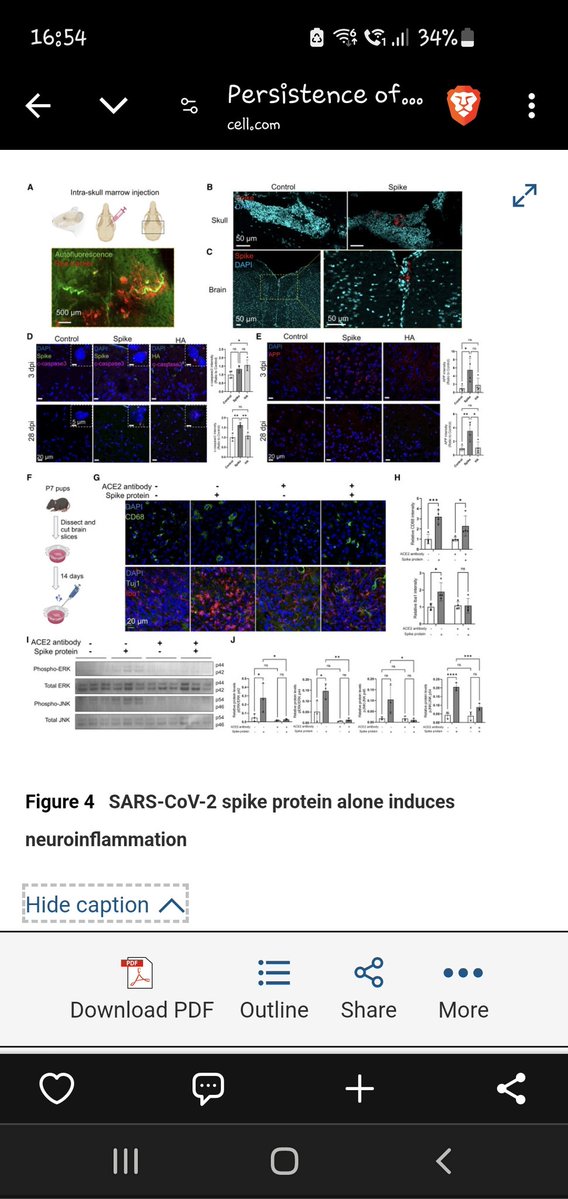
8) Figure 4 indicates that SARS-CoV-2 spike protein alone can induce neuroinflammation, neuronal stress, and anxiety-like behavior in mice, suggesting a direct role in COVID-19 neurological effects. https://t.co/yRULvUVjyy
@ejustin46 - Emmanuel
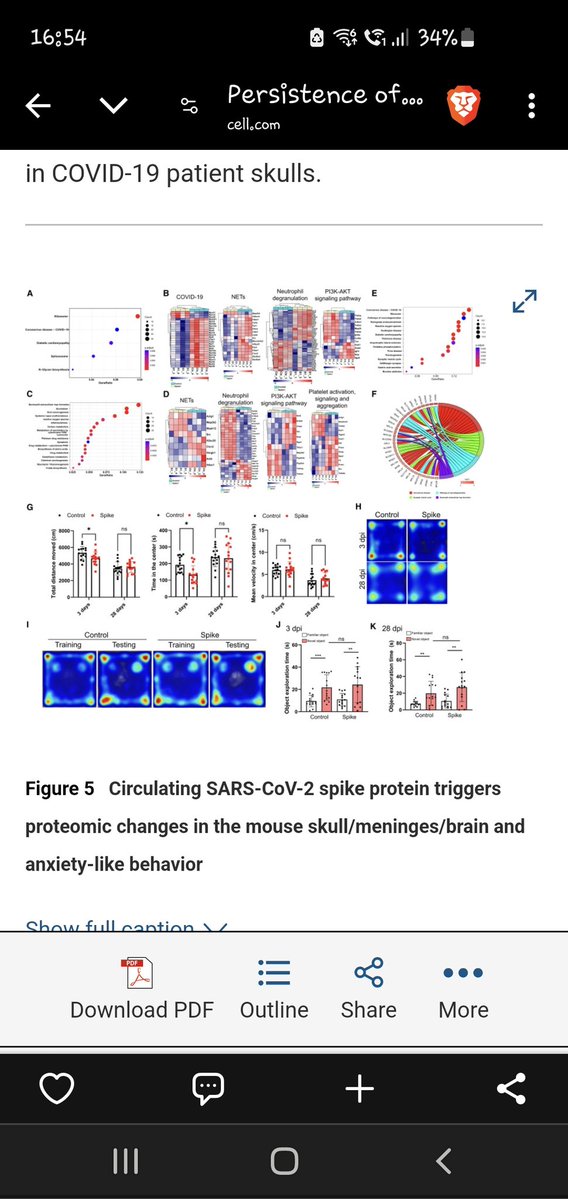
9) Figure 5 demonstrates that SARS-CoV-2 spike protein can cross the blood-brain barrier and accumulate in the brain, potentially contributing to neurological complications in COVID-19 patients. https://t.co/0owLskeyyM
@ejustin46 - Emmanuel
10) Figure 6 shows that SARS-CoV-2 spike protein disrupts the blood-brain barrier, allowing increased entry of immune cells and inflammatory factors into the brain, which may lead to neurological issues. https://t.co/5ZcsrcCe6c
@ejustin46 - Emmanuel
11) In conclusion, this study reveals that the SARS-CoV-2 spike protein can directly enter the brain, triggering neuroinflammation and neurological symptoms in COVID-19 patients. Thanks for reading 🙏 https://www.cell.com/cell-host-microbe/fulltext/S1931-3128(24)00438-4?utm_source=flipboard&utm_content=MickiKosman%2Fmagazine%2FCOVID-19+and+SARS-COV-2 https://t.co/hyShE5NFLW

@ejustin46 - Emmanuel
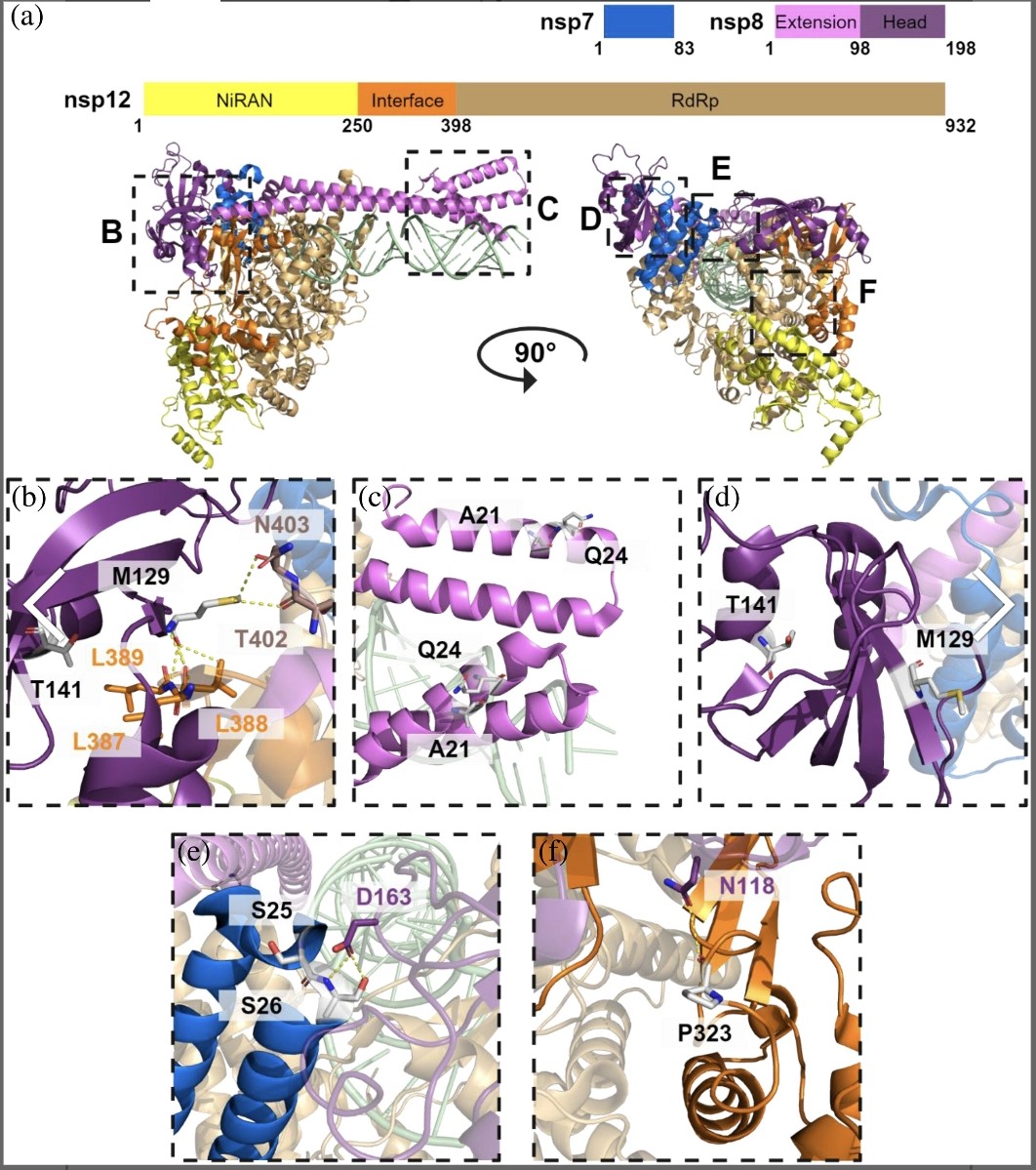
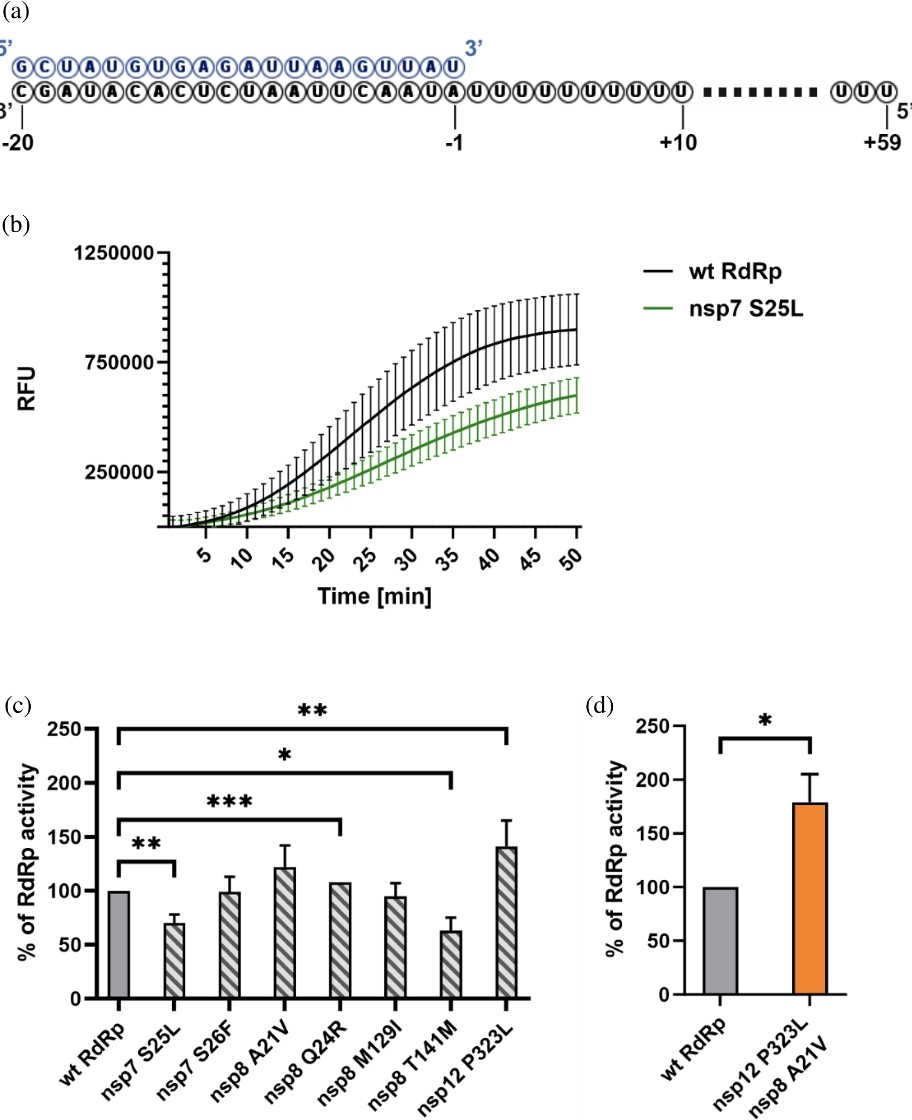
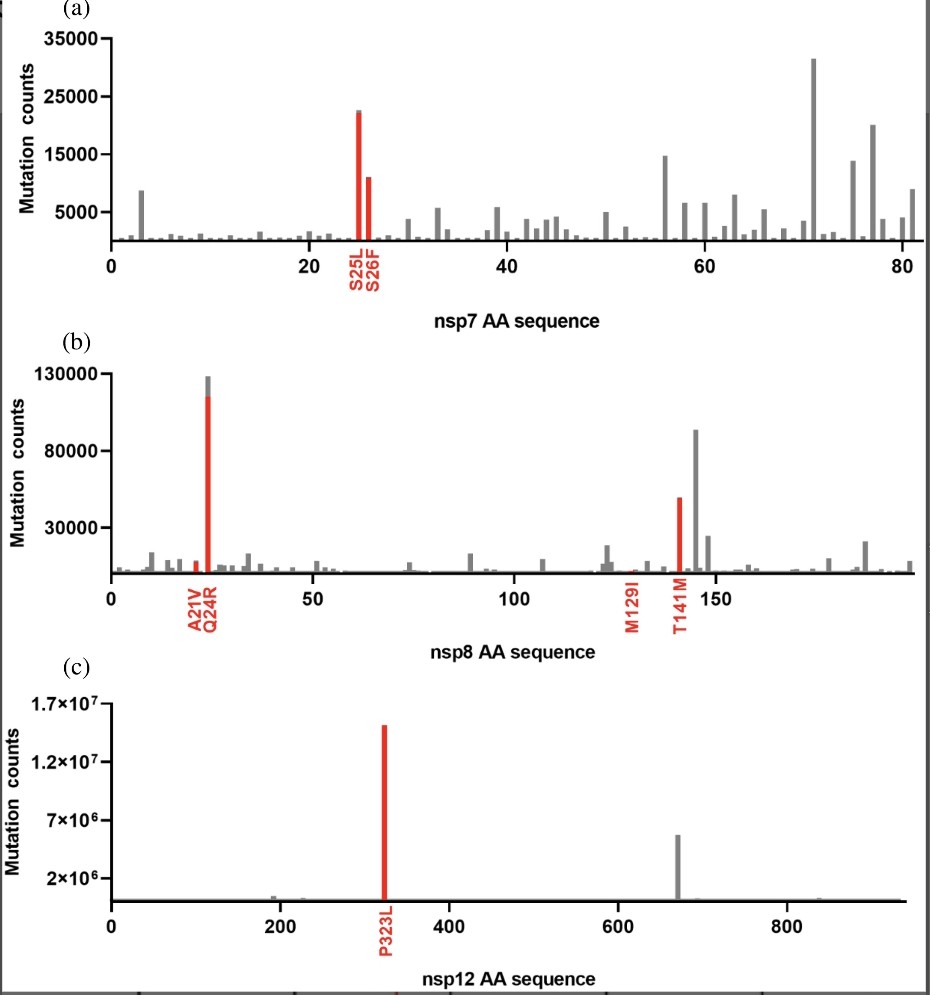
In the "jungle" of SARS-CoV-2 proteins : Phenotypic effects of substitutions in the three RdRp subunits: nsp7, nsp8, and nsp12 https://onlinelibrary.wiley.com/doi/10.1002/pro.5103 https://t.co/nW5AGLPqWy
@ejustin46 - Emmanuel
2) The study investigates the phenotypic effects of mutations in the RNA-dependent RNA polymerase (RdRp) of SARS-CoV-2, focusing on its three subunits: nsp7, nsp8, and nsp12. Despite RdRp being a key target for antiviral drugs, research on these mutations has been limited. https://t.co/sHw1XLcwY0
@ejustin46 - Emmanuel
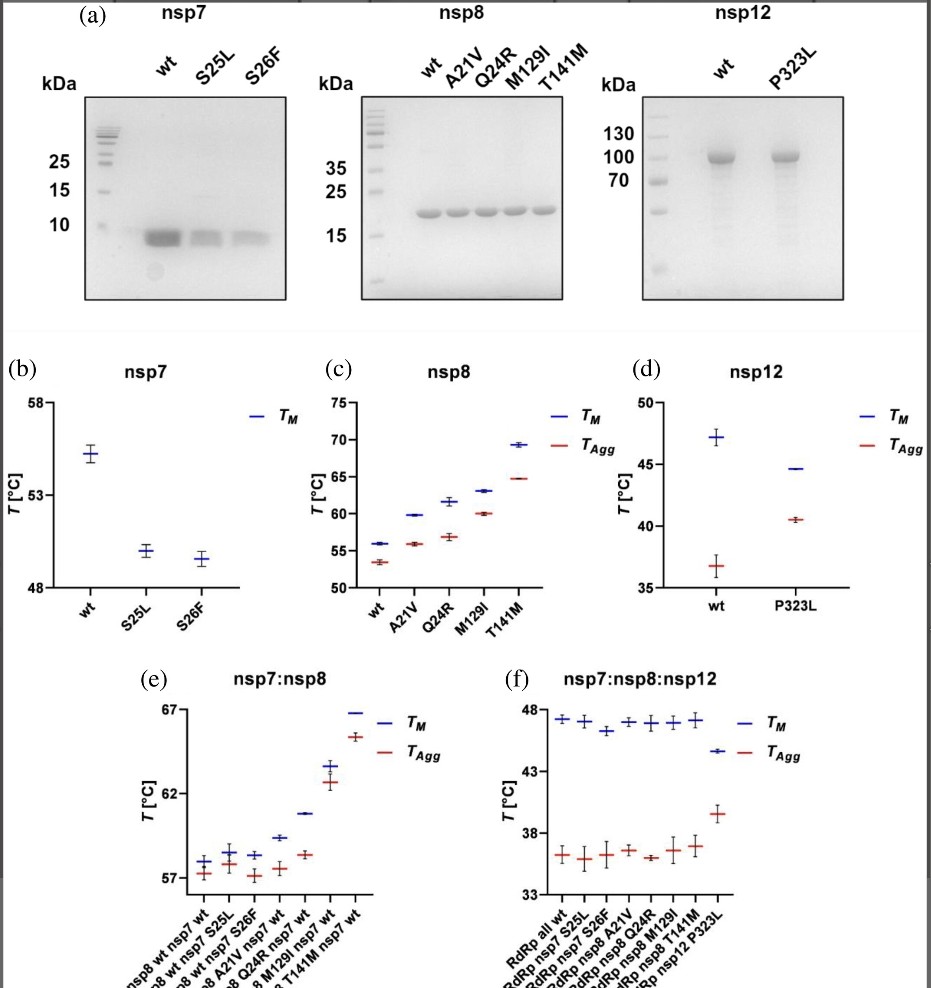
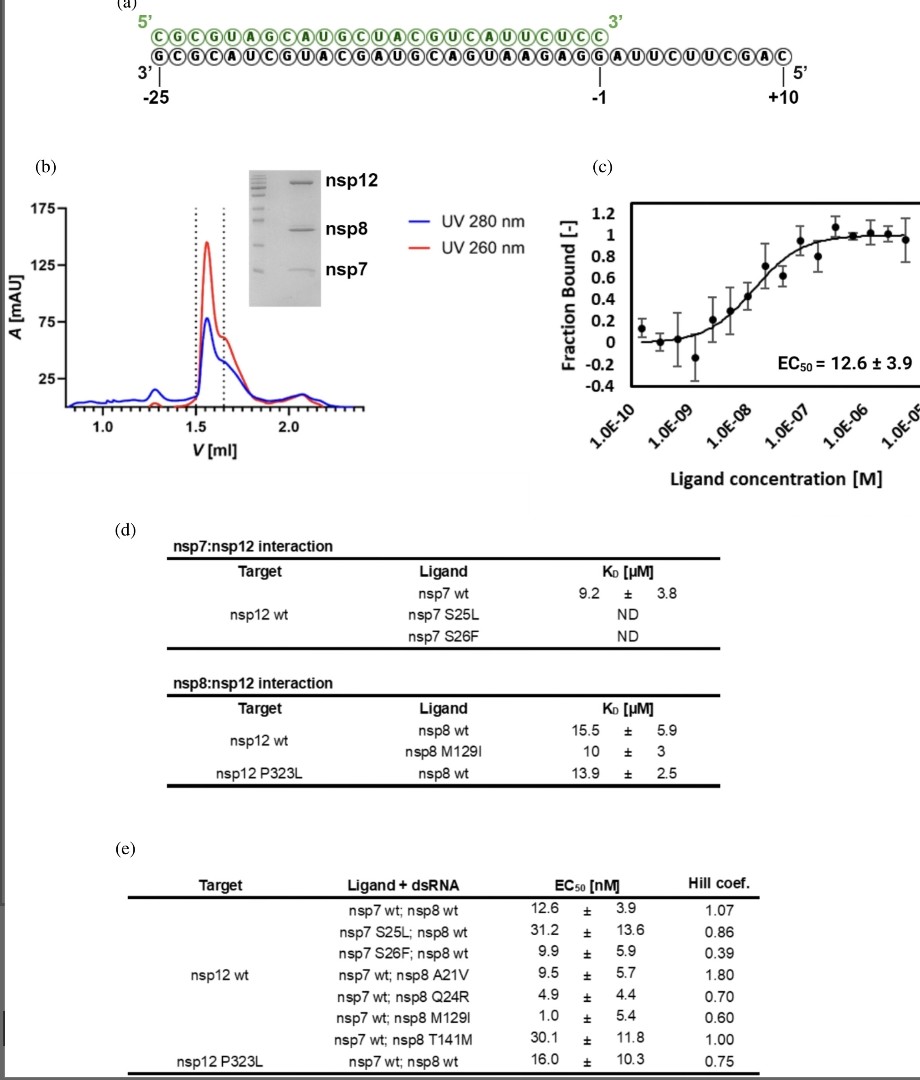
3) Using techniques like nano-differential scanning fluorimetry and microscale thermophoresis, the study assessed how mutations affected protein stability and RdRp complex assembly. https://t.co/sRSzkNVVCY
@ejustin46 - Emmanuel
4) Findings revealed that a mutation in nsp8 significantly increased its stability, while some mutations in nsp7 and nsp8 reduced their binding affinity to nsp12. Additionally, most mutations altered the overall RNA polymerase activity, often due to changes in stability or ... https://t.co/JeuLQEXGKq
@ejustin46 - Emmanuel
5) ...component affinity. Notably, a combination of mutations in nsp8 and nsp12 led to a 50% increase in polymerase activity. This research is the first to analyze the biochemical impact of amino acid mutations across the RdRp complex in emerging SARS-CoV-2 subvariants. Thanks🙏 https://t.co/D8qa1xQkz4


@ejustin46 - Emmanuel
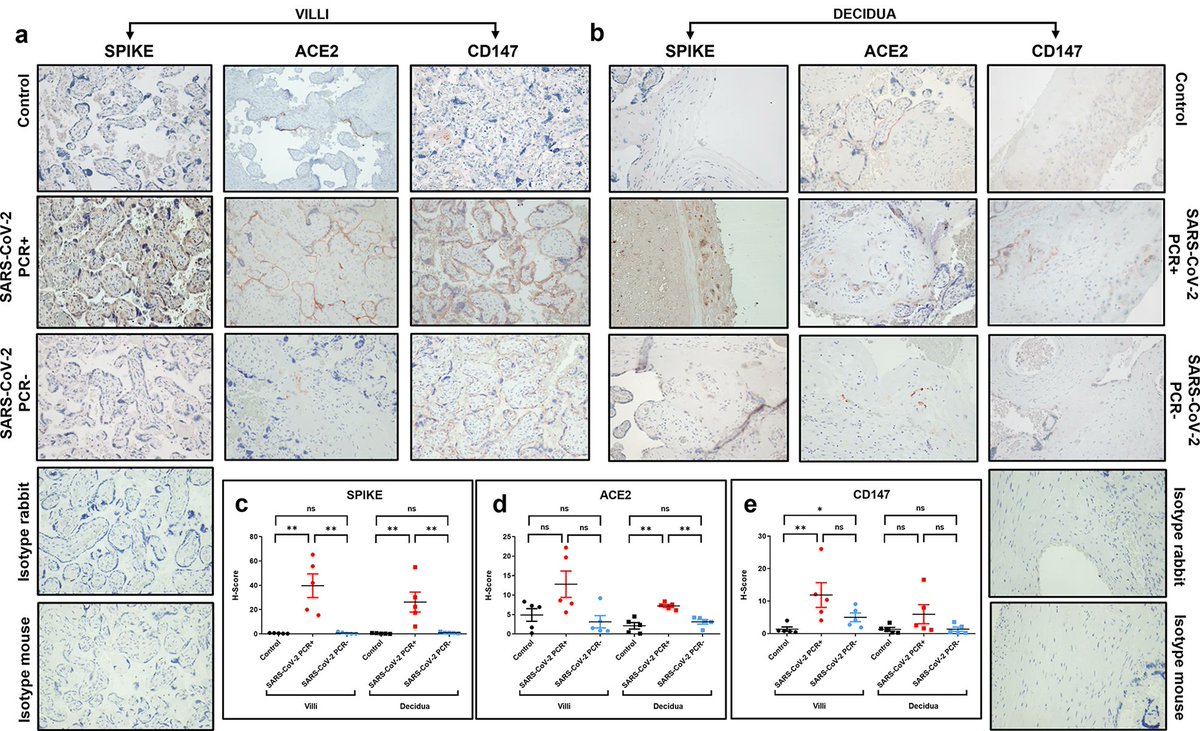
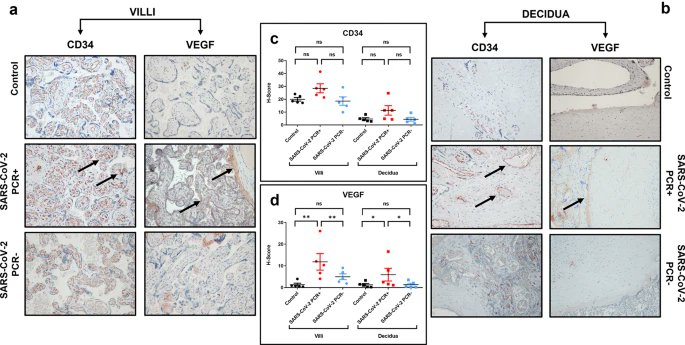
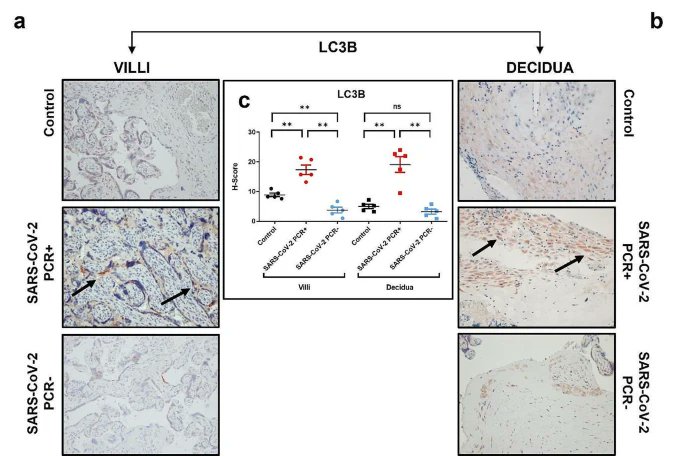
HOW SARS-COV-2 affects the PLACENTA ? 😰 https://link.springer.com/article/10.1007/s10735-024-10228-y

@ejustin46 - Emmanuel
2) This study examined how SARS-CoV-2 infection affects the placenta, the organ that connects the mother and fetus during pregnancy. The researchers analyzed placenta samples from three groups: women with active COVID-19 at delivery, women previously infected but ... https://t.co/FekacMWujQ
@ejustin46 - Emmanuel
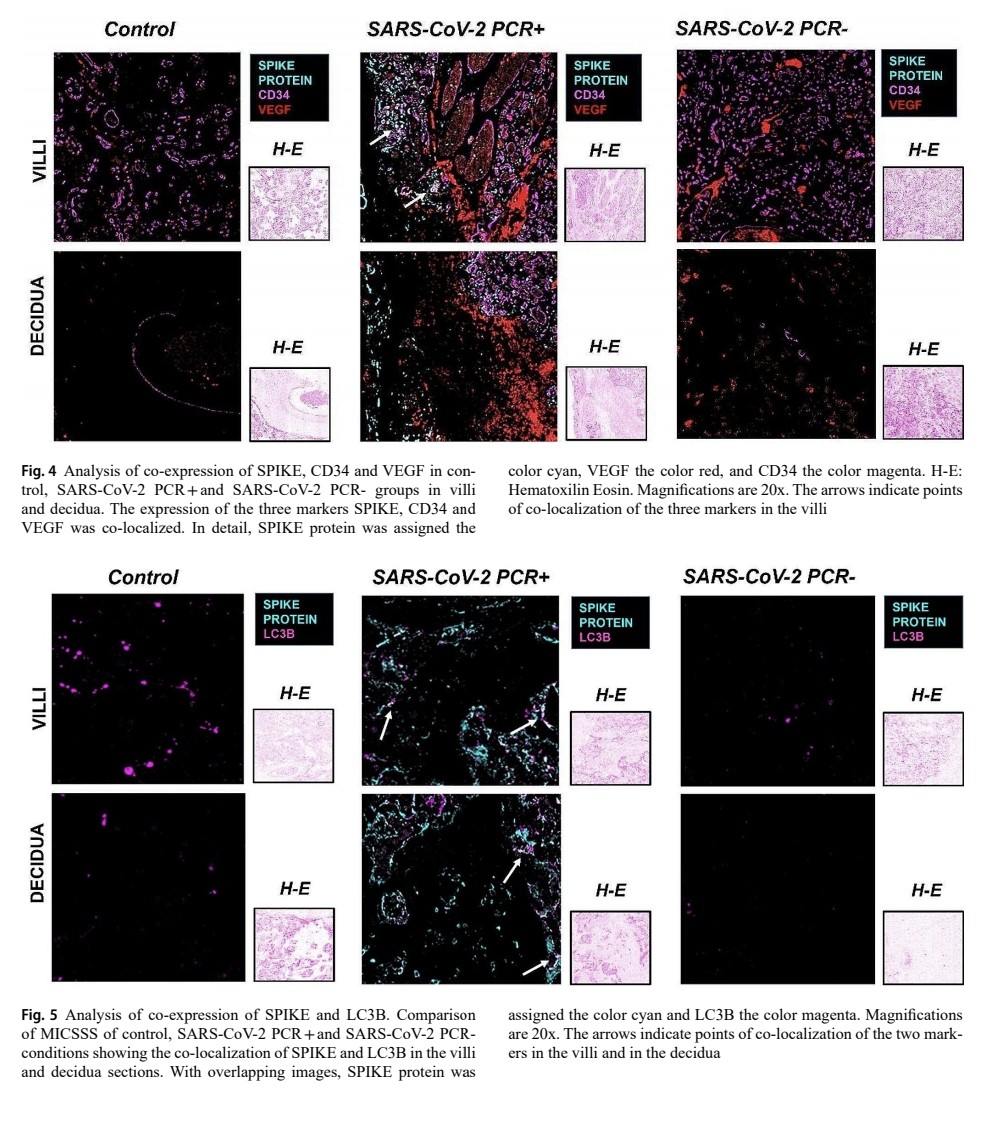
3) ...no longer positive, and uninfected controls. Key findings: - The SARS-CoV-2 spike protein was only detected in placentas of actively infected women. - Proteins that allow the virus to enter cells (ACE2, CD147) were increased in infected groups. https://t.co/lC2CYFwuMe
@ejustin46 - Emmanuel
4) - A growth factor called VEGF was higher in infected placentas, suggesting the virus disrupts normal placental blood vessels. - A marker of autophagy (cell self-cleaning) was elevated in active infection, but decreased after the virus cleared, indicating the placenta ... https://t.co/Ht1IiYPw55
@ejustin46 - Emmanuel
5) ...responds to the infection through this process. These results provide insights into how SARS-CoV-2 can impact the placenta and potentially affect maternal and fetal health during pregnancy.
@ejustin46 - Emmanuel
6) The findings highlight key molecular changes that occur both during active infection and after the virus is cleared. Thanks for reading 🙏 https://t.co/4D3nDaFKyg

@ejustin46 - Emmanuel
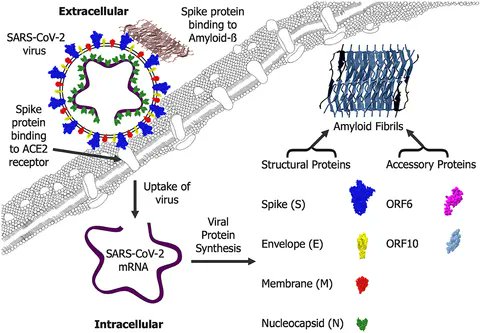
SARS-CoV-2 AMYLOID, is COVID-19-EXACERBATED DEMENTIA an amyloid disorder in the making? An interesting article 👍 https://www.frontiersin.org/journals/dementia/articles/10.3389/frdem.2023.1233340/full

@ejustin46 - Emmanuel
2) SARS-CoV-2 contains amyloid-forming proteins that could contribute to COVID-19-exacerbated dementias. The virus spike, nucleocapsid, and accessory proteins can aggregate into amyloid fibrils, which may interact with and promote deposition of endogenous amyloids like ...
@ejustin46 - Emmanuel
3) ...Aβ associated with Alzheimer's disease. COVID-19 may also indirectly impact the brain through hypoxia. Targeting SARS-CoV-2 amyloids could be a therapeutic approach, as vaccination may not reduce existing brain deposits. Thanks for reading 🙏

@ejustin46 - Emmanuel
AMAZING SARS-COV-2 ! The virus can ENTER and FUSE (leading to the creation of syncytia), using both RAFT-DEPENDENT (LIPID RAFT as CHOLESTEROL) and RAFT-INDEPENDENT pathways. Let me explain in simple terms...
@ejustin46 - Emmanuel
2) ACE2 lipid raft refers to the location of the ACE2 protein within the cell's membrane. Lipid rafts are specialized regions enriched in certain lipids like cholesterol. These lipid rafts can act as platforms that help viruses enter the cell.
@ejustin46 - Emmanuel
3) SARS-CoV-2 has different ways it can get into the cell. It can use: - Raft-dependent pathway using the lipid raft regions of the cell membrane to enter. - Raft-independent pathway, finding other ways to get into the cell that don't involve the lipid rafts.
@ejustin46 - Emmanuel
4) In the case of SARS-CoV-2, the virus is able to use both of these pathways. So the virus has flexibility in how it can infect the cell, it's not completely dependent on the lipid rafts. This is what they showed in this wonderful study https://www.biorxiv.org/content/10.1101/2024.07.13.603361v1

@ejustin46 - Emmanuel
5) For enthusiasts, I highly recommend reading the abstract of this study which is very clear and explicit. Thanks for reading 🙏 https://t.co/C1DQEBDkX6

@ejustin46 - Emmanuel
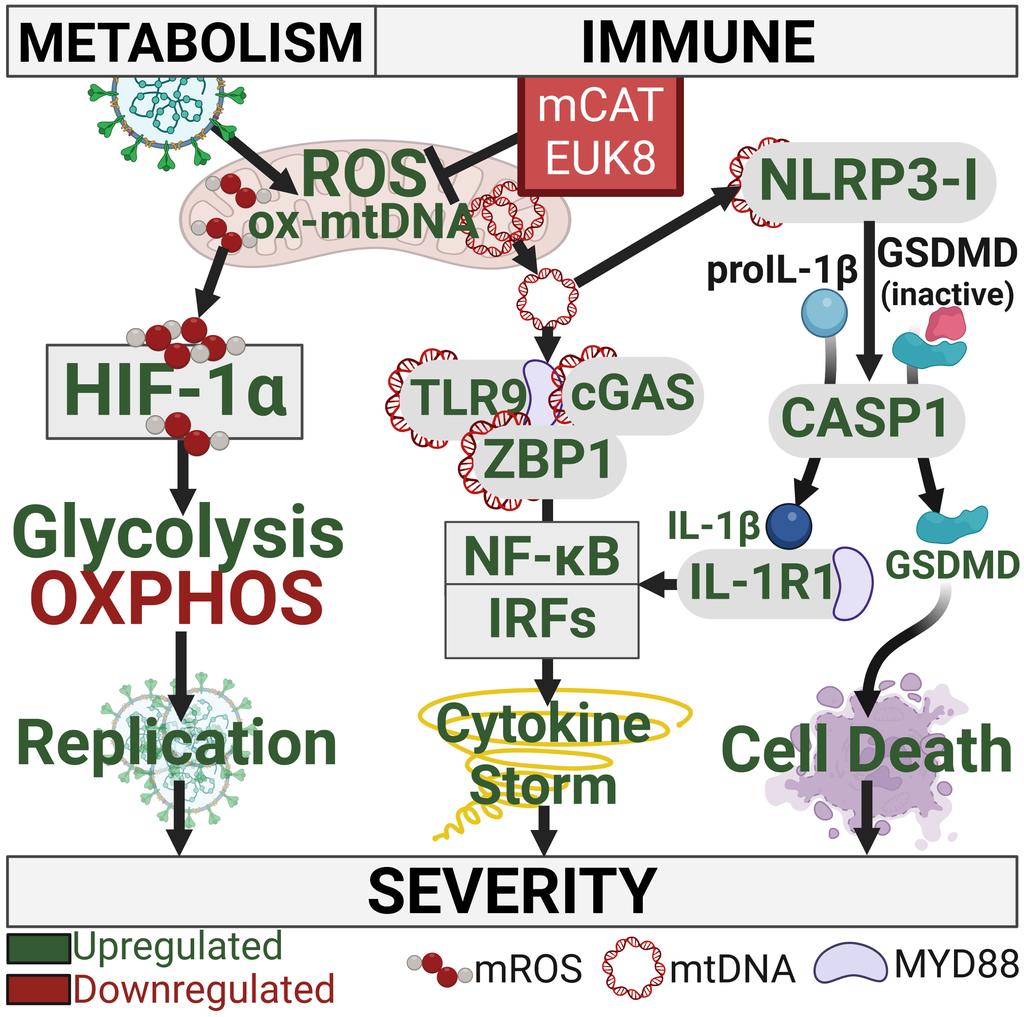
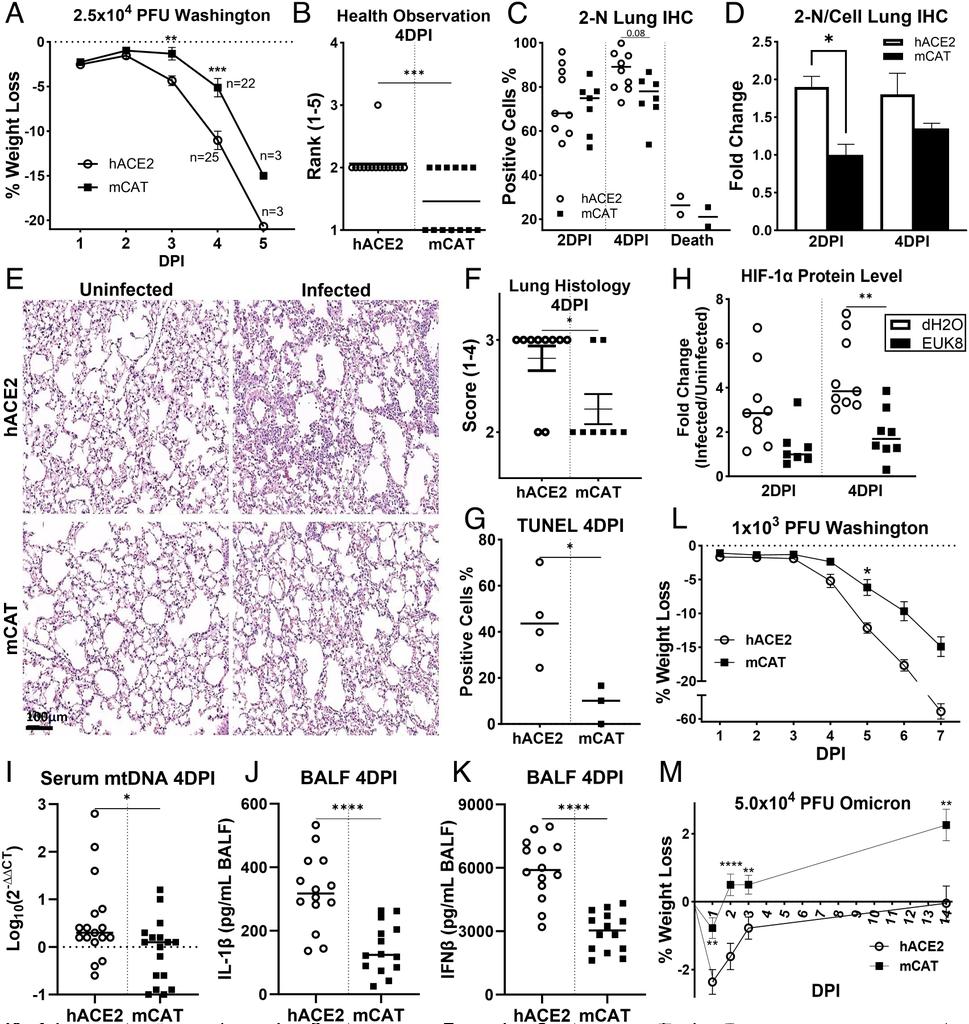
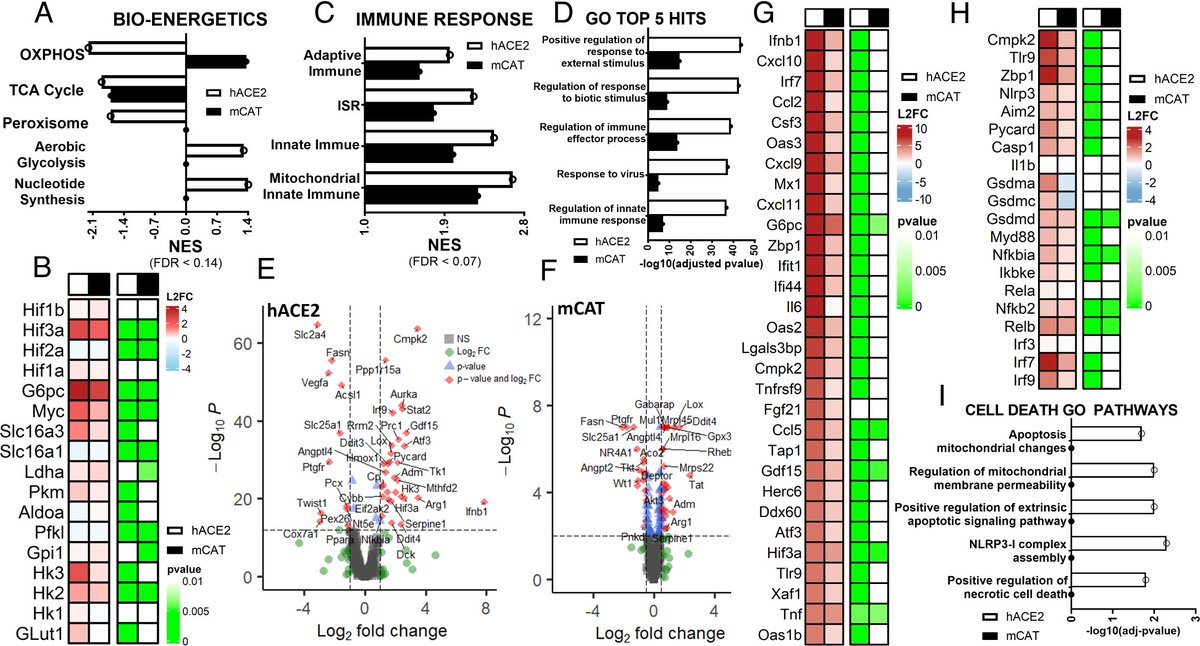
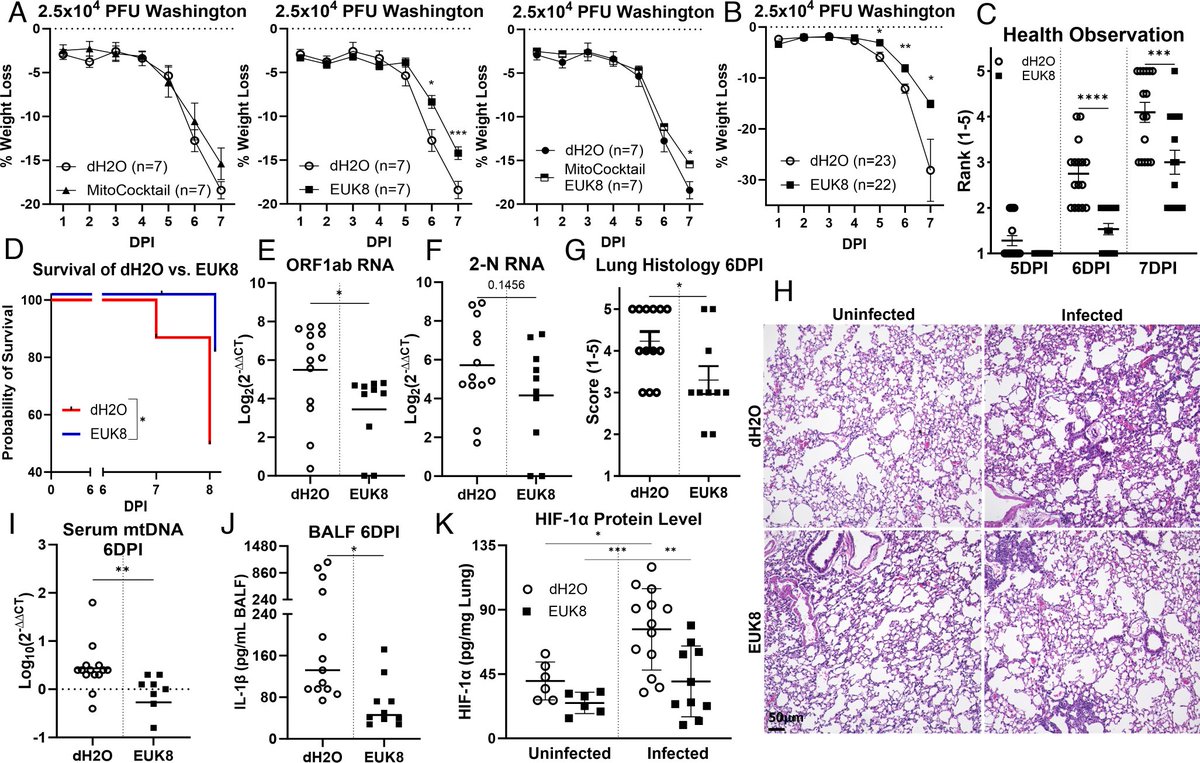
How SARS-CoV-2 INFECTION DISRUPTS the NORMAL FUNCTIONING of MITOCHONDRIA, the powerhouses of cells ? https://www.pnas.org/doi/10.1073/pnas.2321972121 https://t.co/twQRVLNTrC
@ejustin46 - Emmanuel
2) The SARS-COV-2 infection leads to an increase in harmful reactive oxygen species produced by mitochondria. These reactive oxygen species then activate a protein called HIF-1α, which causes the cell to switch its energy production from ... https://t.co/5OezhuWg6I
@ejustin46 - Emmanuel
3) ... efficient mitochondrial respiration to less efficient glycolysis. This metabolic shift benefits the virus by providing more building blocks for viral replication. https://t.co/ps6H3T8jya
@ejustin46 - Emmanuel
4) The increased reactive oxygen species also cause mitochondrial DNA to leak out of the mitochondria into the cell, triggering inflammatory pathways that can damage the lungs and other organs. https://t.co/m1qJyhznhv
@ejustin46 - Emmanuel
5) To counteract these harmful effects of SARS-CoV-2, the researchers used genetic and pharmacological approaches to increase the cell's antioxidant defenses by boosting mitochondrial catalase, an enzyme that neutralizes reactive oxygen species. https://t.co/EYmv0z2aBJ
@ejustin46 - Emmanuel
6) This mitochondrial antioxidant therapy was able to reverse the metabolic changes, reduce inflammation, and protect mice from severe COVID-19 disease. Thanks for reading 🙏
@ejustin46 - Emmanuel
7) For a great reading, we recommend also the thread of @vipintukur We posted this study together and at the same time 🤗 https://t.co/L44sPkrv4W

@ejustin46 - Emmanuel
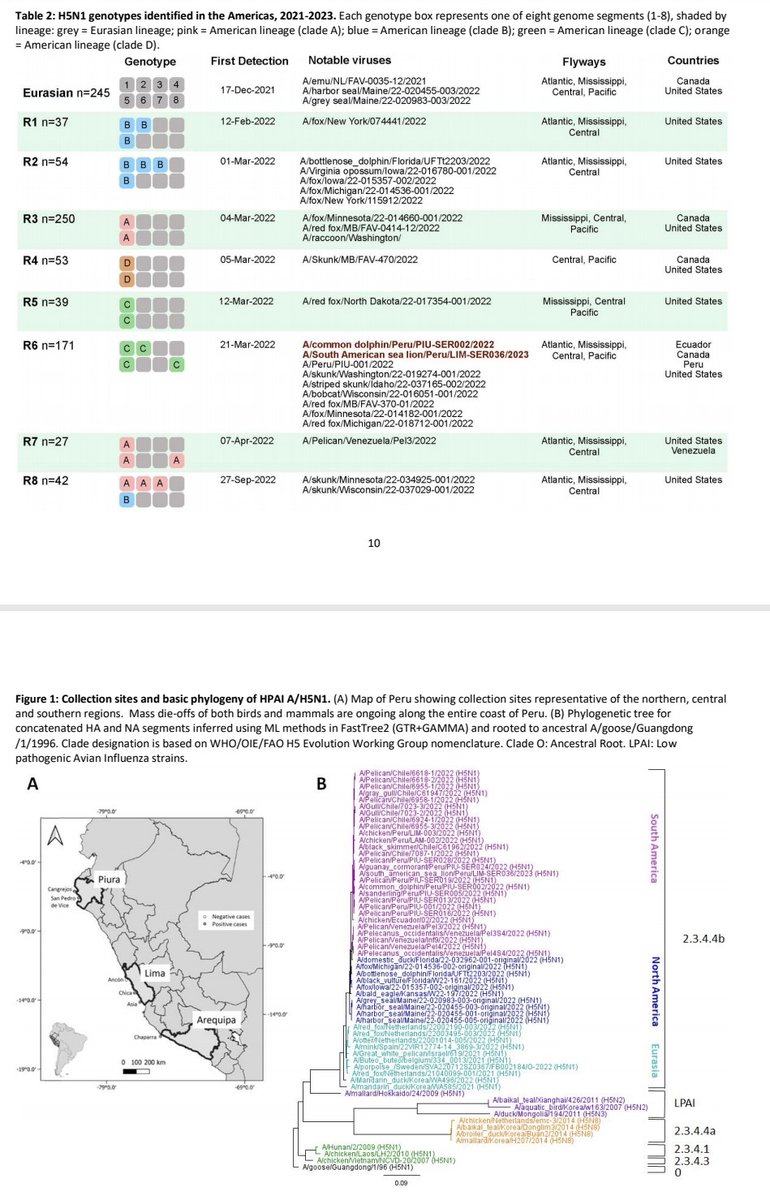
STOP H5N1 influenza in US cattle NOW !!! An excellent article in Science https://www.science.org/doi/10.1126/science.adr5866 https://t.co/tLpe40vHMV
@ejustin46 - Emmanuel
2) This article stresses the importance of practical steps to prevent the spread of zoonotic influenza. It calls for enhanced surveillance, timely vaccine development, global data sharing, improved analysis, optimized detection of human infection clusters. We highly recommend it

@ejustin46 - Emmanuel
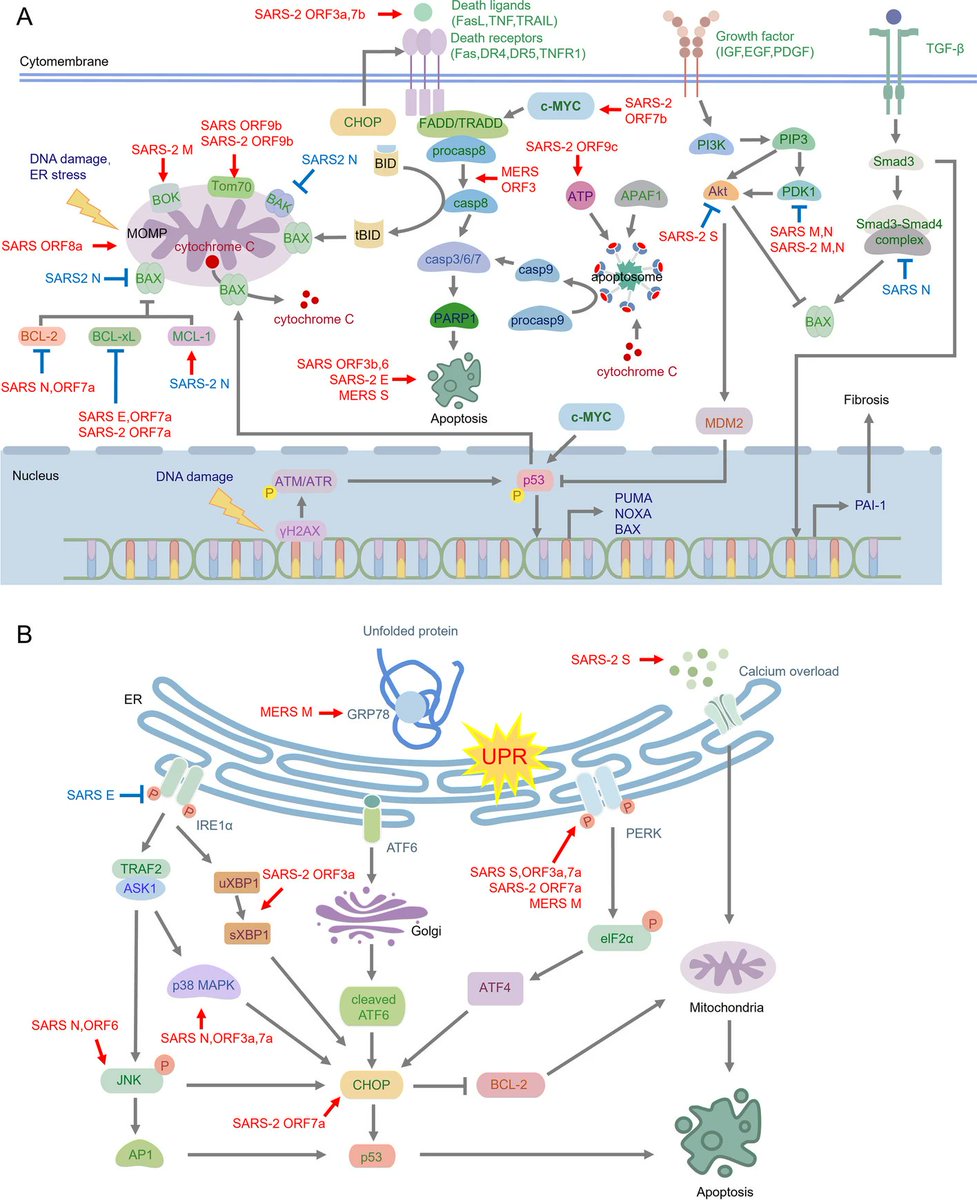
A glimpse into VIRAL WARFARE: decoding the INTRIGUING ROLE of HIGHLY PATHOGENIC CORONAVIRUS PROTEINS in APOPTOSIS REGULATION https://jbiomedsci.biomedcentral.com/articles/10.1186/s12929-024-01062-1

@ejustin46 - Emmanuel
2) Highly contagious coronaviruses like SARS-CoV-2 can trigger a process called apoptosis, or programmed cell death, in the body. This helps the virus spread and avoid the immune system. Compared to less harmful coronaviruses ... https://t.co/qptO8k8dCf
@ejustin46 - Emmanuel
3) ...the dangerous ones have more proteins that can induce apoptosis through different pathways. This damages lung cells, immune cells, and other organs, making people sicker. The spike, envelope, membrane, and nucleocapsid proteins of these viruses ... https://t.co/H7pW25mjPY
@ejustin46 - Emmanuel
4) ...disrupt normal cell functions, leading to apoptosis. Viral non-structural proteins also play a key role, suppressing immune responses and promoting viral replication. Severity of COVID-19 is linked to higher levels of apoptosis.
@ejustin46 - Emmanuel
5) In summary, apoptosis is a critical part of how dangerous coronaviruses infect and harm the body. Targeting this process may be an important strategy for fighting these viruses and other diseases. Thanks for reading 🙏

@ejustin46 - Emmanuel
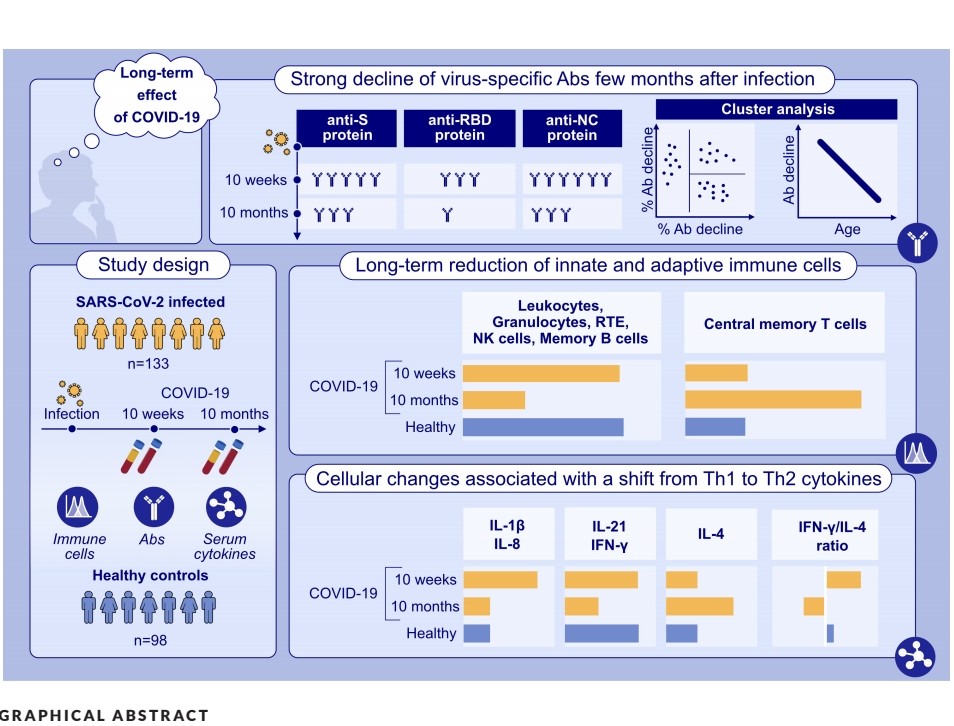
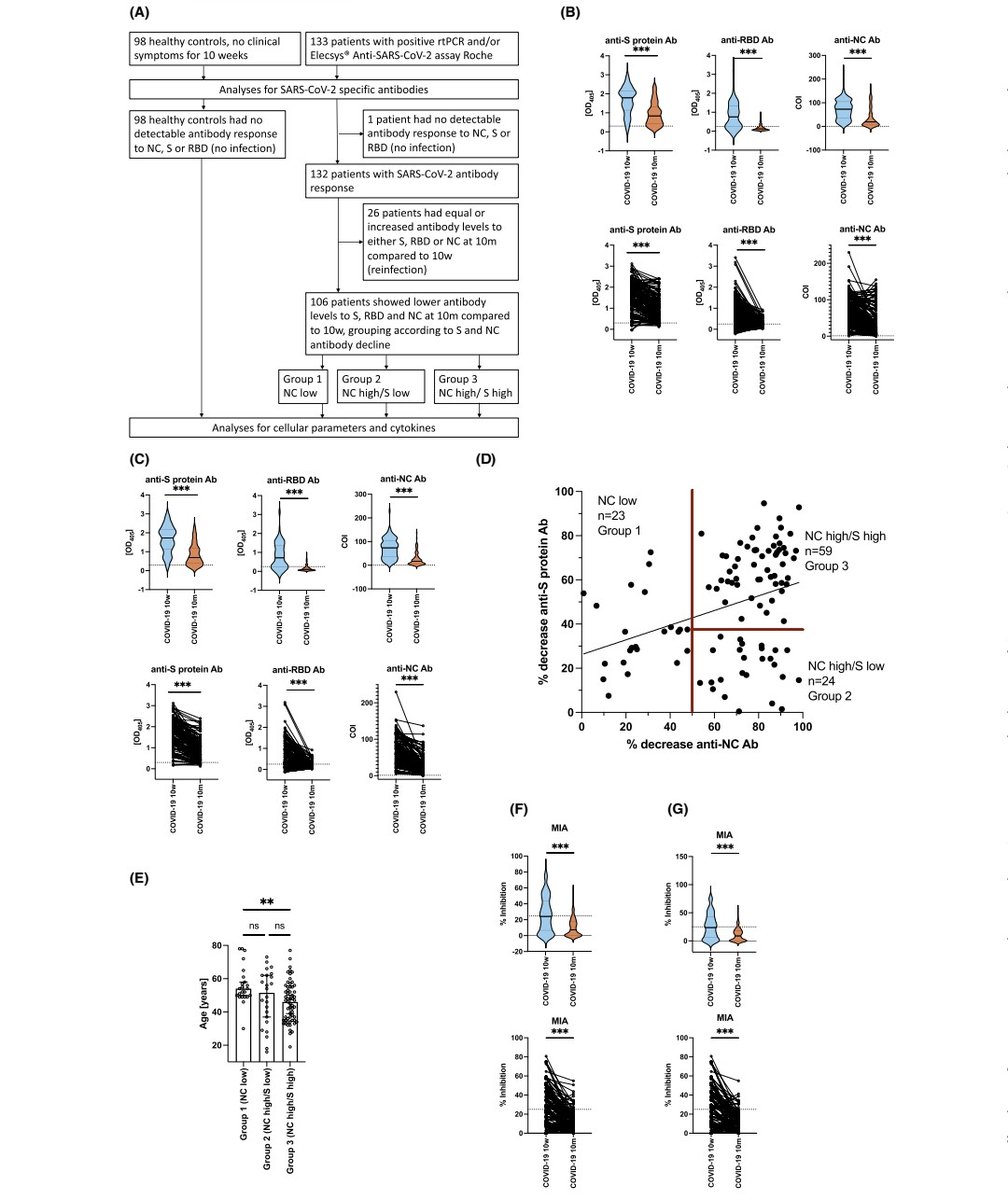
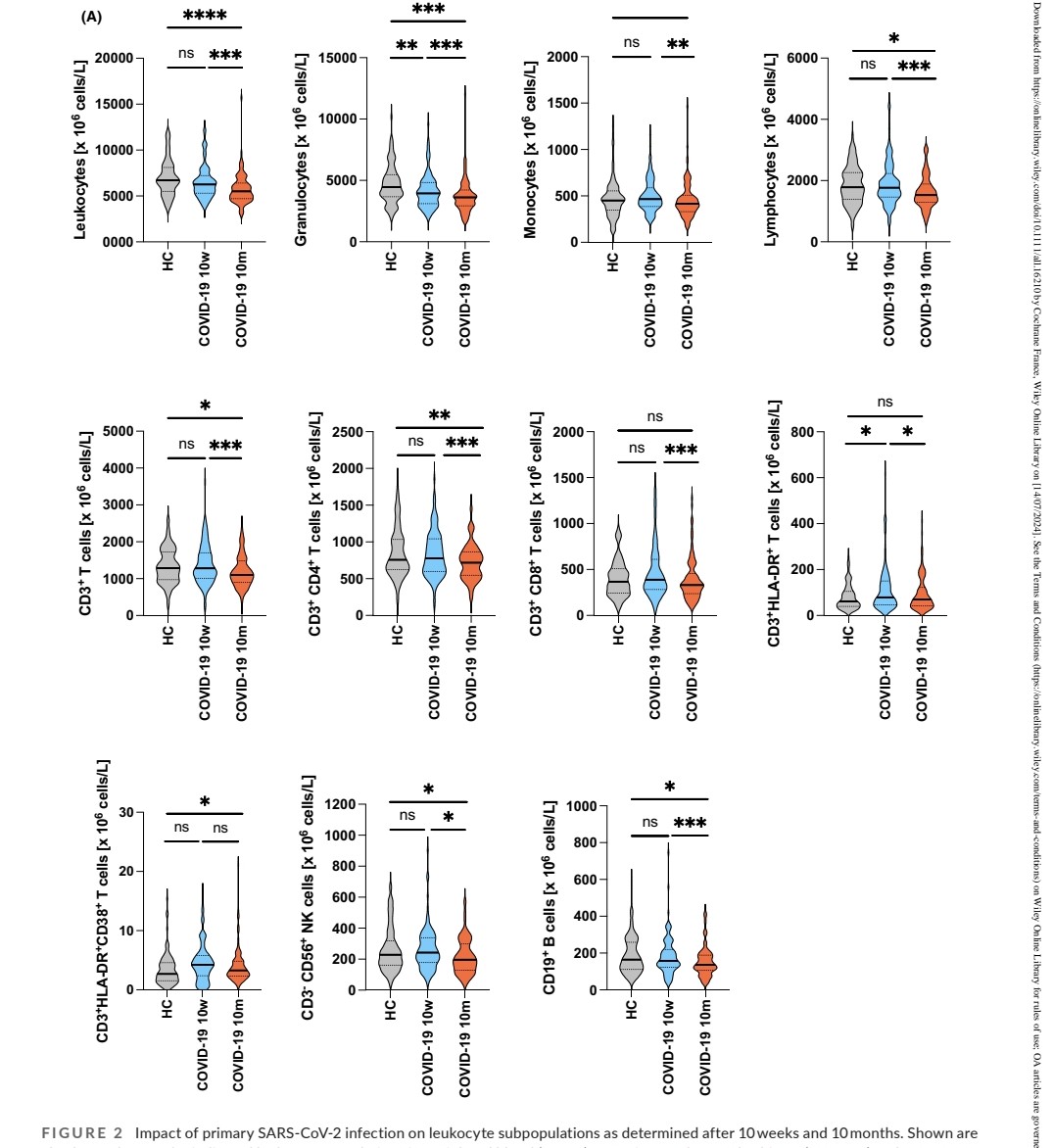
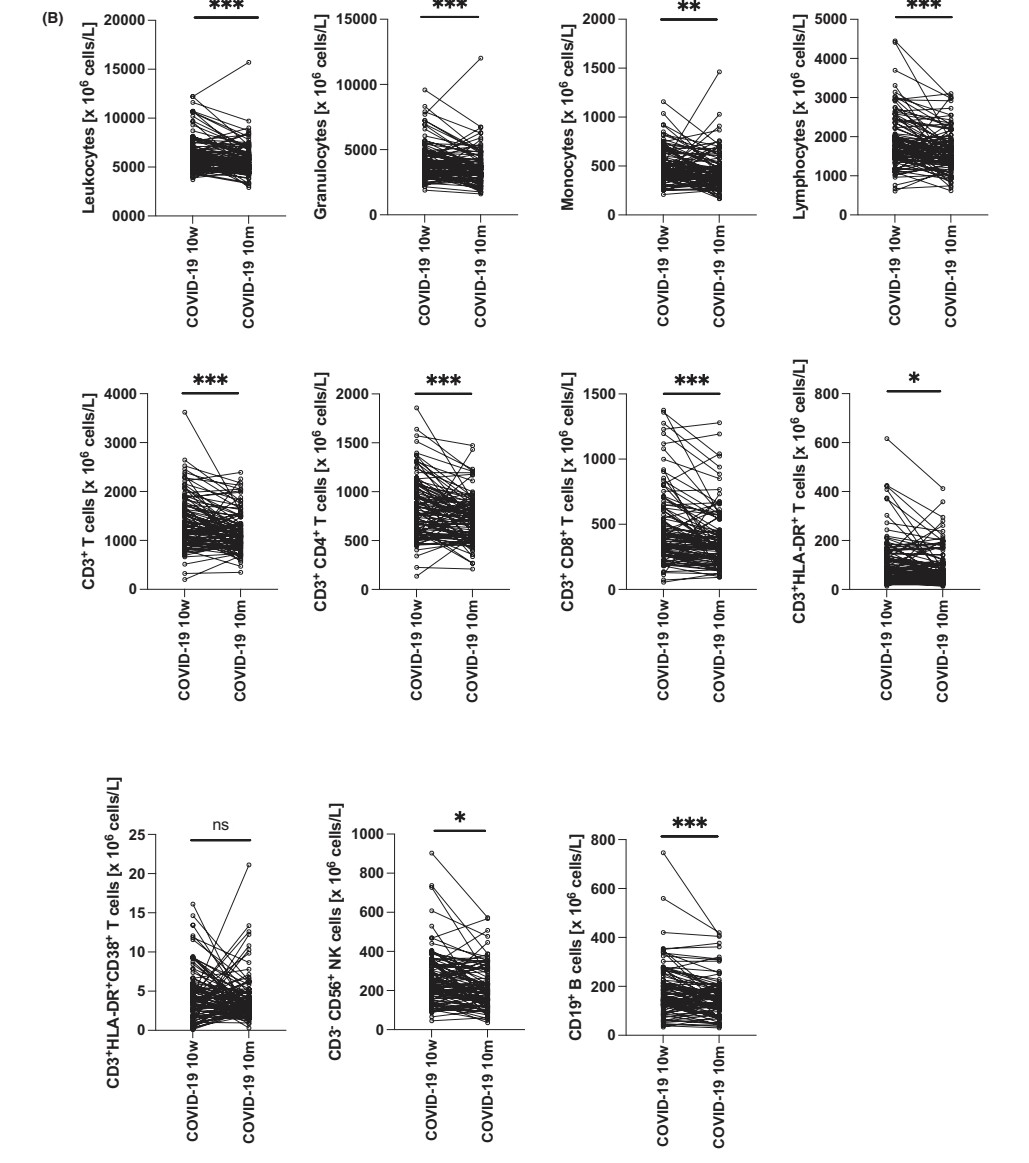
A FEW MONTHS AFTER a single INFECTION, ALL PROTECTIONS DECLINE : antibody levels, innate and adaptive immune cells plus a shift from Th1/inflammatory to Th2 serum cytokine levels #AvoidReinfection https://onlinelibrary.wiley.com/doi/10.1111/all.16210
@ejustin46 - Emmanuel
2) This study investigated the long-term effects of a single COVID-19 infection on the immune system. Even 10 months later, the researchers found significant changes in patients' immune cells and antibodies. https://t.co/VeEjH9GvID
@ejustin46 - Emmanuel
3) Patients had reduced levels of various immune cells, including those that fight infections. Their antibody levels against the virus also dropped substantially over time. The immune system also shifted from a pro-inflammatory state to one focused on allergic responses. https://t.co/MT714DGsv9
@ejustin46 - Emmanuel
4) Younger patients tended to have a more pronounced decline in certain antibodies. These immune changes may help explain the diverse long-term symptoms experienced by some COVID-19 patients, known as "long COVID." https://t.co/zkgYbRr43a
@ejustin46 - Emmanuel
5) The study suggests that the initial COVID-19 infection can have a lasting impact on the body's ability to defend itself. This could make people more susceptible to future infections or other health issues. Thanks 🙏 https://t.co/Q9hhJlkq6Y

@ejustin46 - Emmanuel
E (envelope) PROTEIN. HOW COULD I HAVE MISSED THIS? 🤦♂️🤦♂️🤦♂️ For 2 years, I repeated in a multitude of threads, that the E-protein was for SARS-COV-2, a major protein, just as important as Spike. But I missed a link about this protein. (AI abstract image generated)
@ejustin46 - Emmanuel
2) The E:T9I was one of the key mutation of this pandemic, reducing the pathogenicity of the Omicrons but allowing them at the same time to escape autophagy, which has contributed to their emergence and spread by evading the innate immune defense.
@ejustin46 - Emmanuel
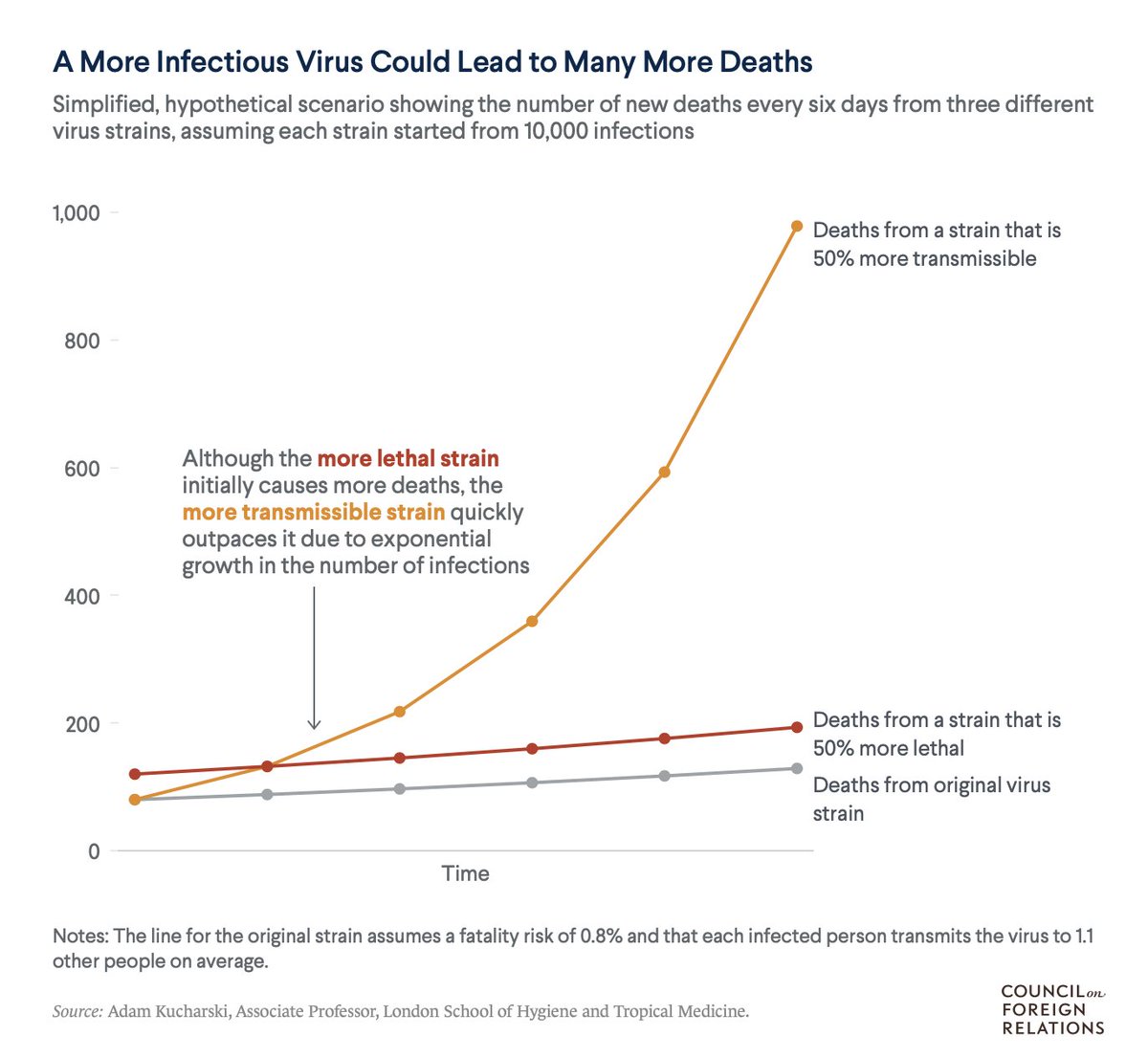
3) Hence the confusion about an Omicron "milder" when a less pathogenic but more transmissible virus is much more dangerous.
@ejustin46 - Emmanuel
4) The E protein acts also as an ion channel (viroporin), which allows ions to pass through the viral membrane, helping the virus replicate and evade the host immune response, playing a crucial role in virus entry and release
@ejustin46 - Emmanuel
5) If the E protein had a dual effects on the Omicron variant, reducing its pathogenicity but also increasing its infectivity, this small protein, acting as an ion channel is also involved in the depletion of cells and neuron apoptosis.
@ejustin46 - Emmanuel
6) While some mentioned the "rise" of Omicrons from the lower respiratory tract (lung) to the upper tract (nasal, throat), in fact the virus was traveling much higher towards the brain. The disease became more neurological than pulmonary.
@ejustin46 - Emmanuel
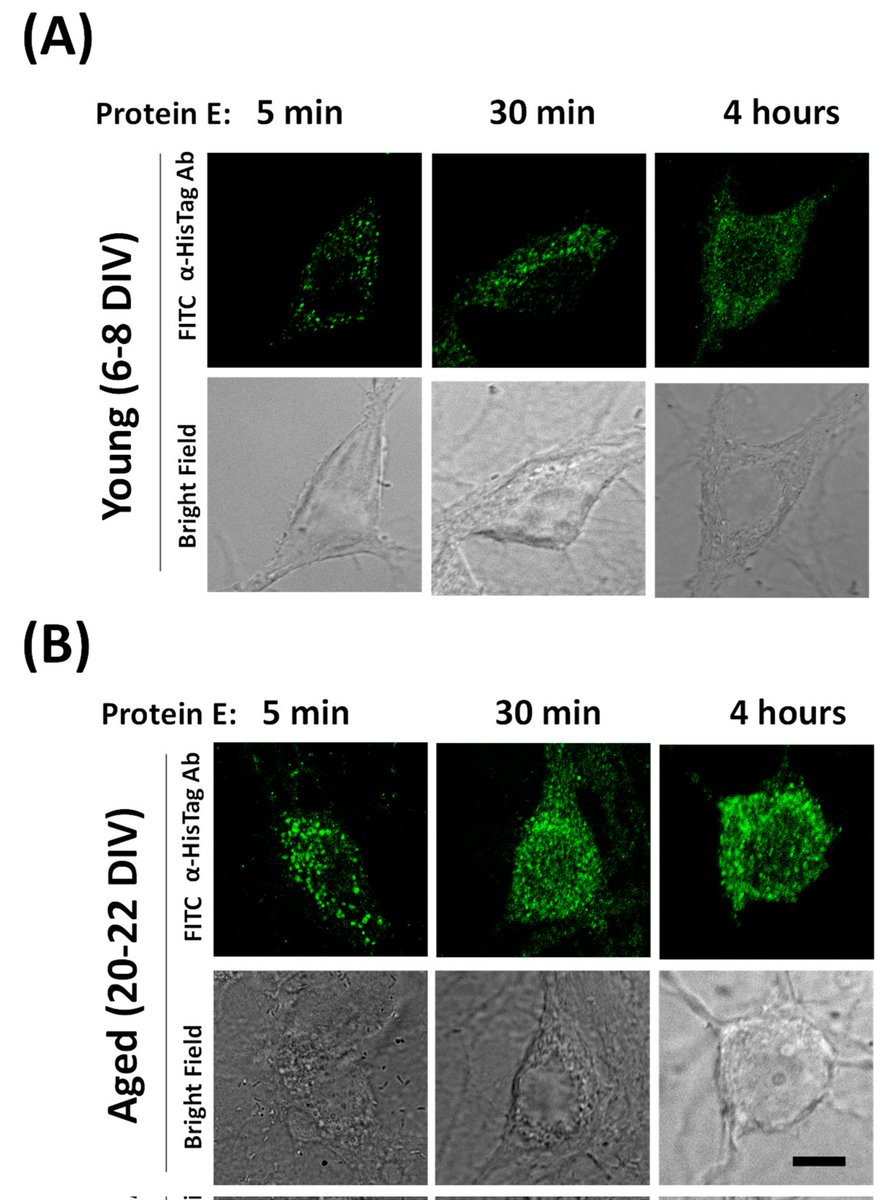
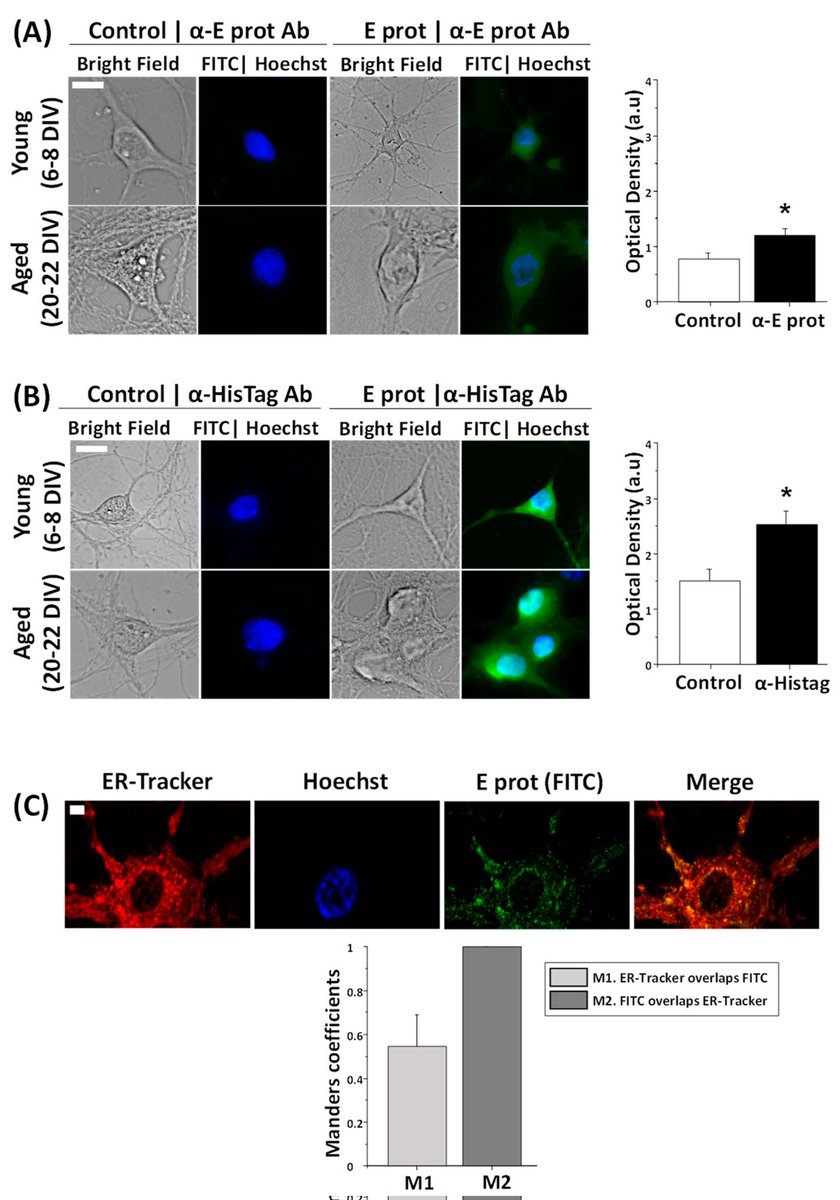
7) What alerted me to this evolution of this protein and allowed me to understand these changes, was this recently published study. https://www.mdpi.com/1422-0067/25/12/6304 They looked at how the E protein affects calcium levels and cell survival in hippocampal neurons from rats.

@ejustin46 - Emmanuel
8) The main findings are: ▶️ The E protein quickly gets inside hippocampal neurons and attaches to the endoplasmic reticulum (ER), which is like the cell's storage compartment. ▶️ The E protein causes older hippocampal neurons (20-22 days in the lab) to die, but ... https://t.co/Btgf3Fc1Y4
@ejustin46 - Emmanuel
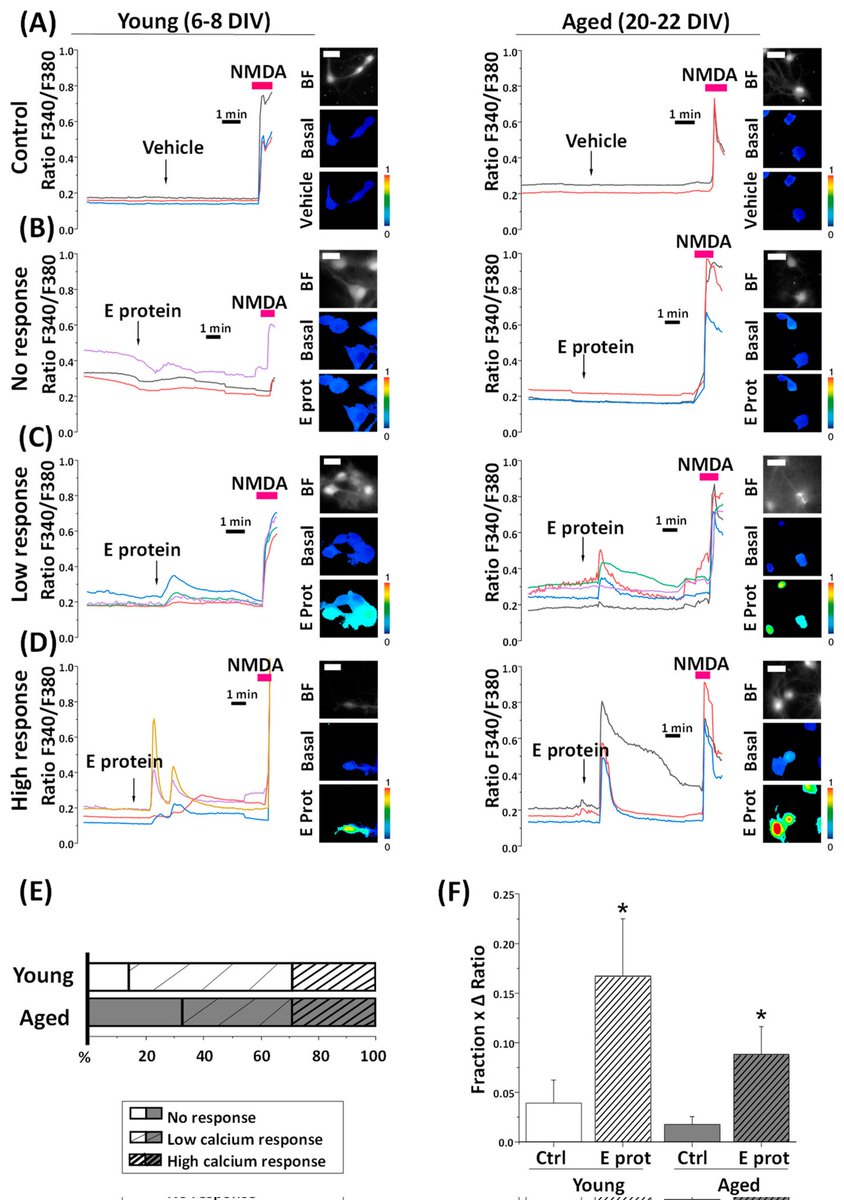
9) ...doesn't kill younger neurons (6-8 days). ▶️ The E protein makes calcium levels inside the hippocampal neurons go up and down in different ways. Older neurons have much bigger changes in calcium levels compared to younger neurons. https://t.co/UwT6zHj4cm
@ejustin46 - Emmanuel
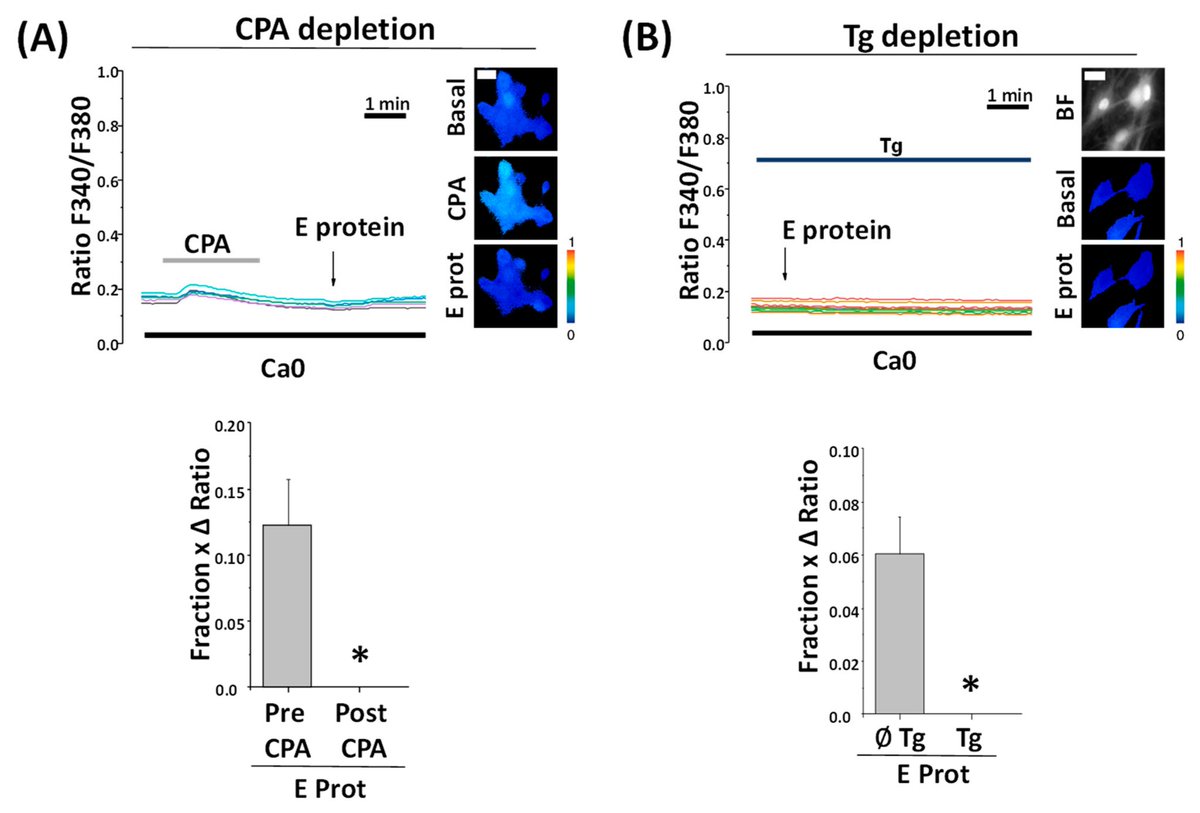
10)▶️ When the calcium stores in the ER are emptied out, the E protein can no longer affect calcium levels. This shows the E protein is releasing calcium from the ER. ▶️ The E protein moves into the ER membranes very quickly, which matches how fast it starts changing calcium and https://t.co/fWqQ1gN5lN
@ejustin46 - Emmanuel
11) ...killing the older neurons. In summary, the SARS-CoV-2 E protein can get inside hippocampal neurons, disrupt their calcium regulation in the ER, and selectively cause older neurons to die. This helps explain how SARS-CoV-2 proteins may contribute to brain problems. https://t.co/6CyJtpE2Bx
@ejustin46 - Emmanuel
12) From a less pathogenic mutation which in fact contributes to an increase of the transmissibility, to this protein capable of killing neurons, we are definitely not finished with the envelope protein and more generally with this SARS-COV-2 virus. Thanks for reading 🙏 https://t.co/sEJf04WfOG

@ejustin46 - Emmanuel
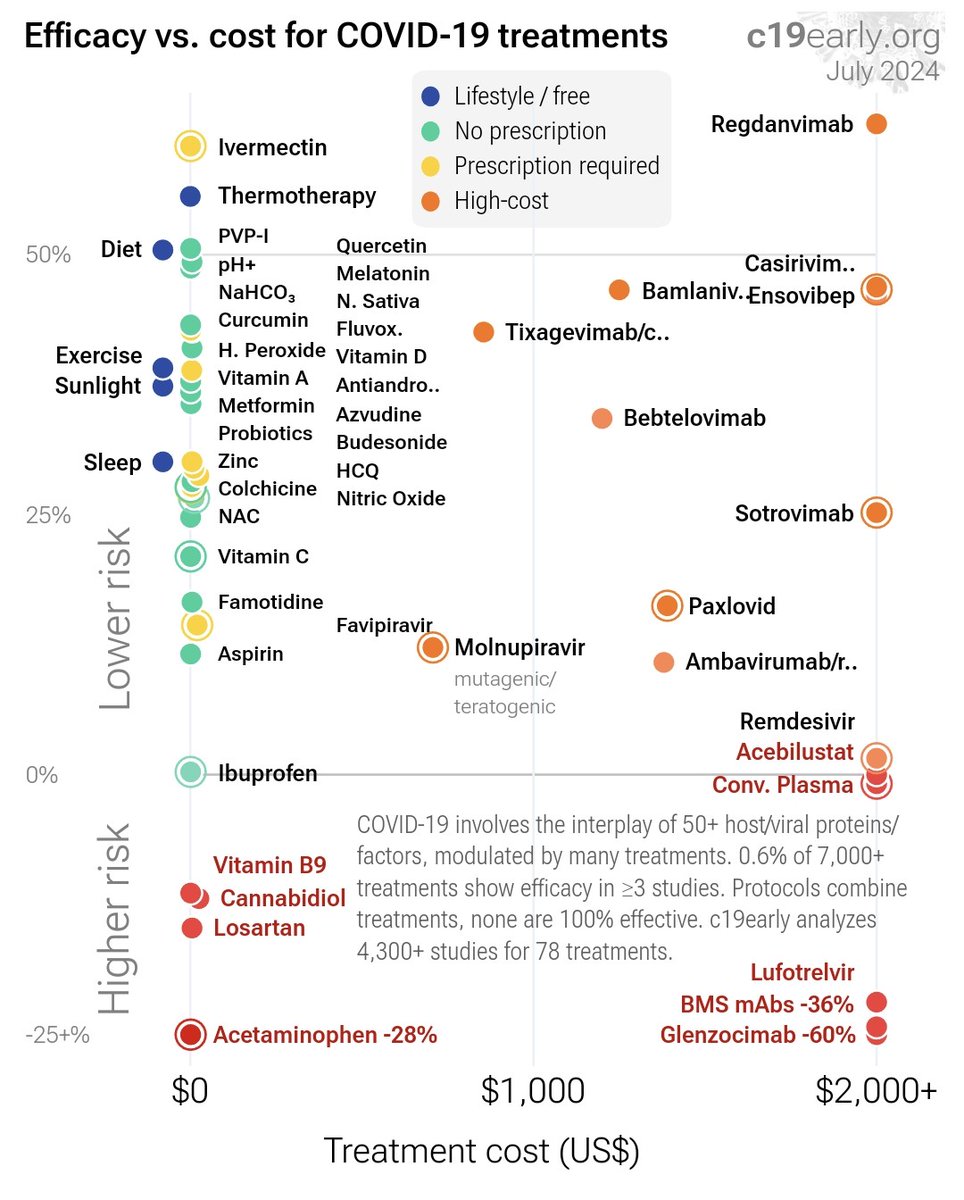
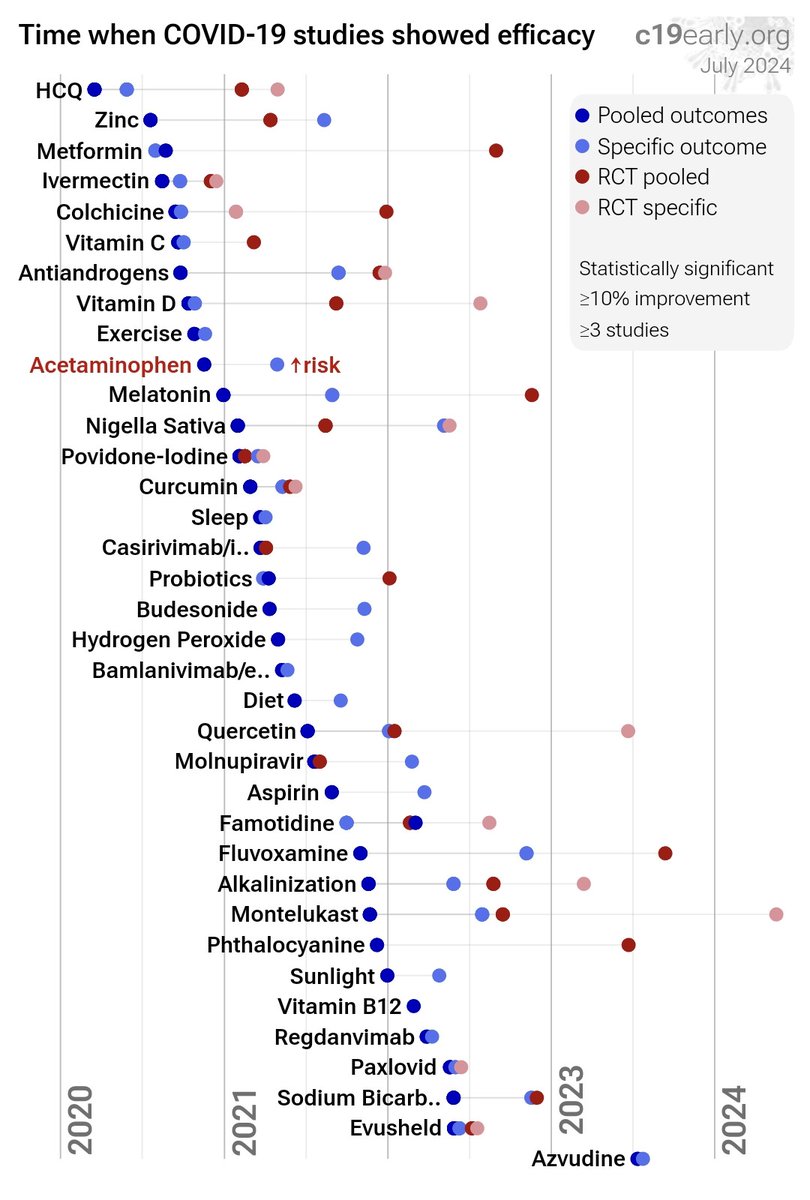
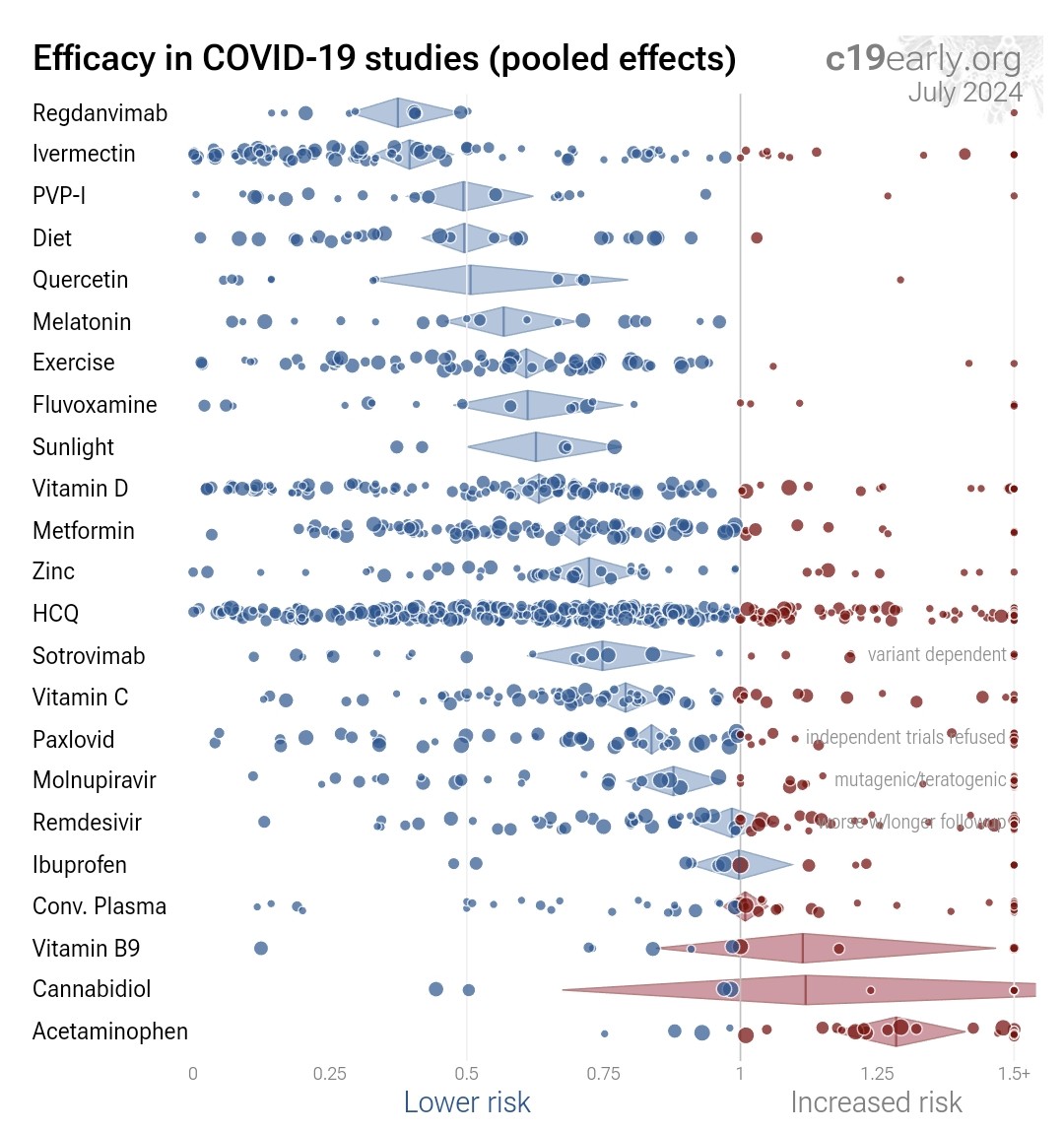
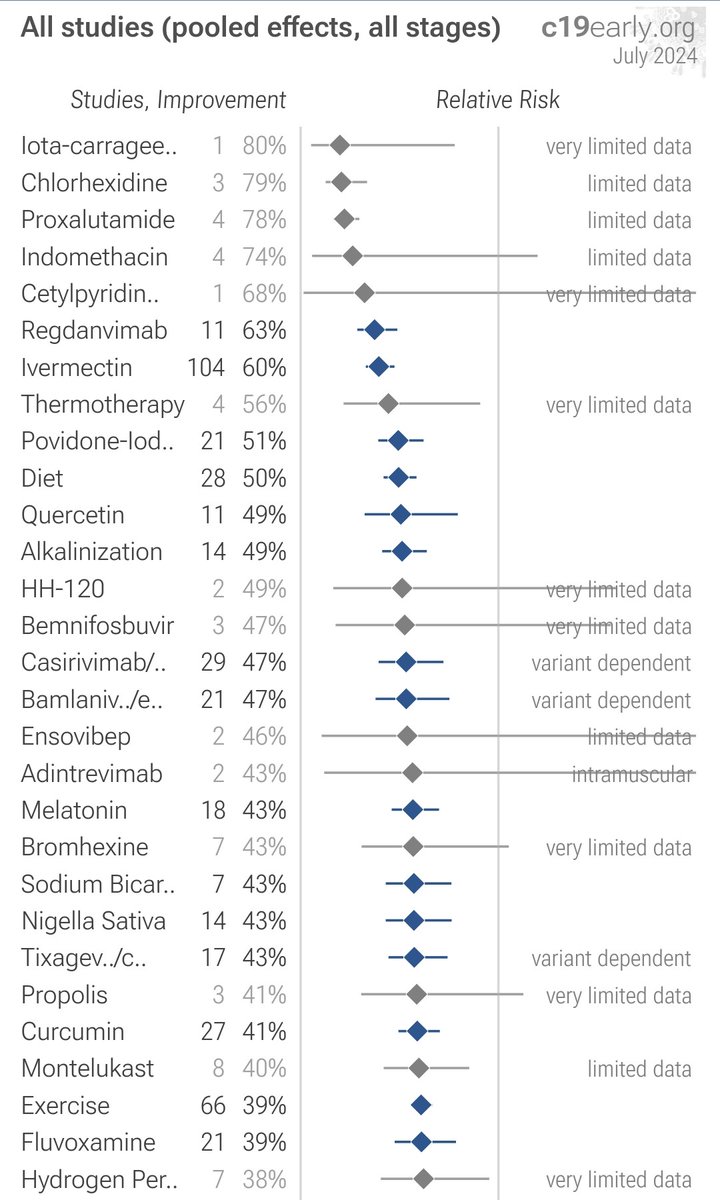
WHAT TREATMENTS WORK AGAINST COVID-19? 💯💥👍 Everything you want to know is here 👇 https://c19early.org/ WHO ARE THEY? They are a group of PhD researchers, scientists, and individuals dedicated to making a contribution, no matter how small.
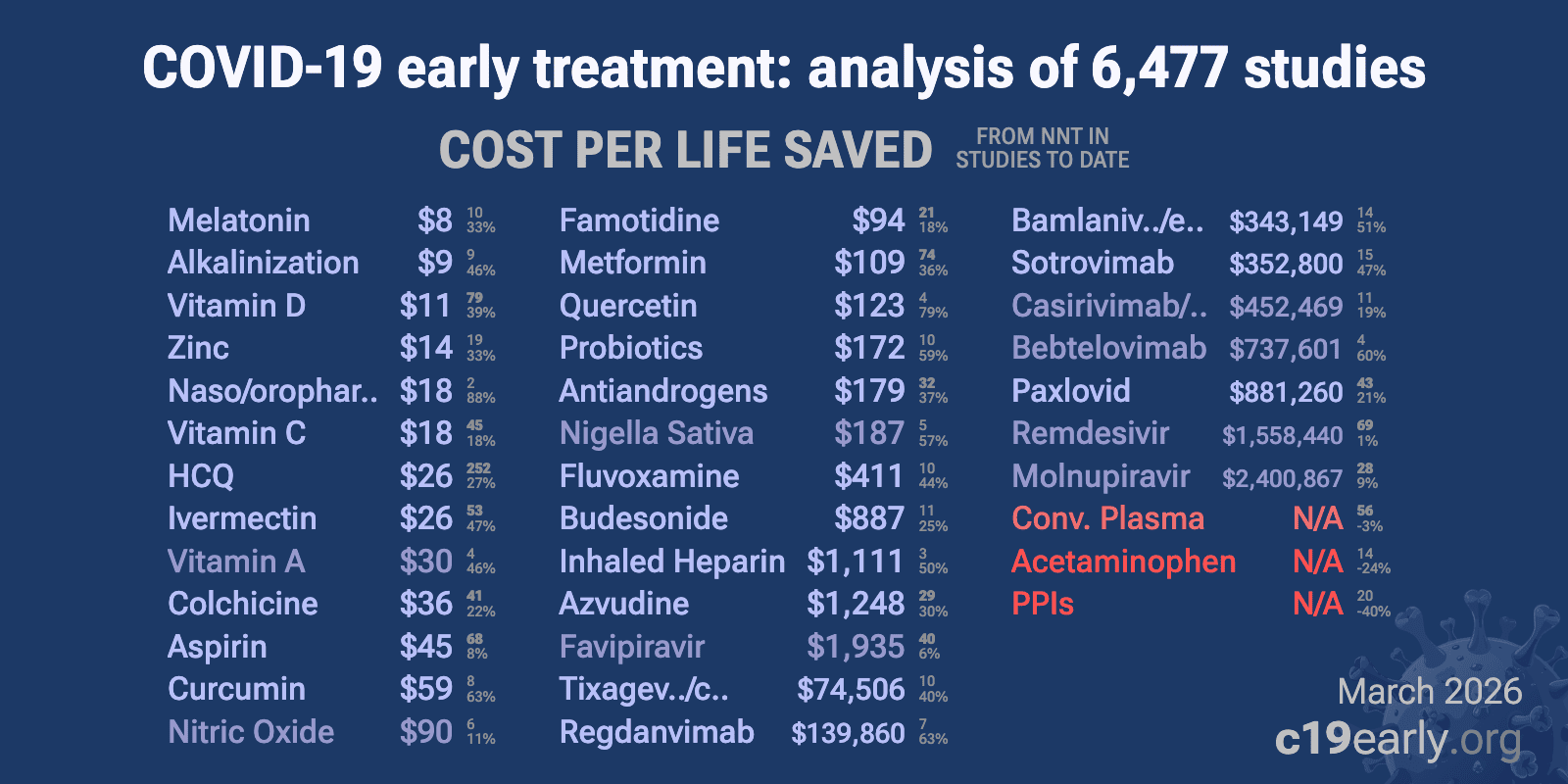
@ejustin46 - Emmanuel
2) Their research can be found in reputable journals like Science and Nature. WHAT TREATMENTS DO THEY RECOMMEND? They cannot provide medical advice but recommend to consult a qualified physician who can give personalized recommendations based on your medical history and ... https://t.co/NPSS3mXzA6
@ejustin46 - Emmanuel
3) ...current situation. This physician will be able to provide details on the risks and benefits of different treatments. WHY SHOULD WE TRUST THEM ? Trust is not required. This website provides organization and analysis of public and verifiable sources. https://t.co/vmHolamkOP
@ejustin46 - Emmanuel
4) For meta-analyses, all the necessary data to reproduce the analysis is included in the appendix, along with direct links to the original source papers. They are not financed by third parties and cover the running costs themselves. Thanks for reading 🙏 https://t.co/TyFmgMmpyM

@ejustin46 - Emmanuel
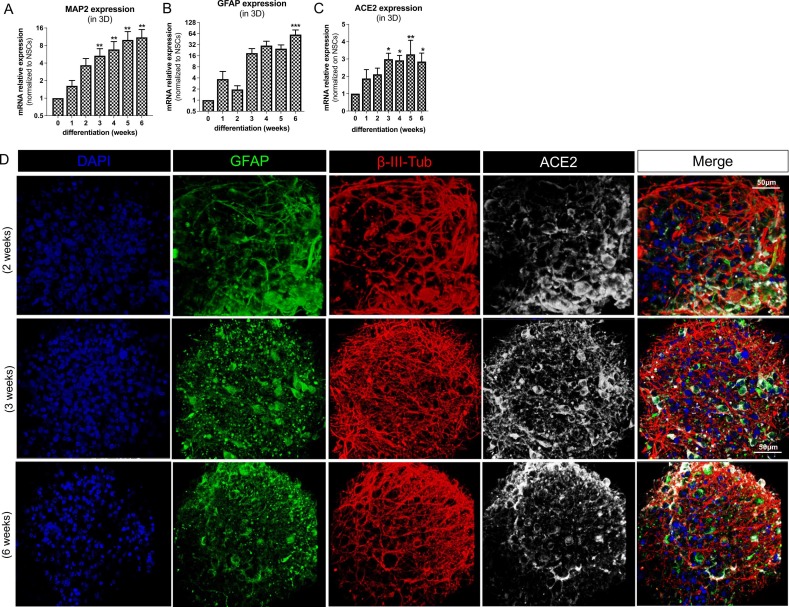
2) In this study, https://www.sciencedirect.com/science/article/pii/S0890623822000600 they investigated the potential neurotoxic effects of SARS-CoV-2 spike protein and toxin-like peptides found in COVID-19 patients on human 3D neuronal/glial models during brain development.

@ejustin46 - Emmanuel
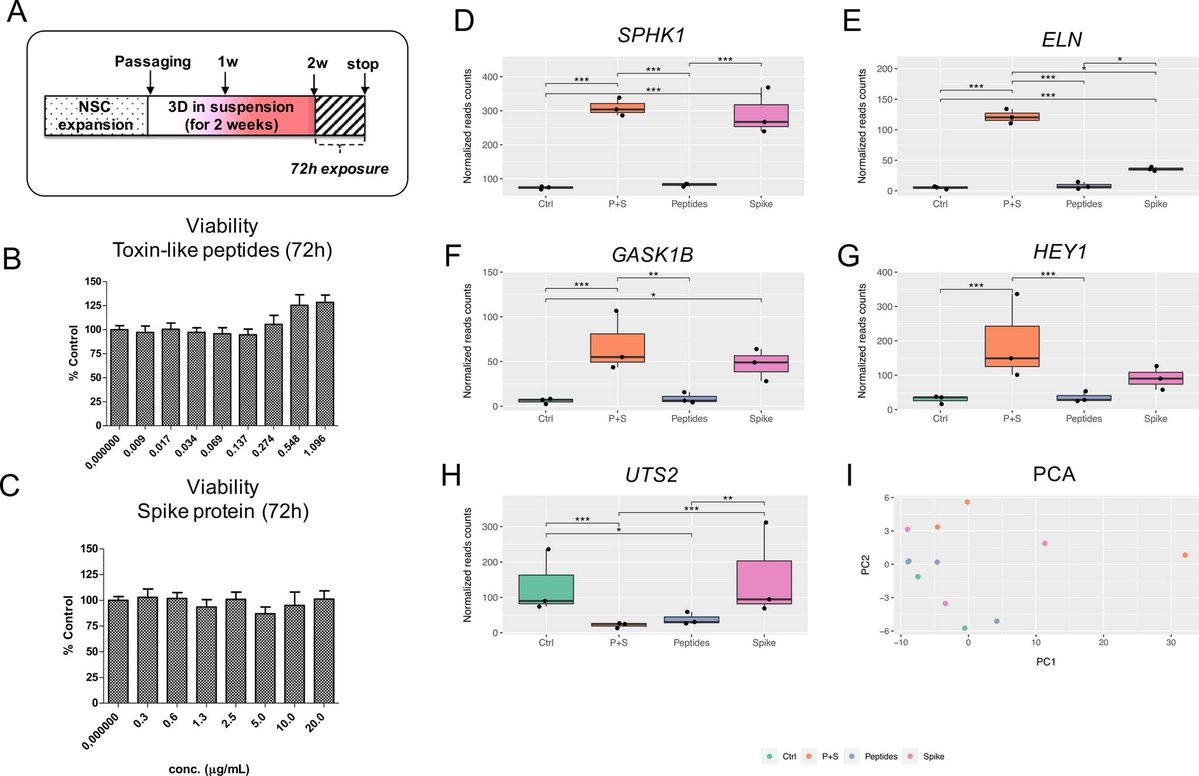
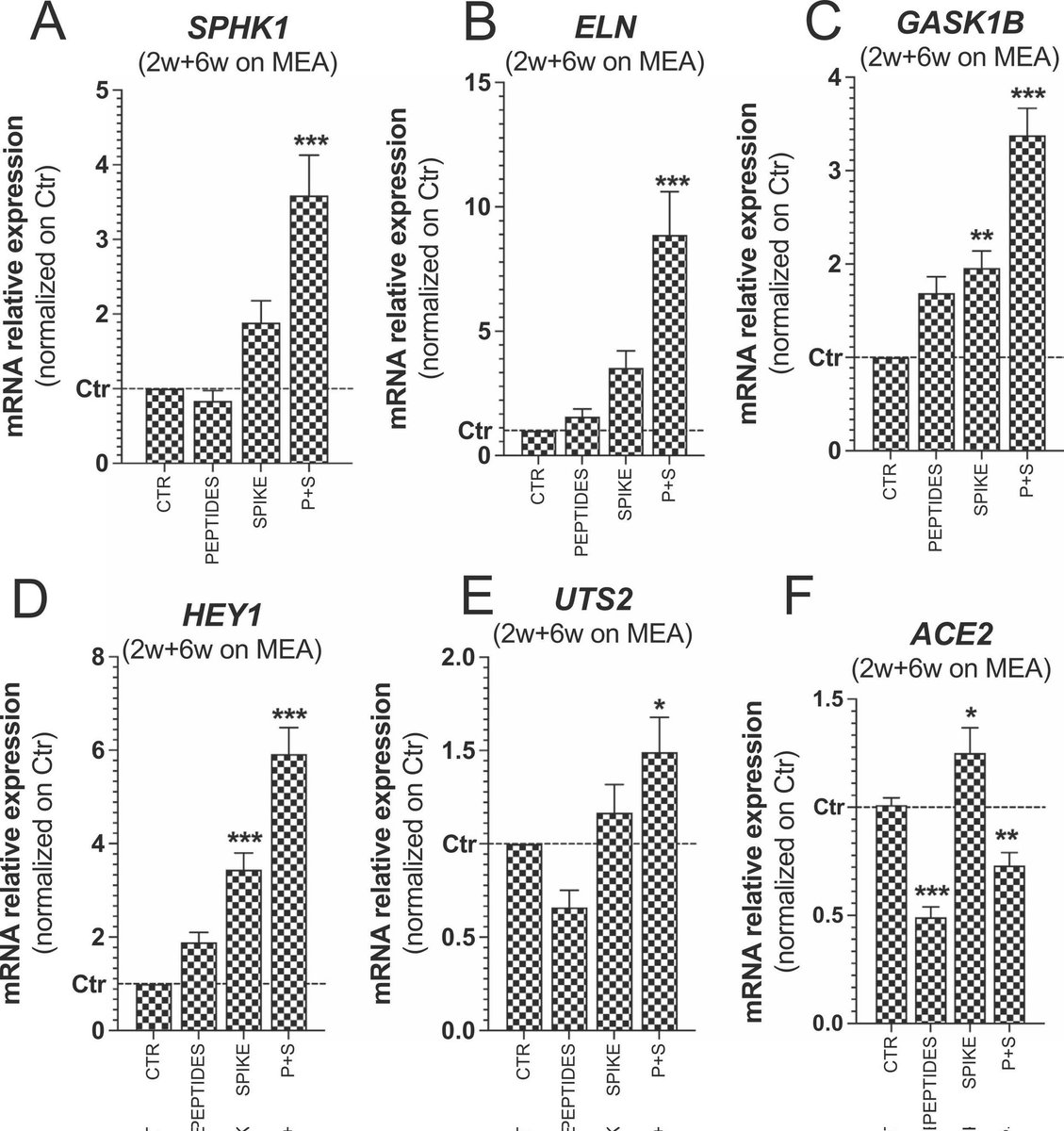
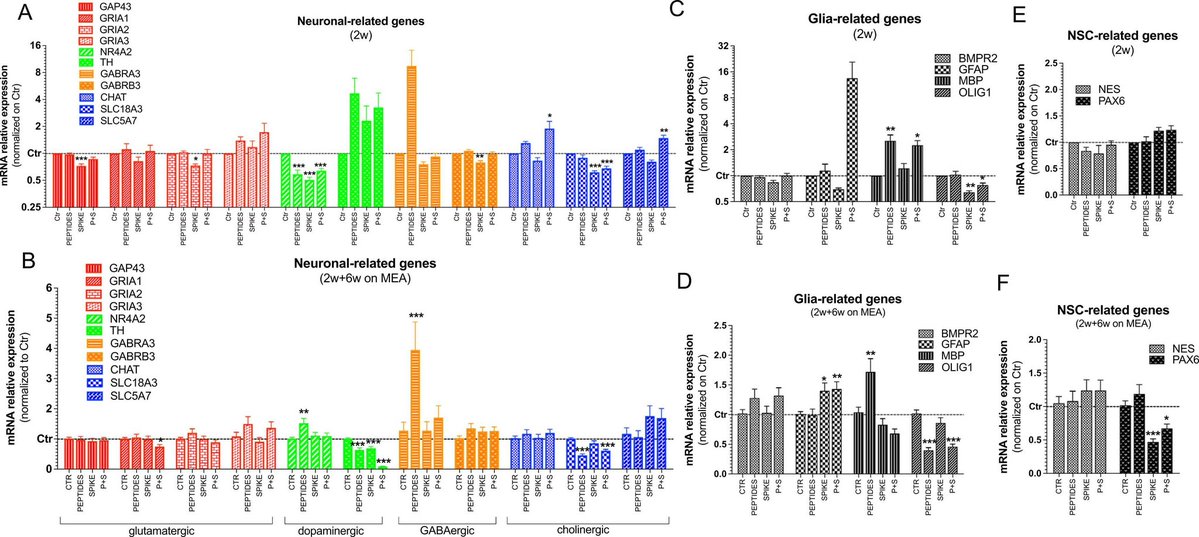
3) Using human iPSC-derived neural stem cells differentiated into 3D neurospheres, the authors found that spike protein and toxin-like peptides at non-cytotoxic concentrations differentially perturbed the expression of genes critical for brain development ... https://t.co/6X7R5YVhio
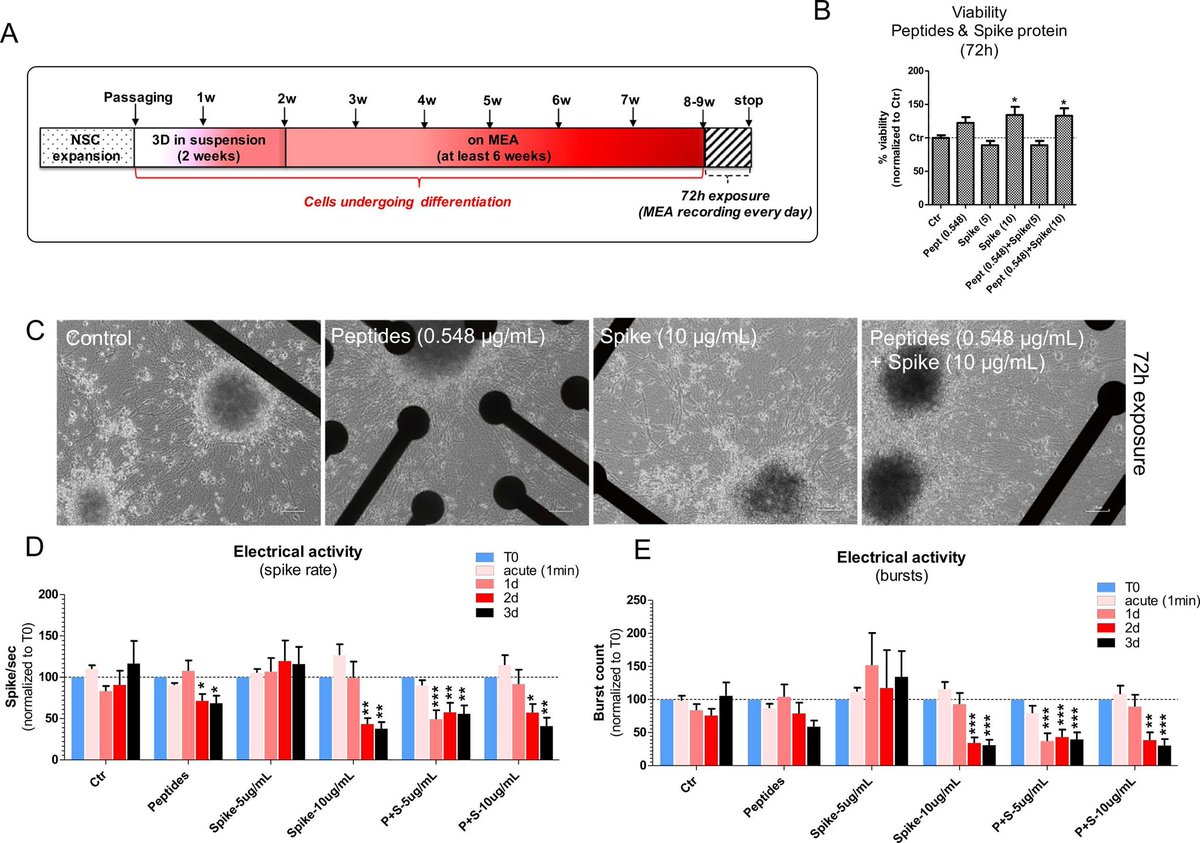
@ejustin46 - Emmanuel
4) ...including SPHK1, ELN, GASK1B, HEY1, UTS2, and ACE2. Exposure to spike protein caused a decrease in spontaneous electrical activity in long-term differentiated cultures, suggesting perturbation of neuronal network function. https://t.co/ekIEBl1fNM
@ejustin46 - Emmanuel
5) The observed transcriptional and functional effects are discussed in the context of key events described in adverse outcome pathways relevant to COVID-19-associated brain disorders, gathered in the CIAO project. https://t.co/xly7KYEvfq
@ejustin46 - Emmanuel
6) The results indicate that SARS-CoV-2 spike protein and potentially contaminating toxin-like peptides found in COVID-19 patients could disrupt neurodevelopmental processes, which may have implications for understanding ... https://t.co/4VSuuuRTen
@ejustin46 - Emmanuel
7) ...the impact of SARS-CoV-2 infection on brain development in children. In summary, the study provides mechanistic evidence on how SARS-CoV-2 components may adversely affect brain development using a human 3D neuronal/glial model system. Thanks for reading 🙏 https://t.co/PIHN7wW5oJ

@ejustin46 - Emmanuel
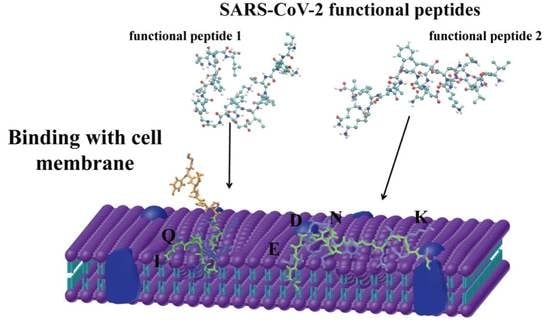
What if PEPTIDES were KEY ELEMENTS during SARS-COV-2 INFECTION? (1st part) Peptides are short chains of amino acids and they play a crucial role in the interaction between SARS-CoV-2, the virus that causes COVID-19, and the human body.
@ejustin46 - Emmanuel
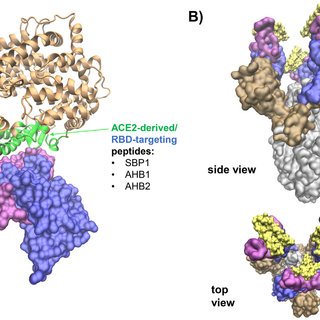
2) Peptides are involved in several key processes: - Viral Entry: SARS-CoV-2 enters human cells by binding to the ACE2 receptor on the surface of the host cells. Peptides derived from the ACE2 receptor can potentially block the interaction between the virus and the receptor,
@ejustin46 - Emmanuel
3) ...inhibiting viral entry. - Vaccine Development: Peptides derived from specific regions of the SARS-CoV-2 spike protein, such as the receptor-binding domain (RBD), are used in vaccine development. These peptides can stimulate the immune system and generate antibodies.
@ejustin46 - Emmanuel
4) Peptides have gained significant attention in recent studies due to their therapeutic potential. However, it is also important to acknowledge that peptides can have adverse effects and pose challenges.
@ejustin46 - Emmanuel
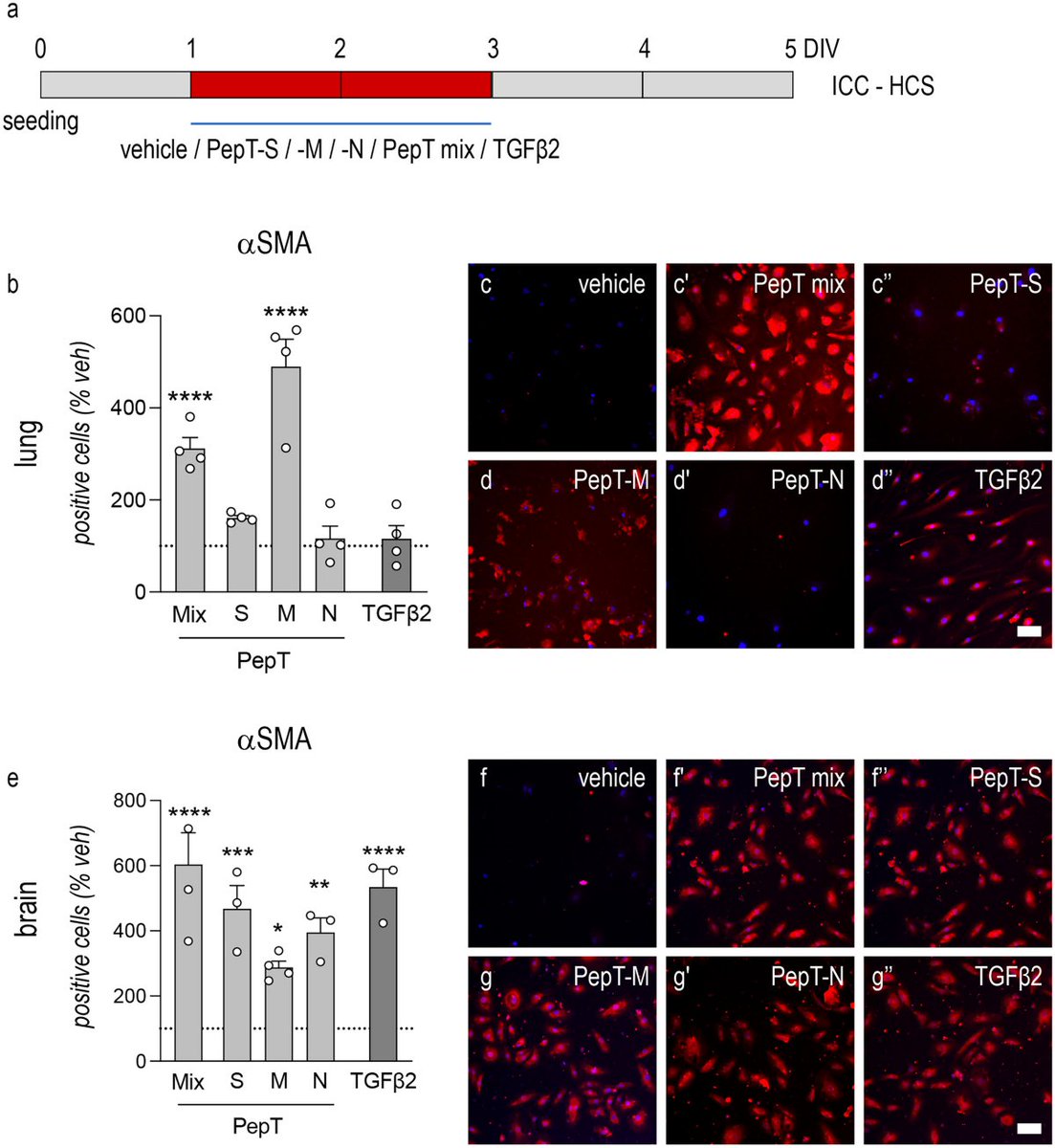
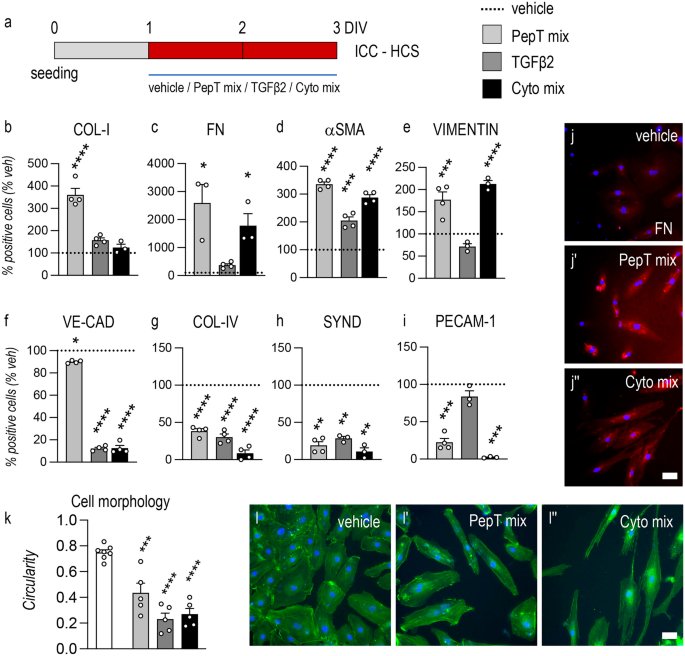
5) PEPTIDES and LONG COVID In this first recent study, they showed that SARS-CoV-2 peptides were found to induce irreversible endothelial-to-mesenchymal transition (EndMT) in endothelial cells from various organs, with the M peptide being particularly significant in lung cells.
@ejustin46 - Emmanuel
6) These findings support the idea that SARS-CoV-2-induced microvascular damage contributes to organ dysfunction and long-COVID syndrome. https://link.springer.com/article/10.1007/s00441-024-03900-y

@ejustin46 - Emmanuel
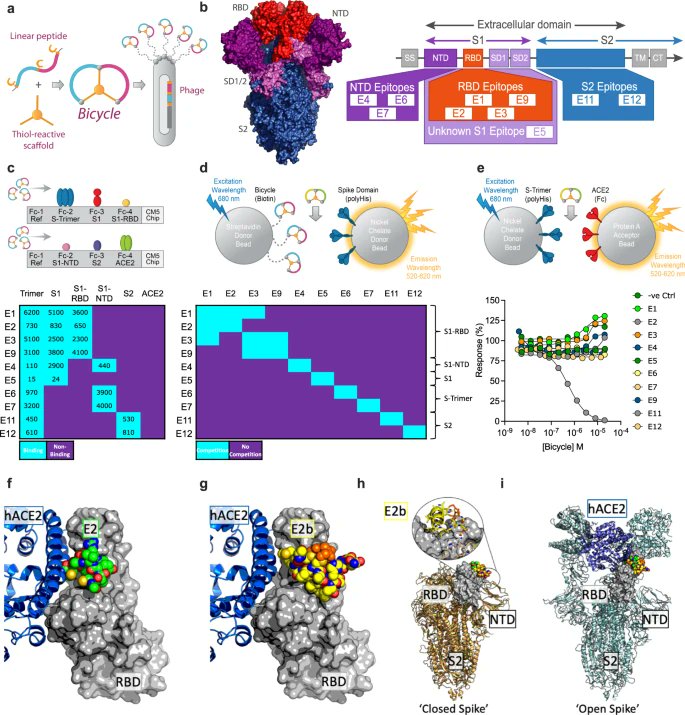
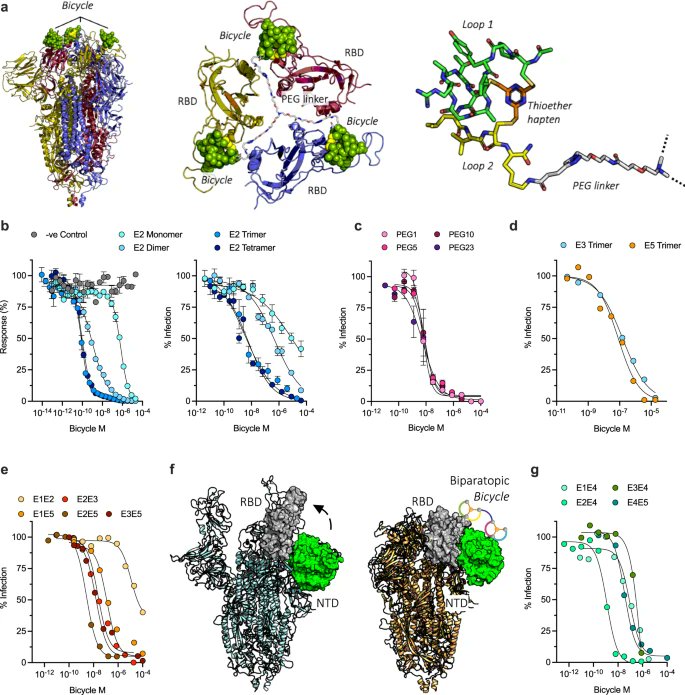
7) PEPTIDES as ANTIVIRALS against SARS-COV-2 In this 2nd study, they showed that bicyclic peptides are a novel antiviral modality that can rapidly generate potent SARS-CoV-2 inhibitors. Screening phage libraries identified binders across the Spike protein, which were easily ...
@ejustin46 - Emmanuel
8) ...multimerized or combined into biparatopic formats to enhance affinity and access new inhibitory mechanisms. Bicycles potently inhibited infection and viral replication in vitro and in animal models, including against variants of concern, while also reducing inflammation.
@ejustin46 - Emmanuel
9) Reference: https://www.nature.com/articles/s41467-023-39158-1 In a 2nd part of our presentation, we will delve deeper into the measurement of ambiguity and complexity in peptides. While these peptides can be beneficial in fighting SARS-COV-2, they can also have detrimental effects on our body.
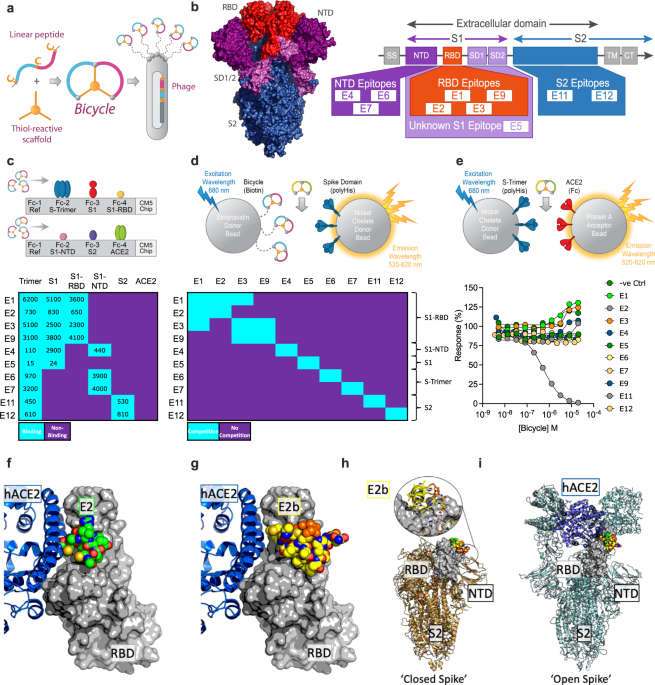
@ejustin46 - Emmanuel
10) See you soon to explore this captivating subject further. Thanks for reading 🙏 https://t.co/o58rj59str

@ejustin46 - Emmanuel
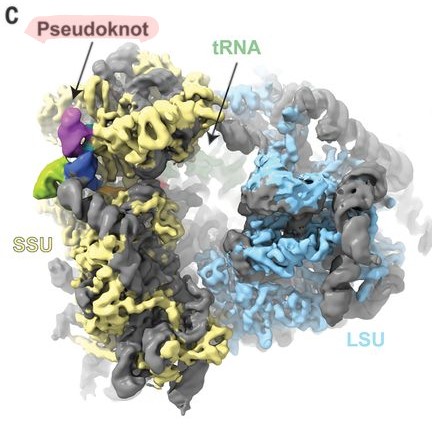
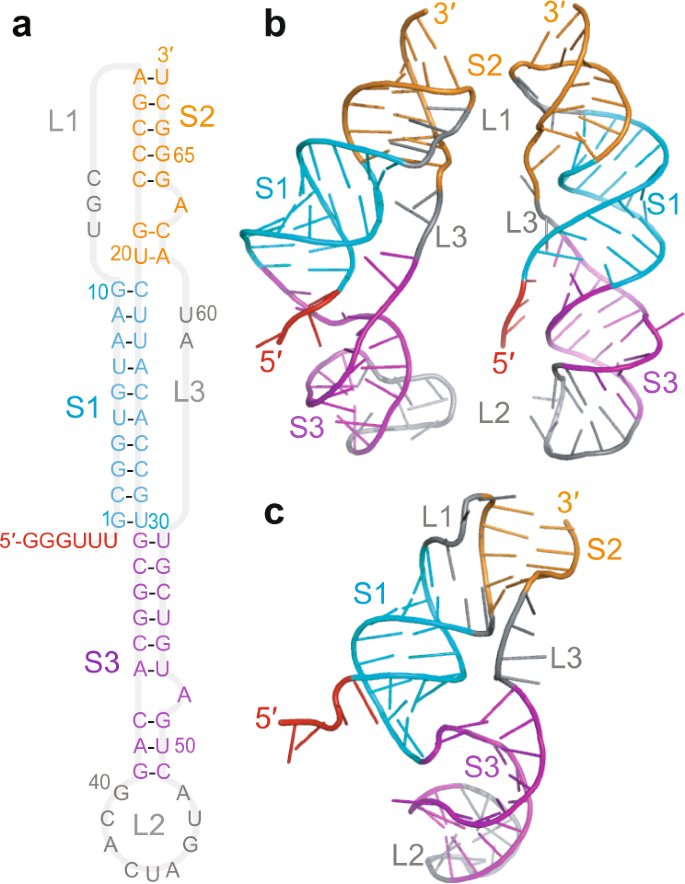
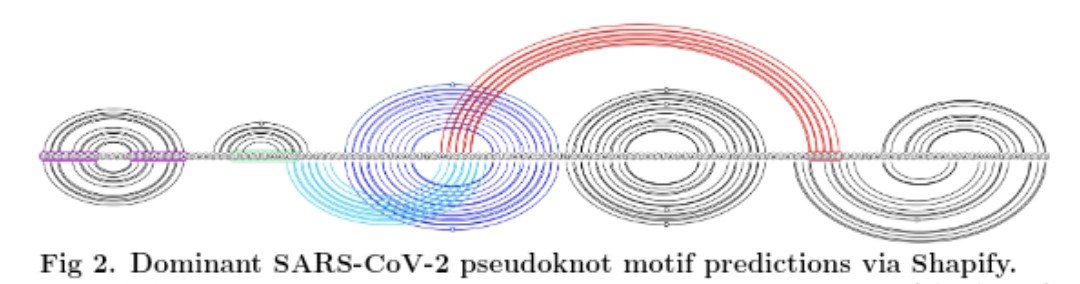
TYING THE KNOT Unraveling the Intricacies of the Coronavirus Frameshift Pseudoknot https://www.biorxiv.org/content/10.1101/2023.12.28.573501v1

@ejustin46 - Emmanuel
2) I take the opportunity of this complex study (not layman at all) to express my admiration for the scientists 🙏, who continue to try to unravel the secrets of SARS-COV-2, four years after the start of the pandemic, while so many people, started with politicians have given up.
@ejustin46 - Emmanuel
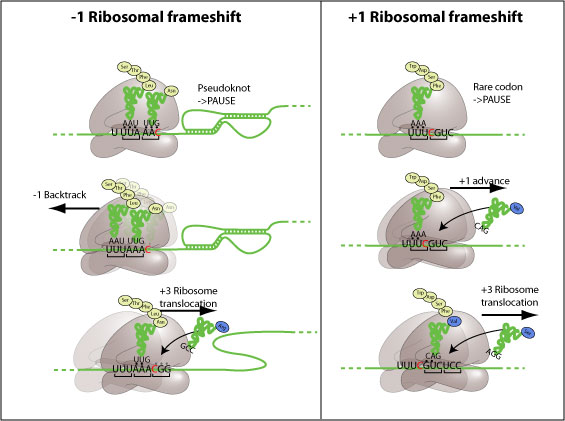
3) For enthusiasts😊 RIBOSOMAL FRAMESHITING is a phenomenon that occurs during translation, where the ribosome shifts to a different reading frame and continues to synthesize proteins and can result in the production of multiple proteins. A good article👇 https://www.news-medical.net/news/20201028/Structure-and-mechanisms-of-ribosomal-frameshifting-during-SARS-CoV-2-translation.aspx
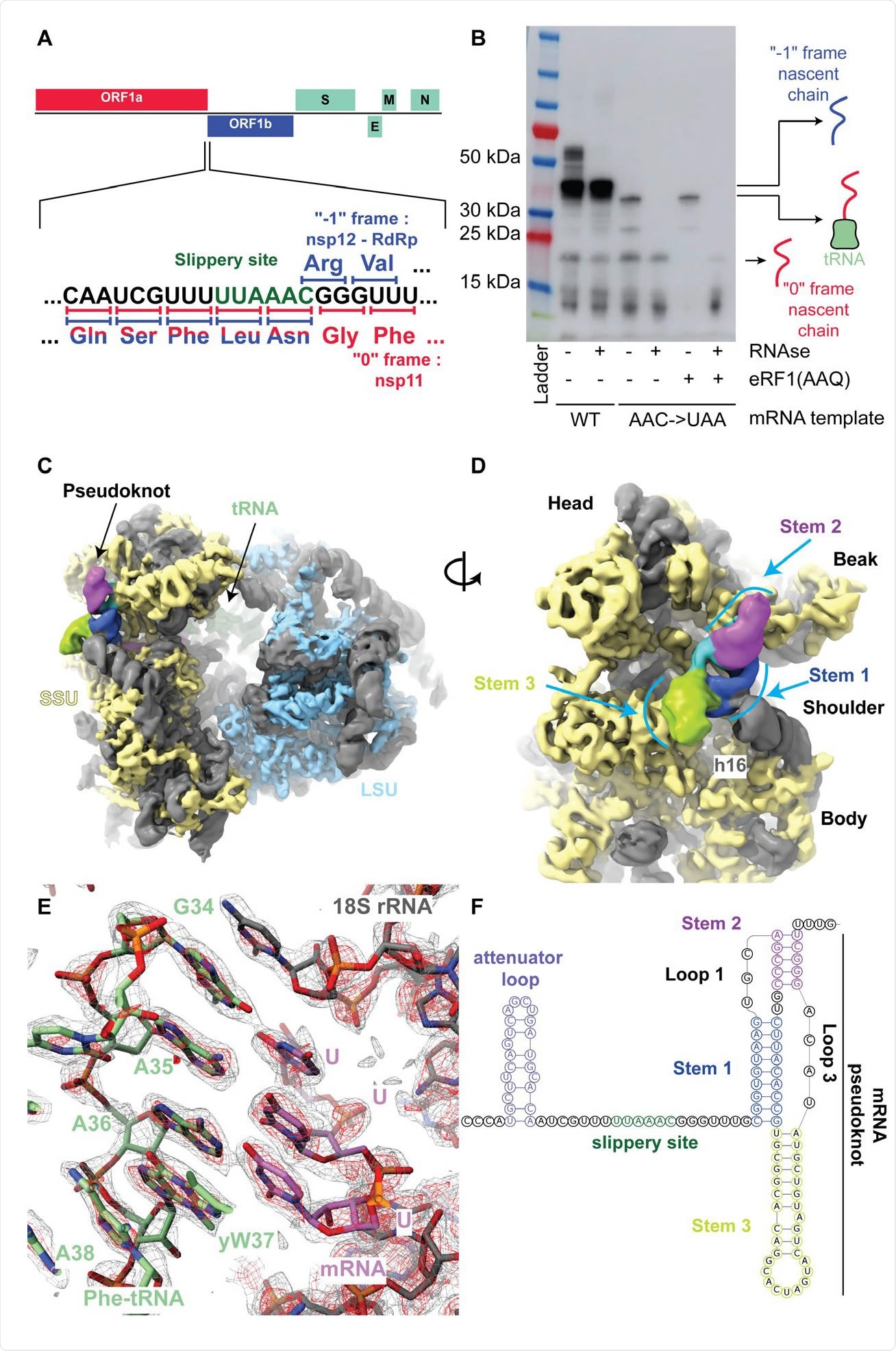
@ejustin46 - Emmanuel
4) PSEUDOKNOT is a complex RNA structure formed by base pairing between distant regions of the RNA molecule. In the case of SARS-CoV-2, the pseudoknot is located in the viral RNA genome, in the region where the viral replicase gene overlaps with the structural protein genes.
@ejustin46 - Emmanuel
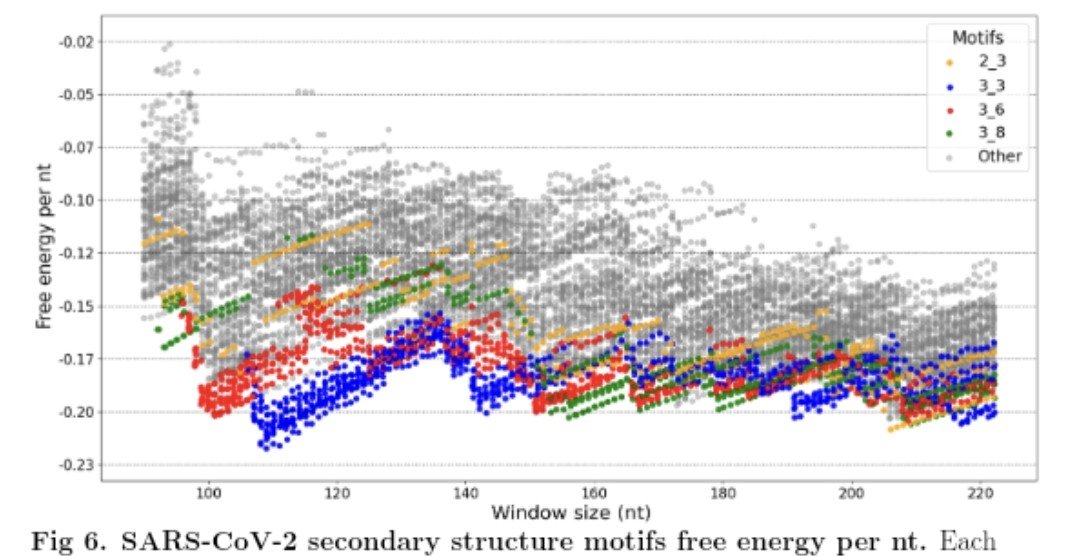
5) In the study, "Leveraging the fact that all coronaviruses use -1 programmed ribosomal frameshifting (-1 PRF) to replicate, we apply algorithms to predict the most energetically favourable secondary structures (each nucleotide involved in at most one pairing)
@ejustin46 - Emmanuel
6) ... that may be involved in regulating the -1 PRF event in coronaviruses, especially SARS-CoV-2." Thanks for reading 🙏 Other reference : https://www.nature.com/articles/s41467-021-25085-6 https://www.science.org/doi/10.1126/science.abf3546 FYI@LongDesertTrain@DavidJoffe64
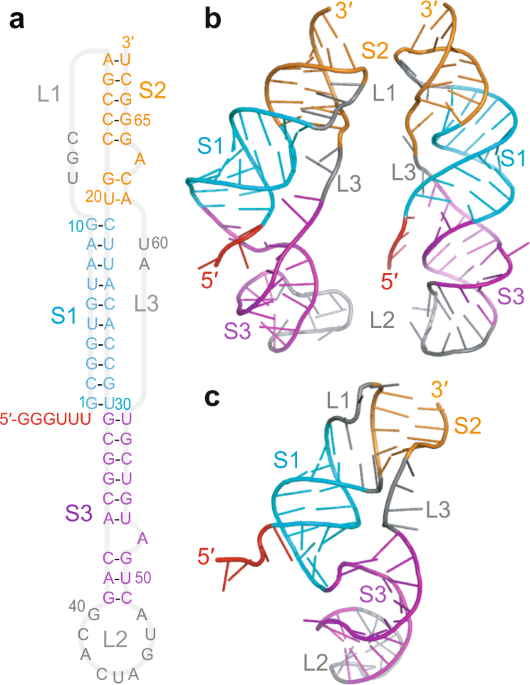

@ejustin46 - Emmanuel
𝙇𝙊𝙉𝙂 𝘾𝙊𝙑𝙄𝘿, 𝙑𝙄𝙍𝘼𝙇 𝙋𝙀𝙍𝙎𝙄𝙎𝙏𝙀𝙉𝘾𝙀 𝙖𝙣𝙙 𝘾𝙇𝙀𝘼𝙍𝘼𝙉𝘾𝙀 ? (3𝘳𝘥 𝘱𝘢𝘳𝘵) Before discussing the clearance of the virus from our organs, it is important to acknowledge the persistence of the virus in immunocompromised individuals.
@ejustin46 - Emmanuel
2) Not only does the virus remain in our organs and induce a persistent inflammatory state, but it also utilizes this opportunity to mutate and further spread among the global population.
@ejustin46 - Emmanuel
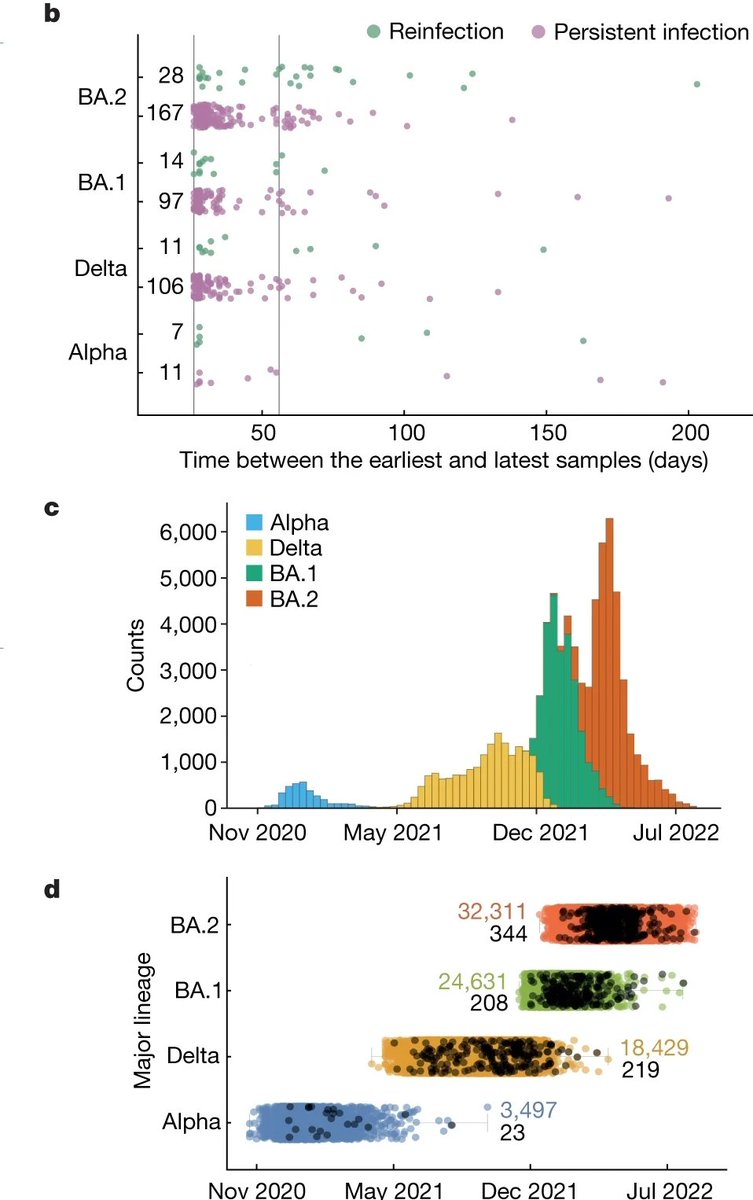
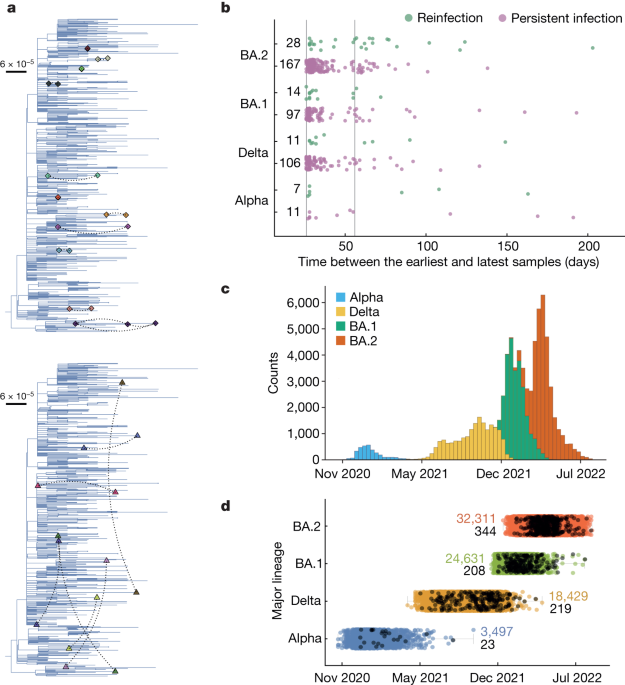
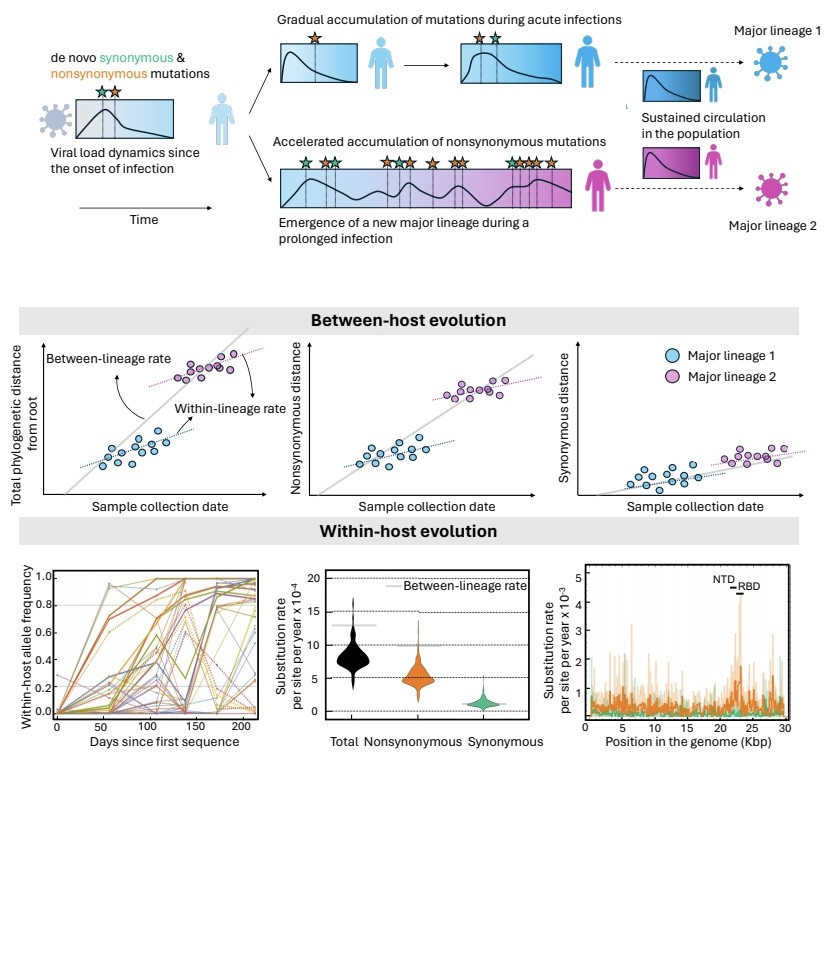
3) In this area, the studies of @Mahan_Ghafari and his colleagues are exceptional and we recommend them.
@ejustin46 - Emmanuel
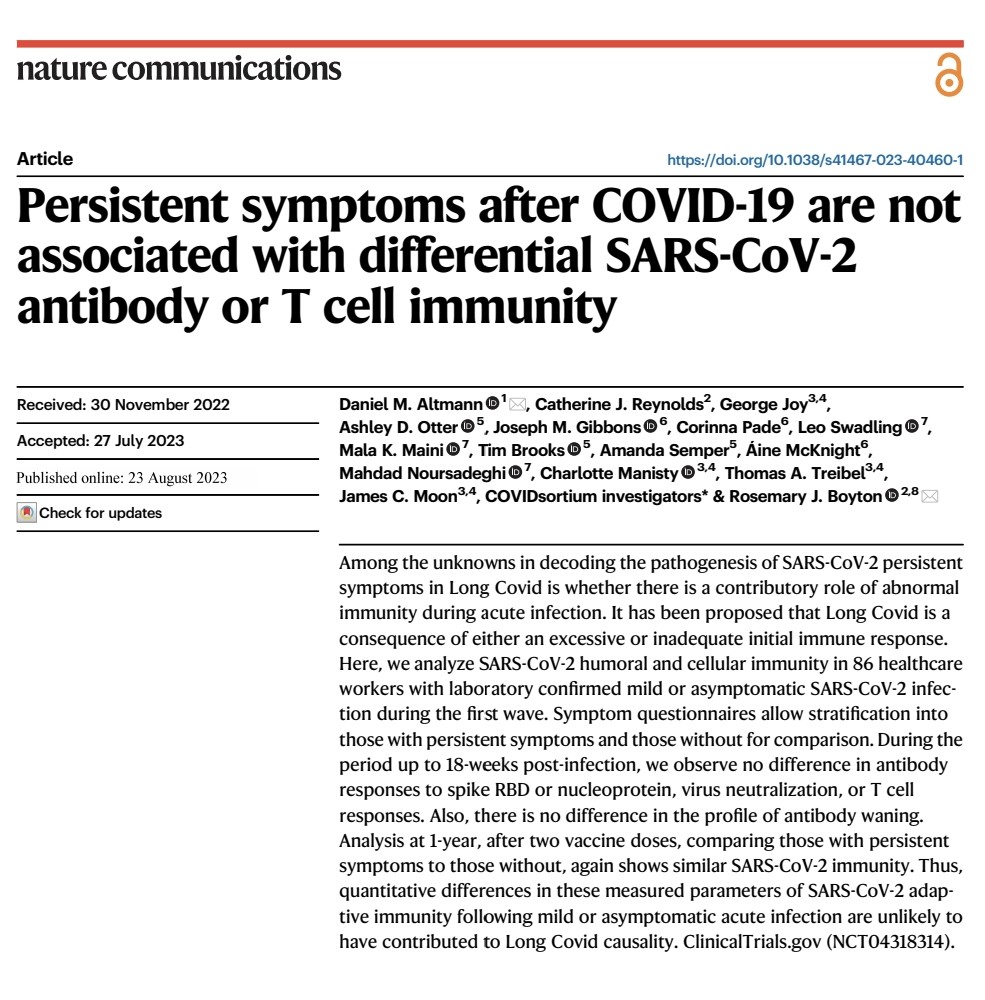
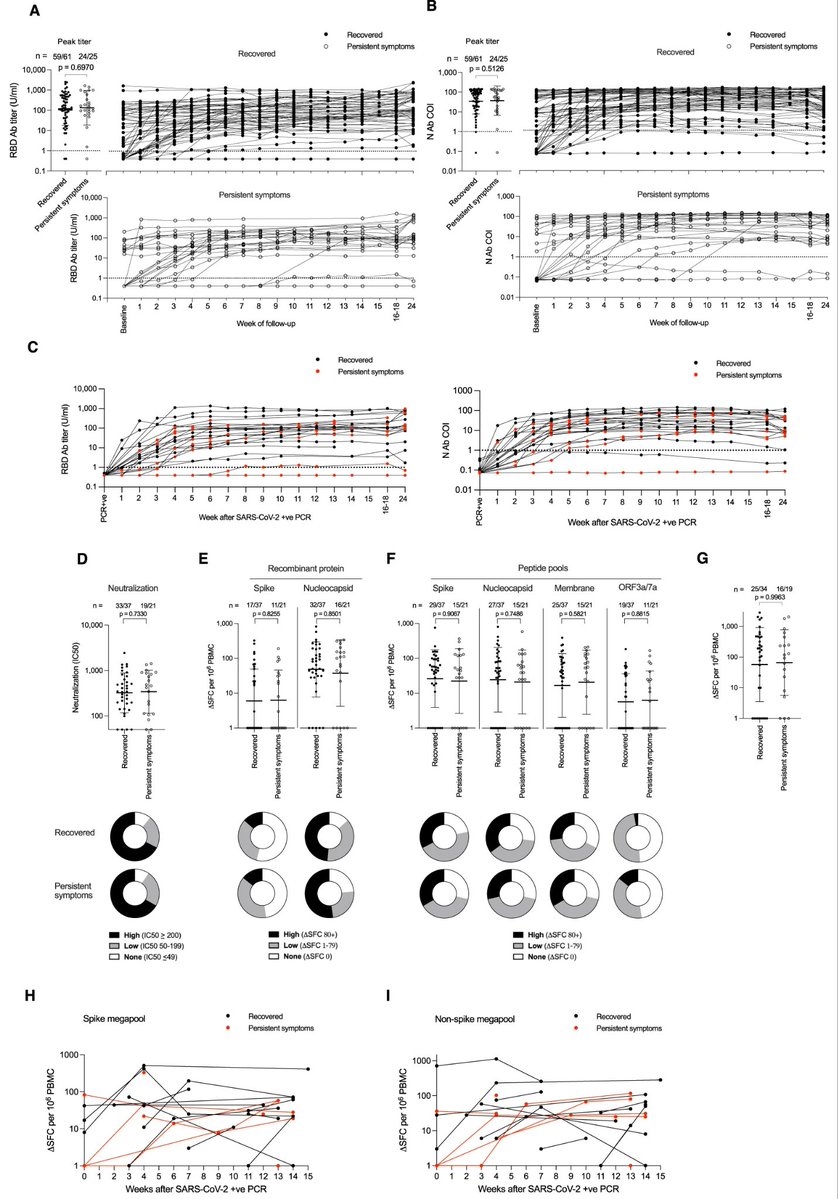
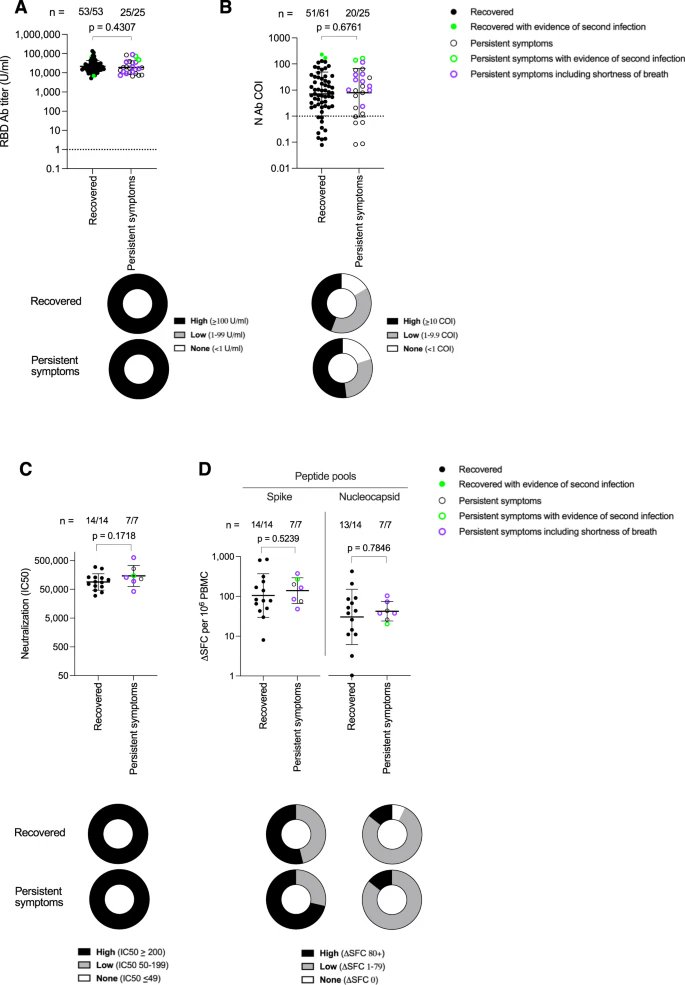
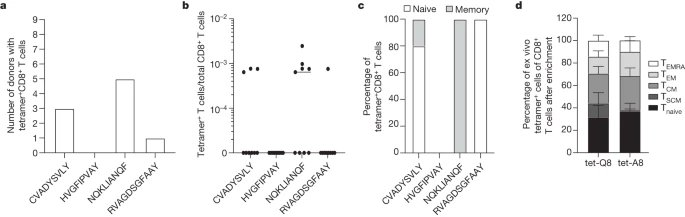
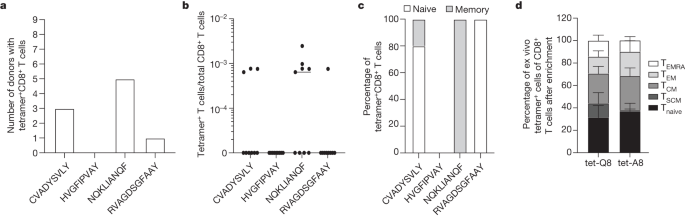
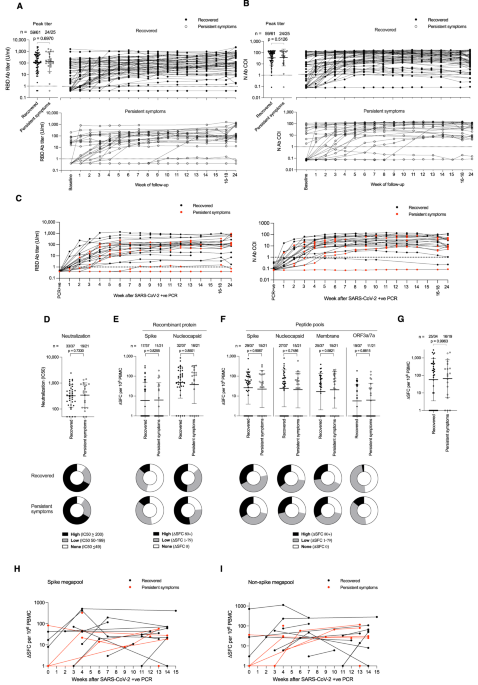
4) From @Daltmann10 and colleagues "Persistent symptoms after COVID-19 are not associated with differential SARS-CoV-2 antibody or T cell immunity" https://www.nature.com/articles/s41467-023-40460-1 This is a mysterious study, as the researchers did not find any differences in the immune system's response
@ejustin46 - Emmanuel
5) ...to the initial COVID-19 infection between those who went on to develop persistent Long COVID symptoms and those who fully recovered. Specifically: 1. Antibody levels - The researchers found no differences in peak antibody levels against the spike and nucleocapsid proteins
@ejustin46 - Emmanuel
6) ...nor in the pattern of antibody waning over time, between the two groups. 2. Neutralizing antibodies - There was also no difference in the levels of neutralizing antibodies, which are important for blocking the virus. 3. T cell responses - The researchers examined ...
@ejustin46 - Emmanuel
7) ... T cell responses to different SARS-CoV-2 proteins and found no differences between the groups. The lack of differences in these key immune parameters suggests that the immune system appears to be responding similarly in both the persistent symptom group and ...
@ejustin46 - Emmanuel
8) ... the fully recovered group. This implies that differences in immune function are unlikely to be the primary driver of why the virus seems to persist and cause long-term effects in some individuals, while others fully recover.
@ejustin46 - Emmanuel
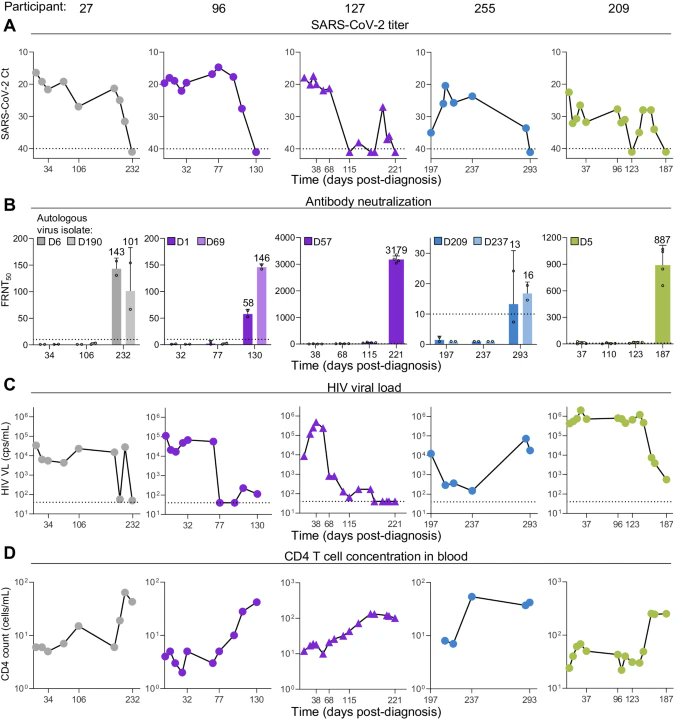
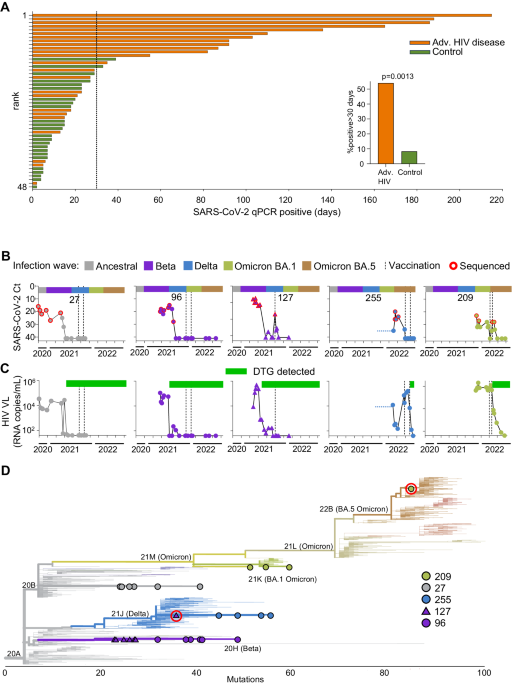
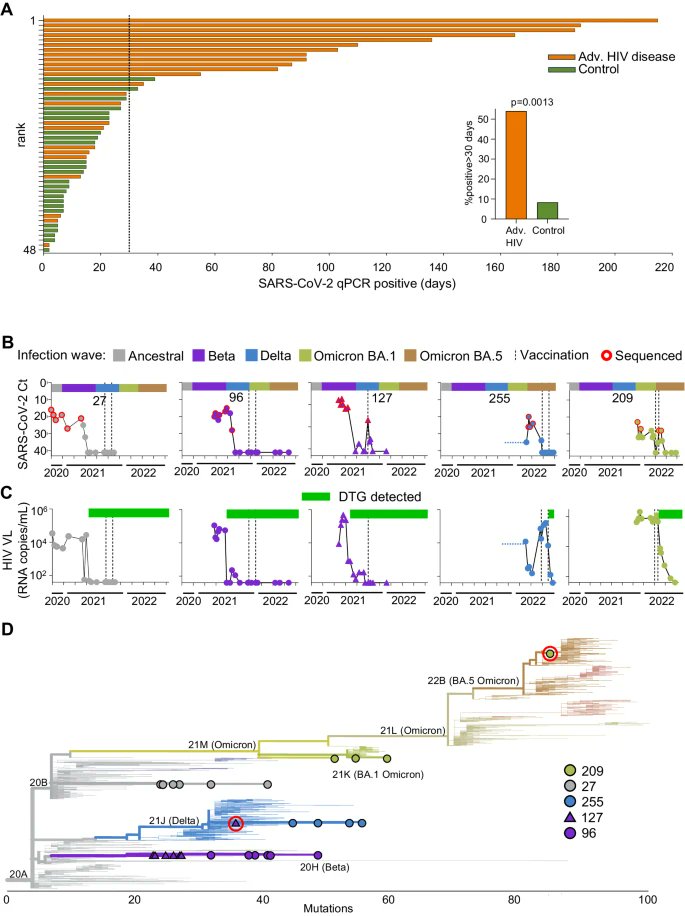
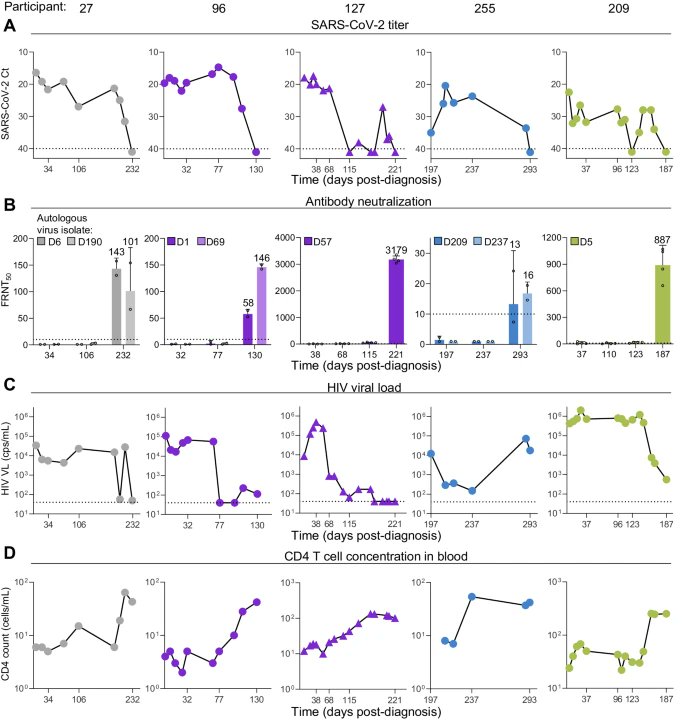
9) This study which looked at people with advanced HIV disease, where the immune system is severely weakened, provides some answers for the clearance. It found that these people often had very long-lasting SARS-CoV-2 infections, lasting over a month in ..
@ejustin46 - Emmanuel
10) ...54% of cases. The study showed that in these advanced HIV patients, the SARS-CoV-2 virus was cleared when they developed neutralizing antibodies - antibodies that can block the virus from infecting cells. https://t.co/MH5gvm8trH
@ejustin46 - Emmanuel
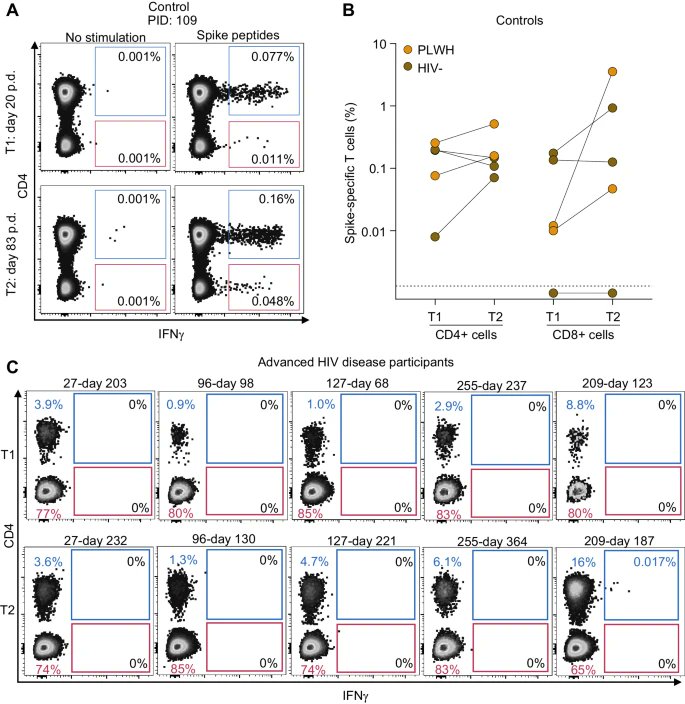
11) Importantly, this happened even if the patients' HIV was not fully suppressed by treatment. It is interesting to note that while the clearance of SARS-CoV-2 was linked to the development of neutralizing antibodies, it was not necessarily associated with ... https://t.co/HNXU2TDU5F
@ejustin46 - Emmanuel
12) ...the SARS-CoV-2-specific CD8 T cells, which are considered to be the main players in this process. Additionally, complete HIV suppression was not found to be a requirement for clearance. https://t.co/mpP6DNQu3b
@ejustin46 - Emmanuel
13) In the area of understanding persistence and clearance mechanisms, there is still much to learn. I realize that I have embarked on a "gargantuan" work on this topic to use the words of @1goodtern If you want, you can send me free espresso emoji ☕️ to keep me going 😂😂😂

@ejustin46 - Emmanuel
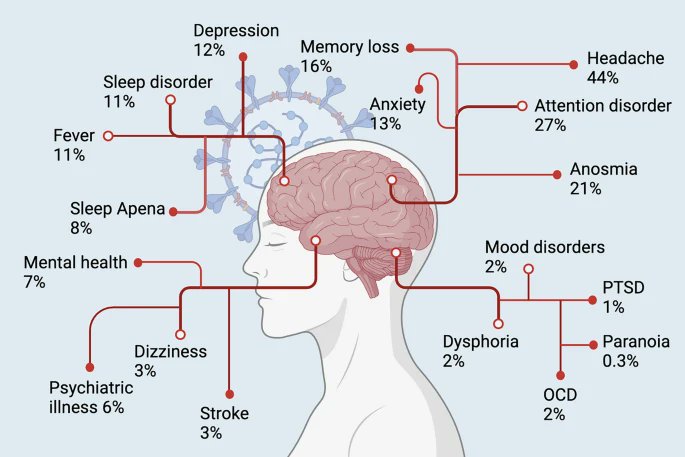
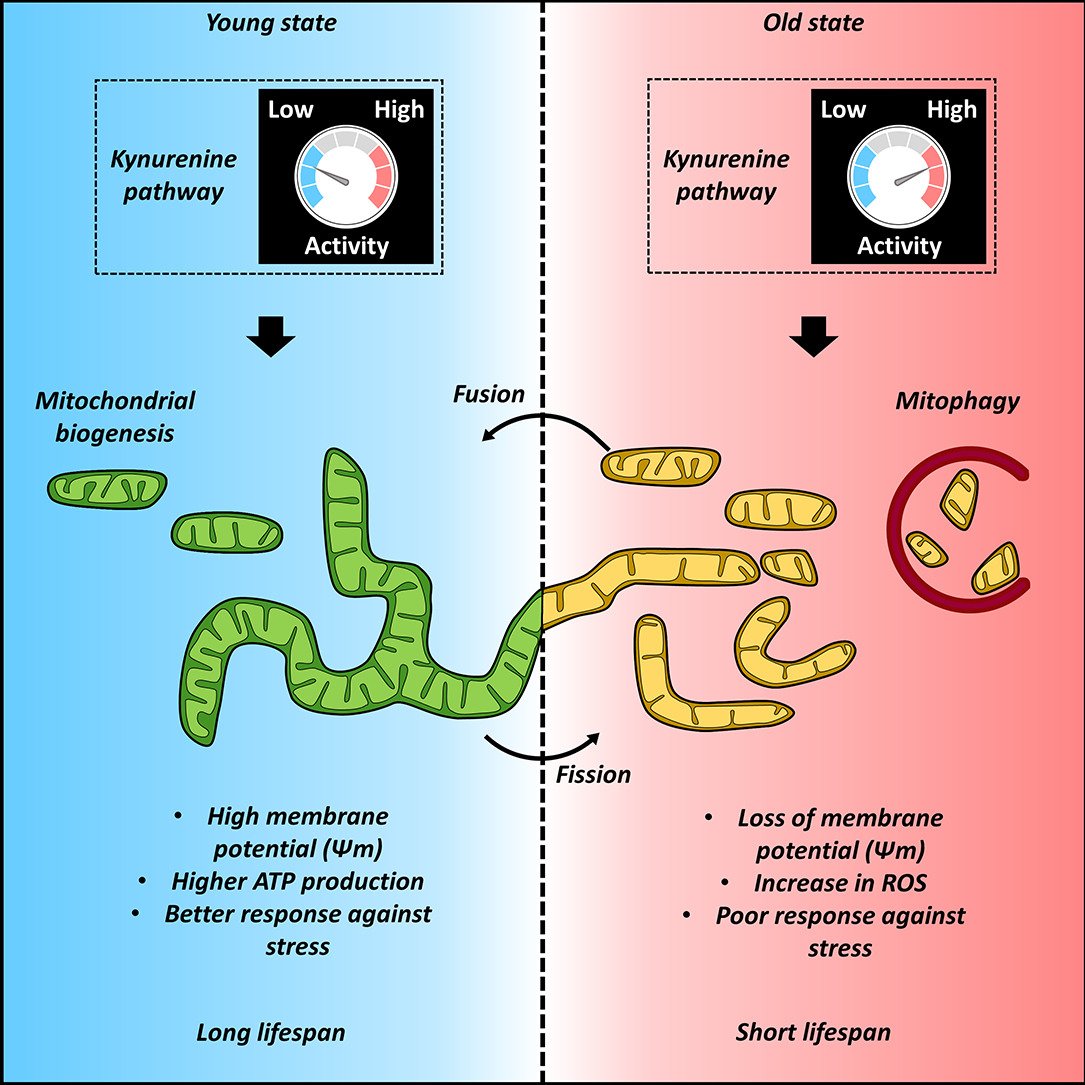
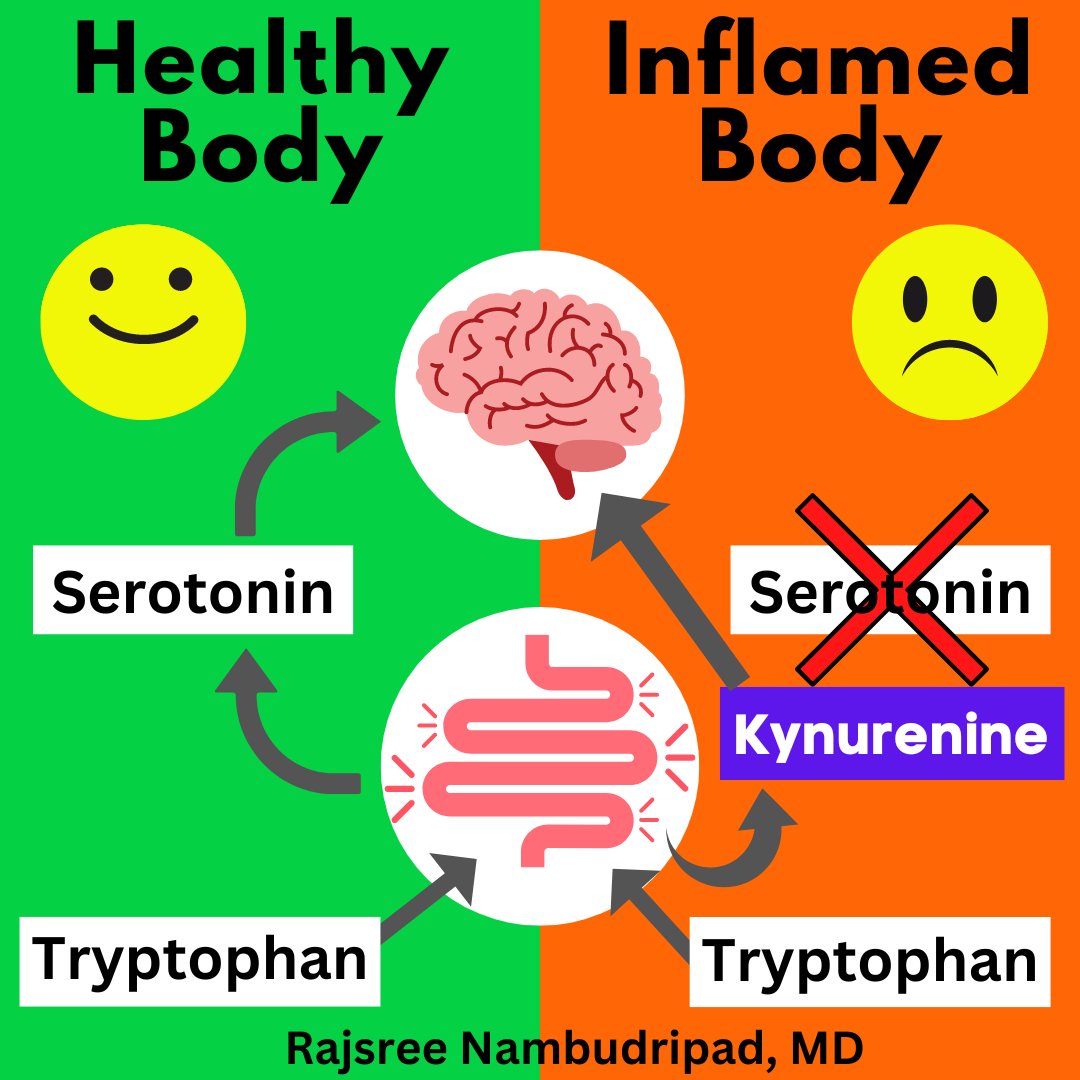
𝙒𝙝𝙮 𝙨𝙤 𝙢𝙖𝙣𝙮 𝙉𝙀𝙐𝙍𝙊𝙋𝙎𝙔𝘾𝙃𝙄𝘼𝙏𝙍𝙄𝘾 𝙎𝙔𝙈𝙋𝙏𝙊𝙈𝙎 𝙖𝙨𝙨𝙤𝙘𝙞𝙖𝙩𝙚𝙙 𝙬𝙞𝙩𝙝 𝙡𝙤𝙣𝙜-𝘾𝙊𝙑𝙄𝘿-19 ? 𝘼𝙣 𝙚𝙭𝙥𝙡𝙖𝙣𝙖𝙩𝙞𝙤𝙣: 𝙩𝙝𝙚 𝙆𝙔𝙉𝙐𝙍𝙀𝙉𝙄𝙉𝙀 𝙋𝘼𝙏𝙃𝙒𝘼𝙔 https://ncbi.nlm.nih.gov/research/coronavirus/publication/38802702
@ejustin46 - Emmanuel
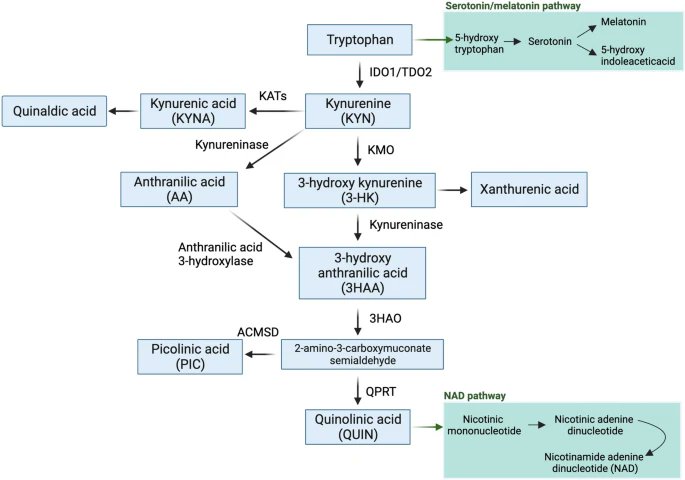
2) The kynurenine pathway metabolizes the essential amino acid tryptophan into neuroactive compounds like kynurenine, kynurenic acid, and quinolinic acid. It is activated by inflammation and produces both neuroprotective and neurotoxic metabolites. https://t.co/XKg6vWpDfZ
@ejustin46 - Emmanuel
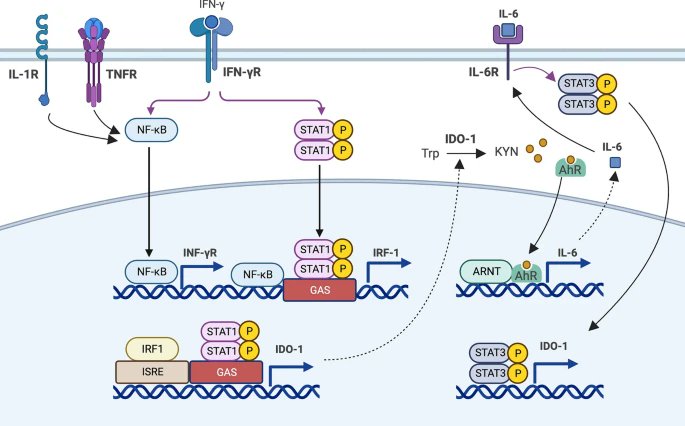
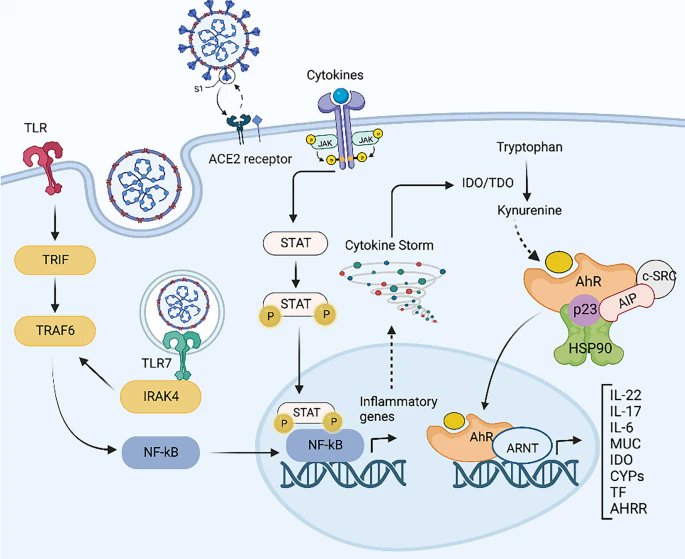
3) The SARS-CoV-2 virus that causes COVID-19 can significantly alter levels of metabolites in the kynurenine pathway (KP), which metabolizes the essential amino acid tryptophan. During acute infection, inflammation raises levels of cytokines like IFN-γ ...
@ejustin46 - Emmanuel
4) ...that induce the KP enzyme IDO-1. This shifts tryptophan metabolism toward neurotoxic KP metabolites like QUIN and 3-HK rather than serotonin. Elevated KP metabolites have been found in COVID-19 patients, correlating with illness severity and prognosis. https://t.co/6kWn5M8y2f
@ejustin46 - Emmanuel
5) Prolonged KP activation may explain long-term issues after COVID-19. Studies found cognitive impairment in post-acute patients linked to high QUIN and 3-HAA over months. Chronic headaches, fatigue and mood changes in long COVID may also involve KP/NMDA receptor interactions https://t.co/w5Sv3oFwjk
@ejustin46 - Emmanuel
6) ...and reduced NAD+ from excessive QUIN. Lingering virus fragments could sustain inflammation driving KP dysregulation. Modulating the KP may help manage COVID-19's impact. Targeting IDO-1 or inhibiting neurotoxic metabolite production reduce inflammation and neurotoxicity. https://t.co/w12HJLCIPr
@ejustin46 - Emmanuel
7) Correcting imbalances like restoring NAD+ may address persistent symptoms. Further KP research could yield biomarkers to predict outcomes and guide care. Longitudinal studies are needed to clarify the virus's lasting effects through metabolic pathways like the KP.
@ejustin46 - Emmanuel
8) It is a key topic and to end, a simple graph to understand this challenge of the kynurenine pathway. Thanks for reading 🙏 https://t.co/SAGboyvrCn

@ejustin46 - Emmanuel
8) Thanks for reading 🙏 FYI @MeetJess @LauraMiers @DavidJoffe64 @RadCentrism @HarrySpoelstra @mrmickme @C_A_Gustave @arijitchakrav @outbreakupdates
@ejustin46 - Emmanuel
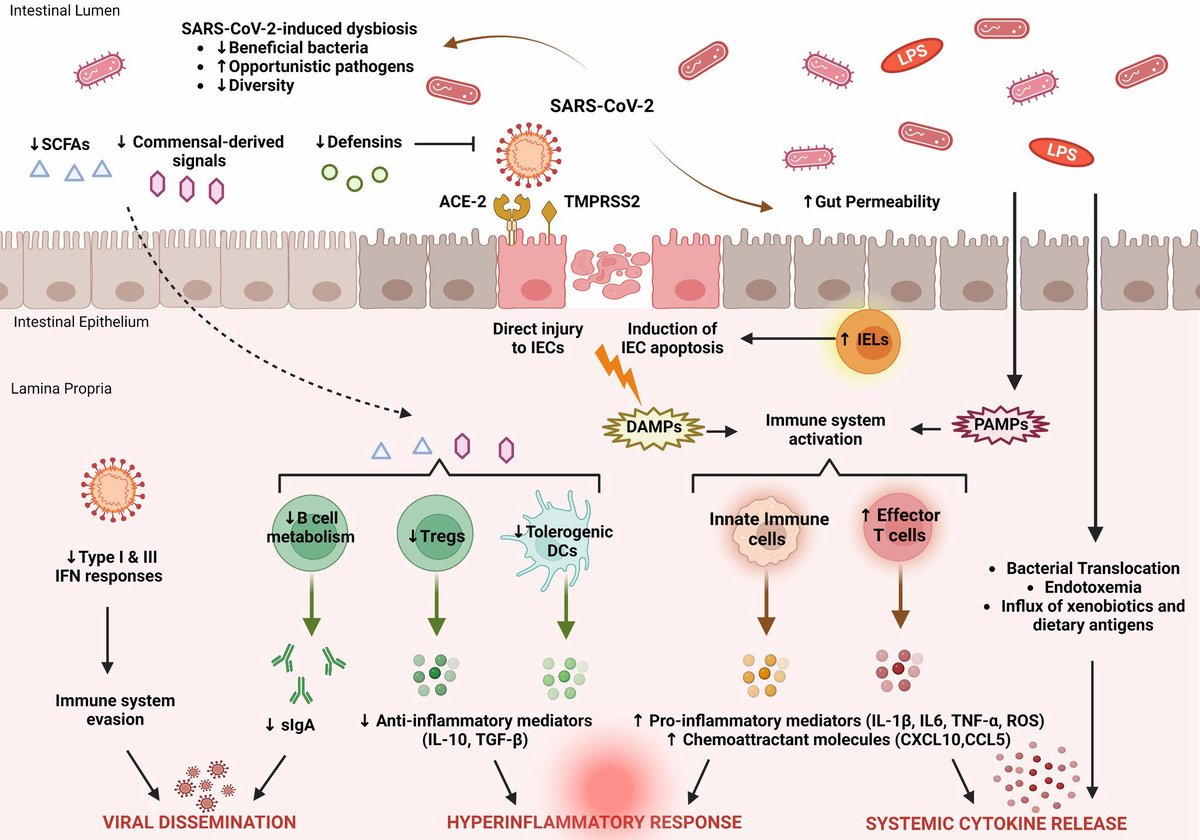
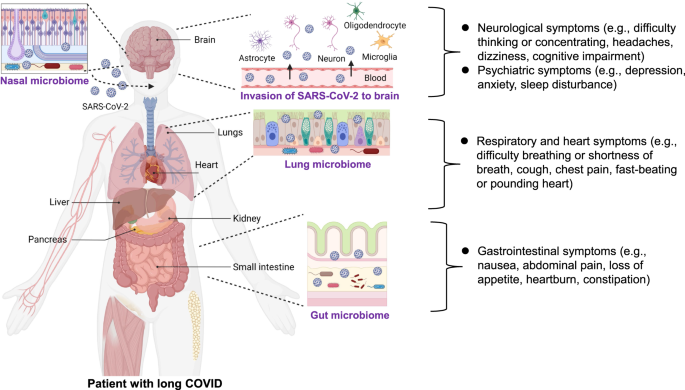
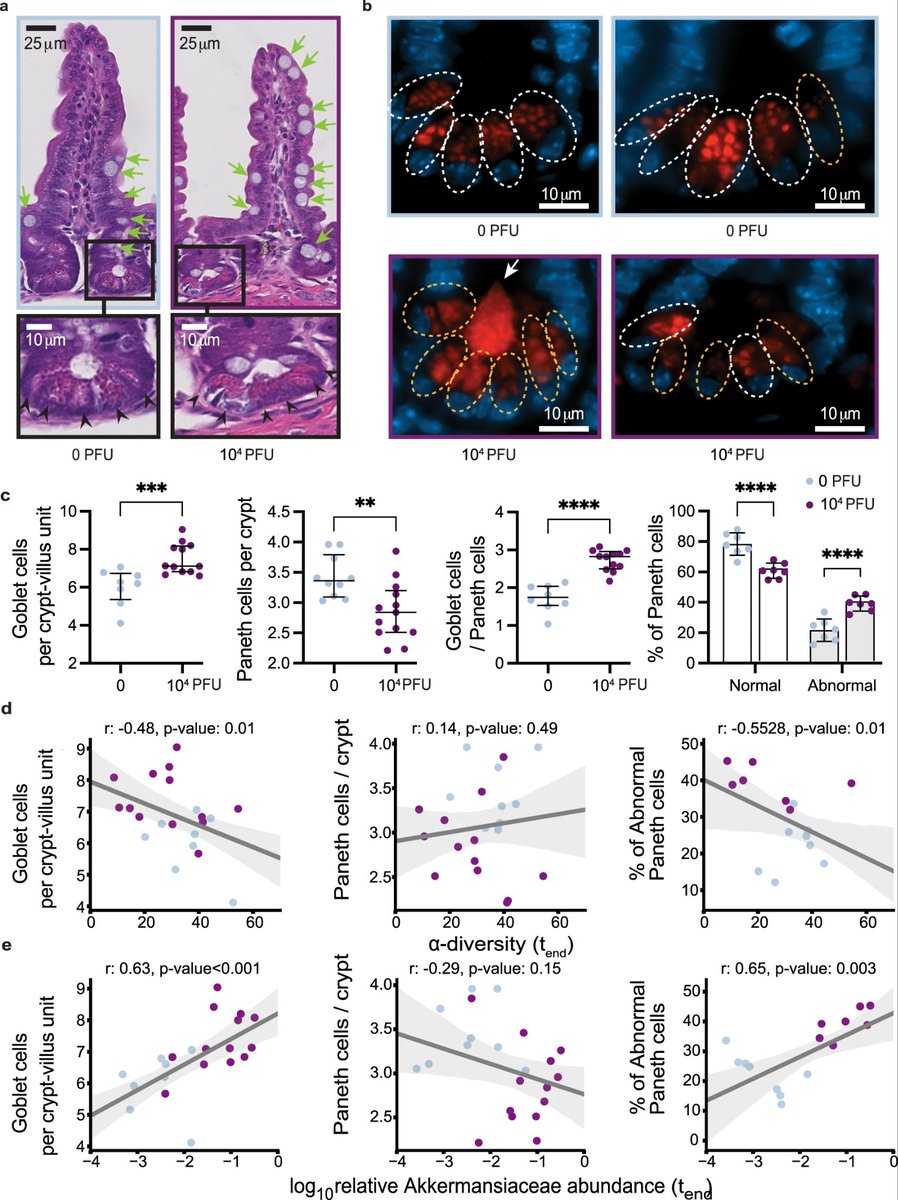
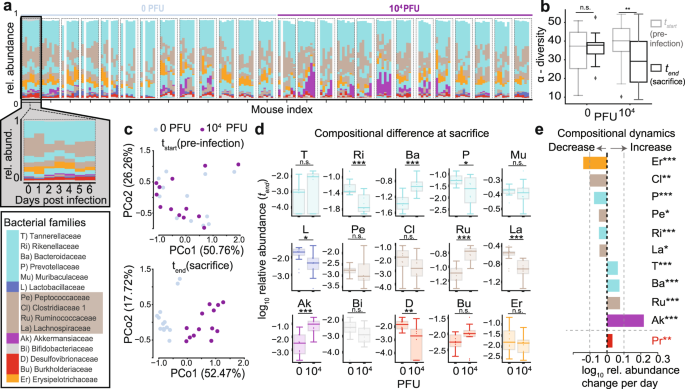
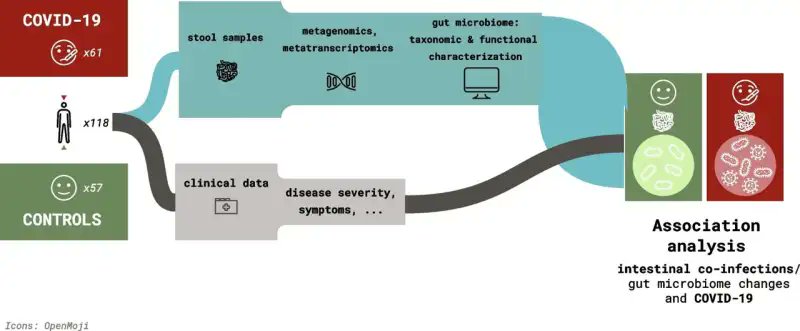
@MeetJess @LauraMiers @DavidJoffe64 @RadCentrism @HarrySpoelstra @mrmickme @C_A_Gustave @arijitchakrav @outbreakupdates NEW STUDY "Emerging evidence suggests that the gastrointestinal (GI) tract is also affected, with angiotensin-converting enzyme 2, a key receptor for SARS-CoV-2, abundantly expressed in the ileum and colon" https://www.biorxiv.org/content/10.1101/2023.11.29.568526v1


@ejustin46 - Emmanuel
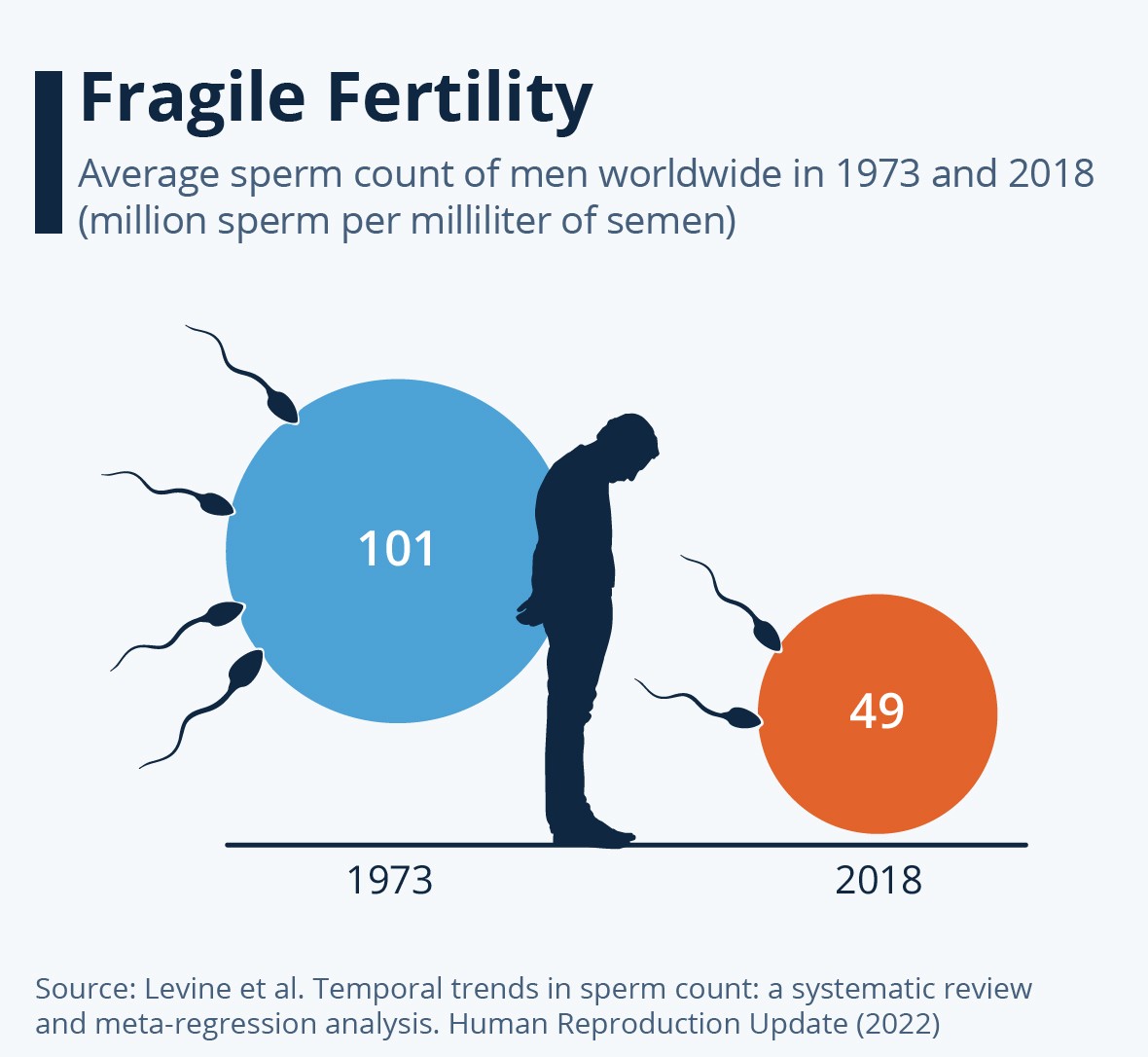
𝙏𝙃𝙀𝙔 𝙒𝘼𝙉𝙏 𝙐𝙎 𝙩𝙤 𝘽𝙀 𝙁𝙀𝙒𝙀𝙍 𝙤𝙣 𝙀𝘼𝙍𝙏𝙃 ? 𝘔𝘦𝘨𝘢-𝘵𝘩𝘳𝘦𝘢𝘥 𝘚𝘈𝘙𝘚-𝘊𝘖𝘝-2 𝘢𝘯𝘥 𝘚𝘗𝘌𝘙𝘔 It's a silent pandemic. Before SARS-COV-2, sperm counts drop was accelerating worldwide. This could go even faster with COVID-19 ! https://euronews.com/health/2022/11/15/sperm-count-drop-is-accelerating-worldwide-and-threatens-the-future-of-mankind-study-warns

@ejustin46 - Emmanuel
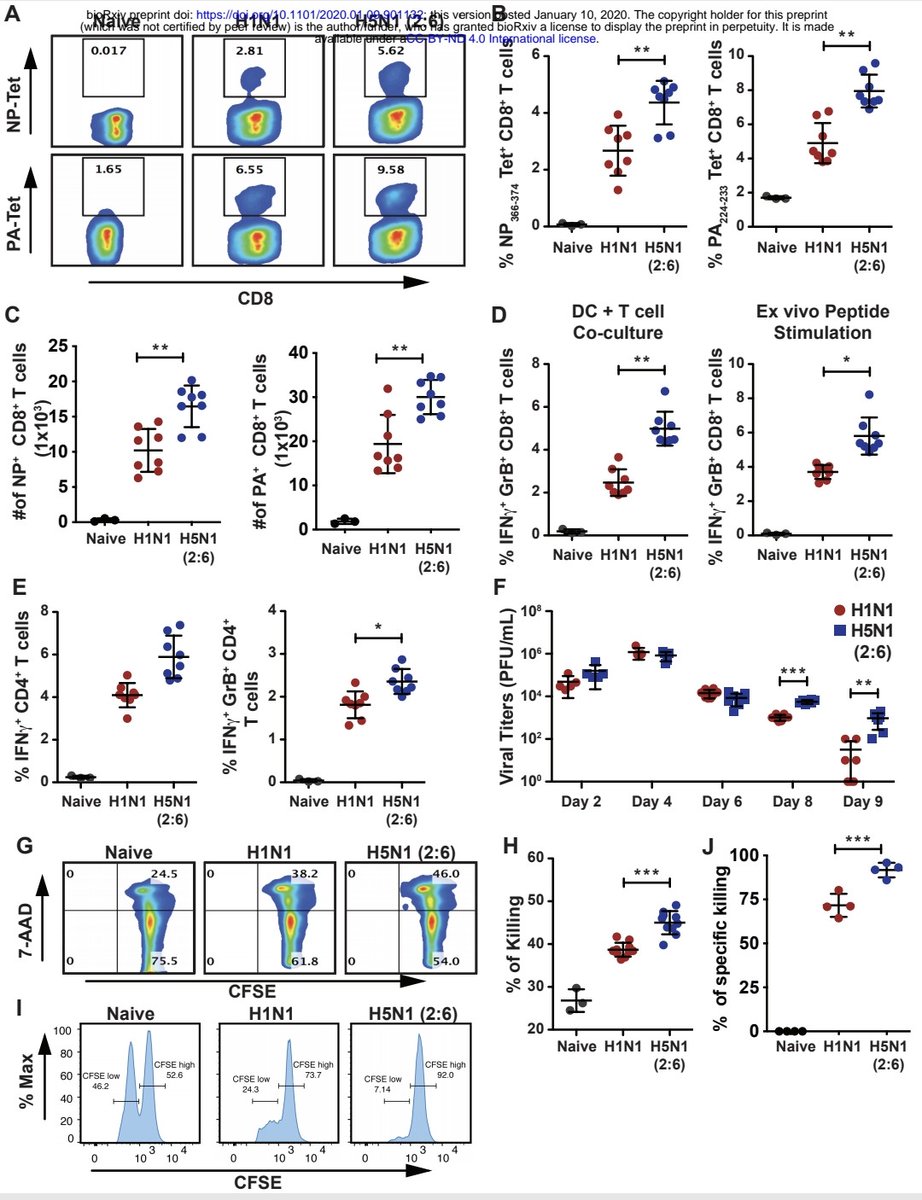
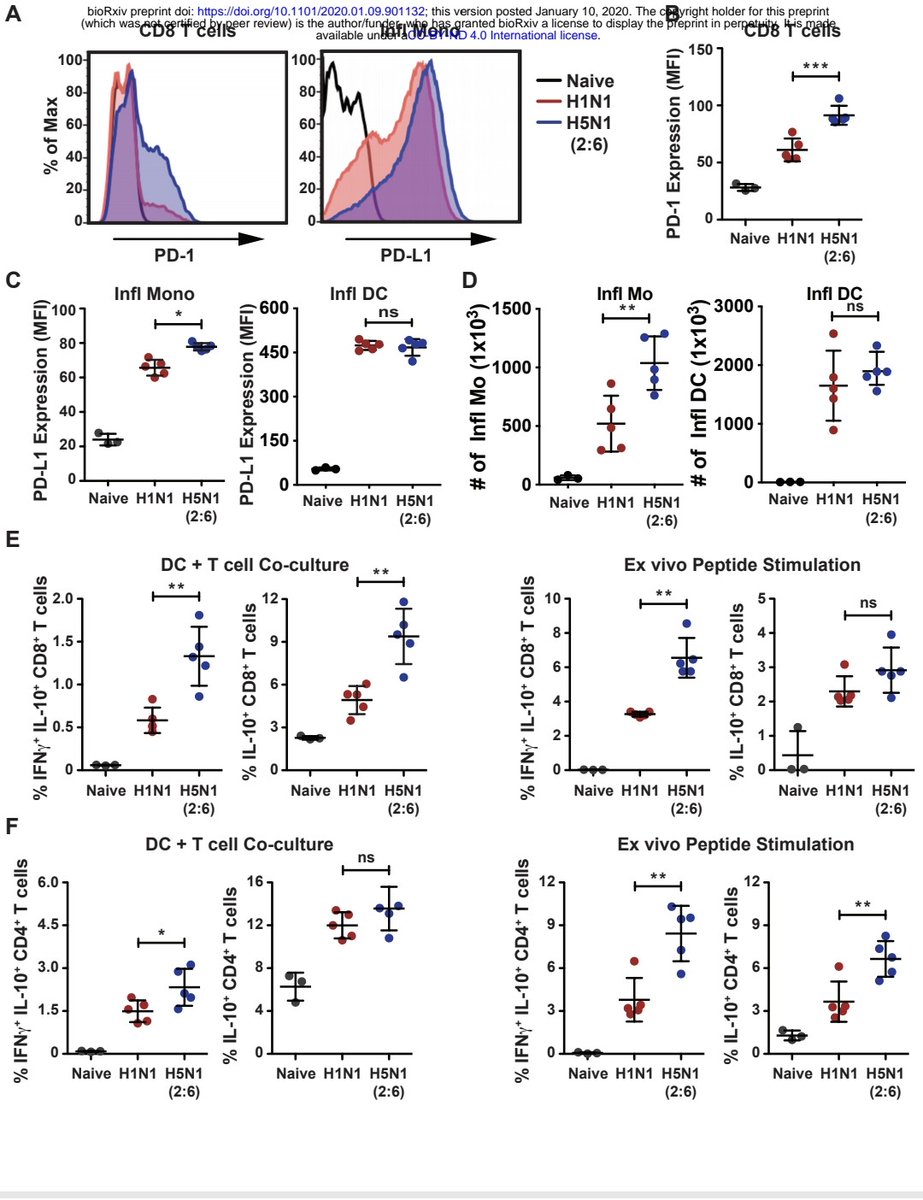
𝙃5𝙉1 𝙖𝙣𝙙 𝙎𝘼𝙍𝙎-𝘾𝙊𝙑-2, "𝘽𝙧𝙤𝙩𝙝𝙚𝙧𝙨 𝙞𝙣 𝙖𝙧𝙢𝙨" ? "𝘚𝘶𝘱𝘱𝘳𝘦𝘴𝘴𝘪𝘰𝘯 𝘰𝘧 𝘊𝘺𝘵𝘰𝘵𝘰𝘹𝘪𝘤 𝘛 𝘊𝘦𝘭𝘭 𝘍𝘶𝘯𝘤𝘵𝘪𝘰𝘯𝘴 𝘢𝘯𝘥 𝘋𝘦𝘤𝘳𝘦𝘢𝘴𝘦𝘥 𝘓𝘦𝘷𝘦𝘭𝘴 𝘰𝘧 𝘛𝘪𝘴𝘴𝘶𝘦 𝘙𝘦𝘴𝘪𝘥𝘦𝘯𝘵 𝘔𝘦𝘮𝘰𝘳𝘺 𝘛 𝘤𝘦𝘭𝘭" https://biorxiv.org/content/10.1101/2020.01.09.901132v1

@ejustin46 - Emmanuel
2) The study investigated how excessive innate immune responses to H5N1 avian influenza virus impair subsequent adaptive T cell responses. Infection with a recombinant H5N1 virus carrying the internal genes of H1N1 (H5N1(2:6)) induced higher activation of lung dendritic cells.. https://t.co/ga4Rwf1RO6
@ejustin46 - Emmanuel
3) ...compared to infection with H1N1 alone. H5N1(2:6) infection led to increased migration of lung dendritic cells to the draining lymph nodes, resulting in robust activation of virus-specific CD8+ and CD4+ T cell responses in the lungs. https://t.co/rUJ37DscQB
@ejustin46 - Emmanuel
4) Despite mounting strong T cell responses, mice infected with H5N1(2:6) showed delayed viral clearance from the lungs compared to H1N1 infection. T cells from H5N1(2:6)-infected mice expressed higher levels of the inhibitory marker PD-1 and produced more ... https://t.co/WQKrxFncN5
@ejustin46 - Emmanuel
5) ...of the anti-inflammatory cytokine IL-10, suggesting suppression of cytotoxic T cell functions. H5N1(2:6) infection also resulted in decreased numbers of lung-resident memory T cells compared to H1N1 infection. https://t.co/Tr3bT7Hrqs
@ejustin46 - Emmanuel
6) In conclusion, hyperactivation of the innate immune response by H5N1 impairs T cell responses and delays viral clearance by inducing inhibitory mechanisms like PD-1 and IL-10. This helps explain the severe disease associated with H5N1 infections. https://t.co/AjetggWSpe

@ejustin46 - Emmanuel
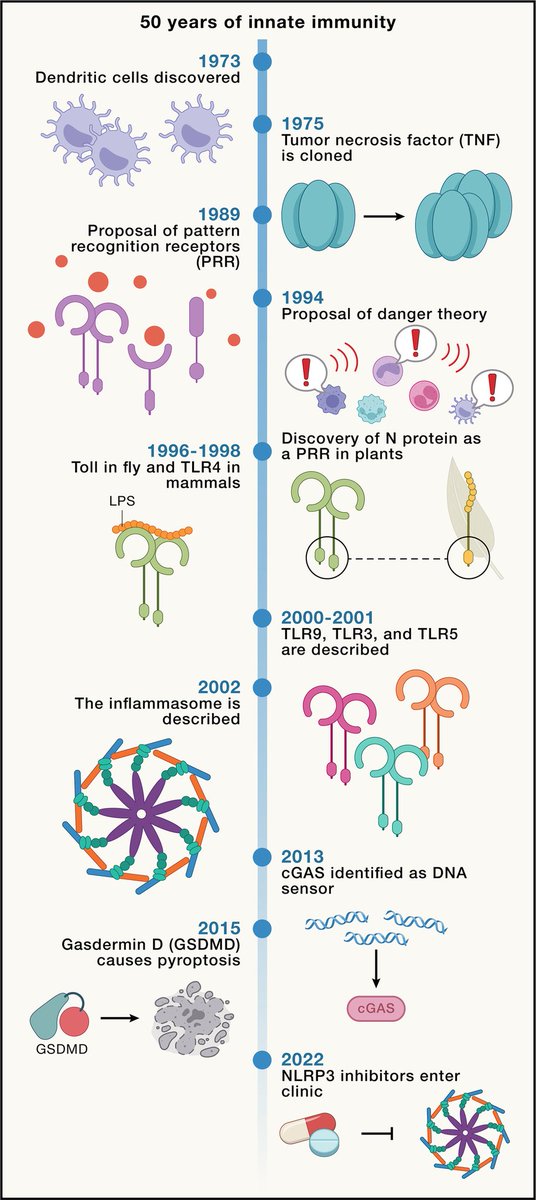
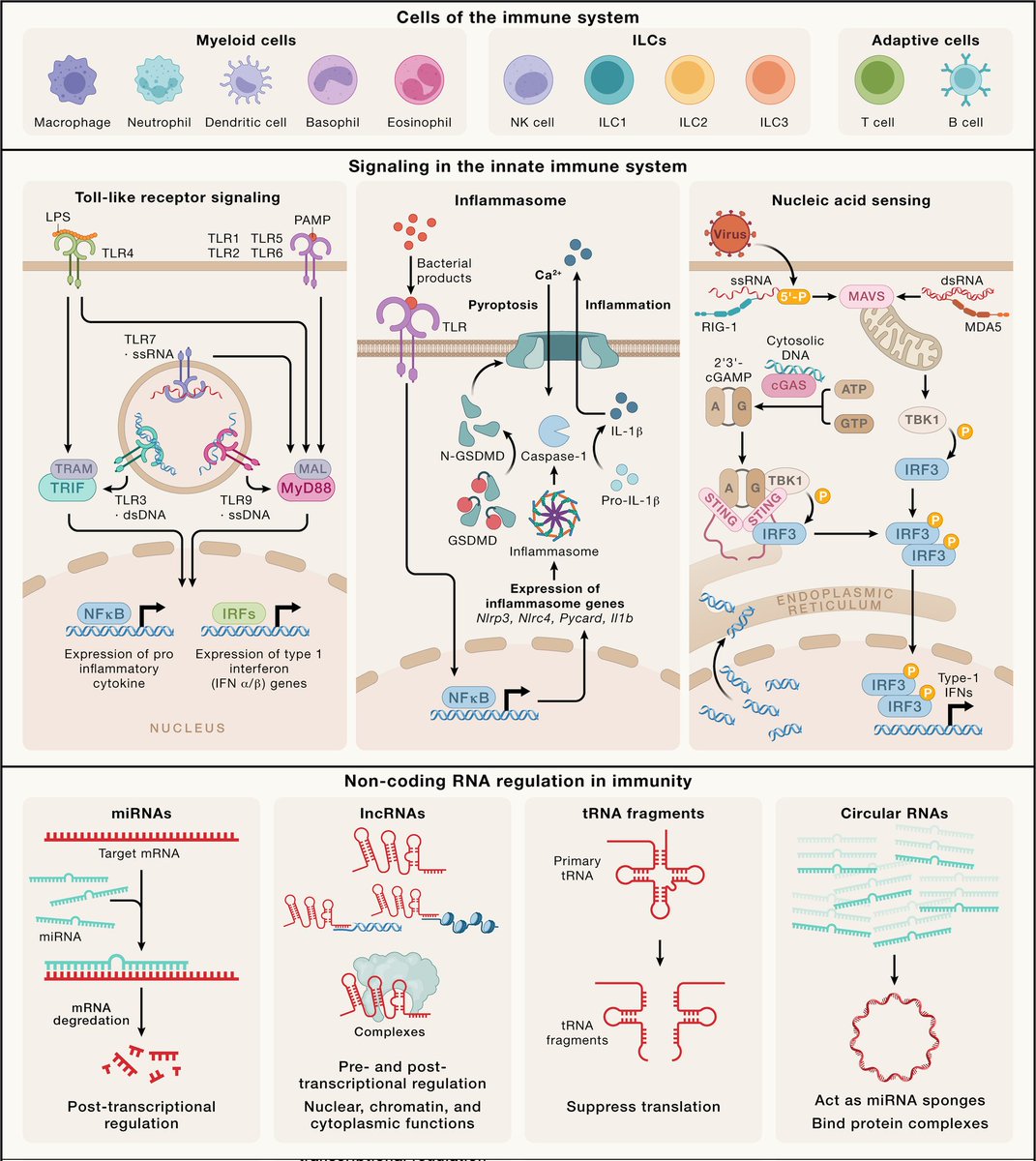
𝙁𝙧𝙤𝙢 𝙥𝙚𝙧𝙞𝙥𝙝𝙚𝙧𝙮 𝙩𝙤 𝙘𝙚𝙣𝙩𝙚𝙧 𝙨𝙩𝙖𝙜𝙚: 50 𝙮𝙚𝙖𝙧𝙨 𝙤𝙛 𝙖𝙙𝙫𝙖𝙣𝙘𝙚𝙢𝙚𝙣𝙩𝙨 𝙞𝙣 𝙞𝙣𝙣𝙖𝙩𝙚 𝙞𝙢𝙢𝙪𝙣𝙞𝙩𝙮 https://www.cell.com/cell/fulltext/S0092-8674(24)00352-0 https://t.co/yxn9szx2ns
@ejustin46 - Emmanuel
2) Innate immunity was long overlooked compared to adaptive immunity, but over the past 50 years research has revealed it to be a highly sophisticated and interconnected system. https://t.co/1vjgX8dk0W
@ejustin46 - Emmanuel
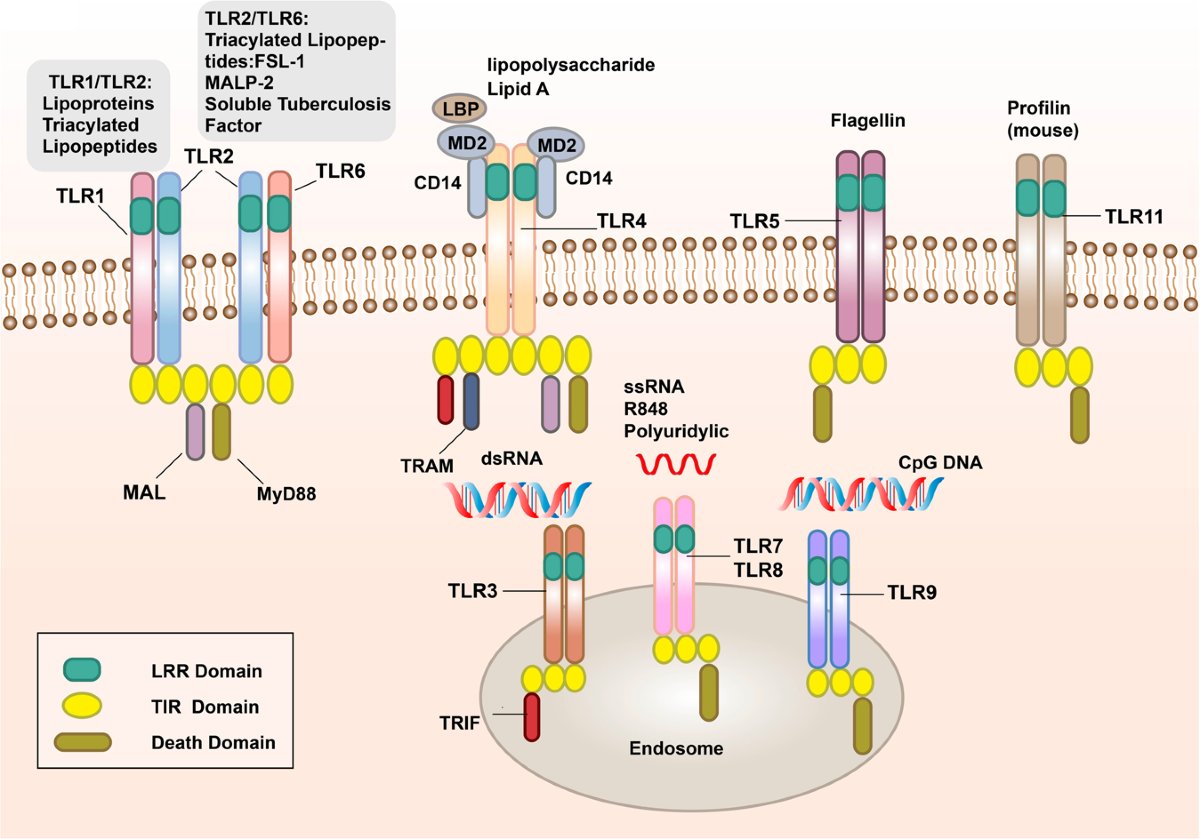
3) Major discoveries include pathogen recognition receptors (PRRs) like Toll-like receptors (TLRs) and Nod-like receptors (NLRs), which detect pathogens and damage. This links innate and adaptive immunity. https://t.co/ybMI7w0thl
@ejustin46 - Emmanuel
4) Cytokines were found to control physiological responses and link innate cells like macrophages to adaptive lymphocytes. Factors like INF-b are critical antiviral messengers. https://t.co/sY4VqRUtfp
@ejustin46 - Emmanuel
5) Inflammasomes are multiprotein complexes containing NLR sensors like NLRP3 that activate caspase-1 and IL-1b/IL-18 release in response to microbes and danger signals. https://t.co/55TxEgCQJG
@ejustin46 - Emmanuel
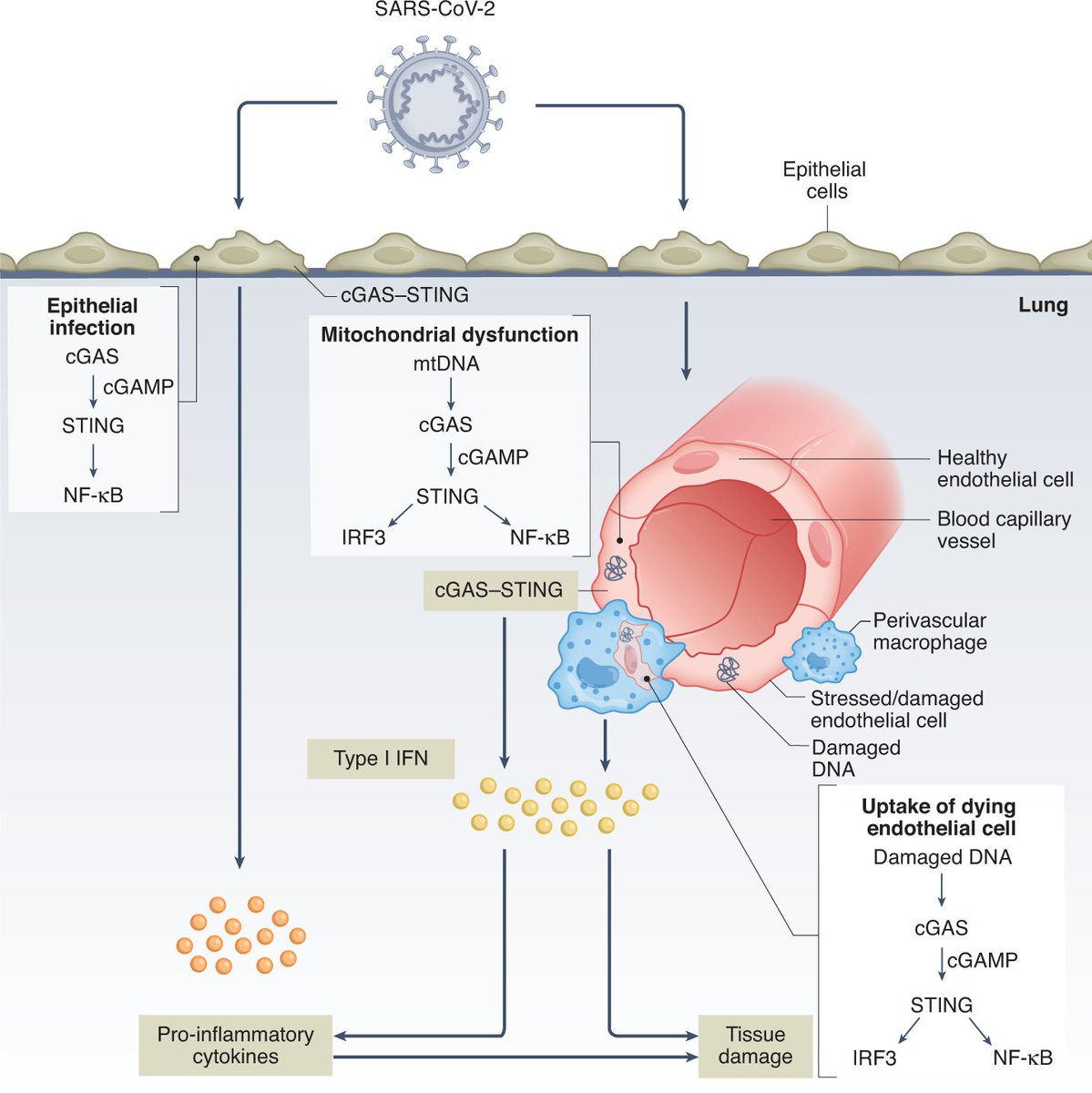
6) DNA and RNA sensing pathways involving cGAS, STING, RIG-I and MDA-5 were uncovered to induce type I interferons. This revealed DNA as an innate immune trigger. https://t.co/rpXJfxNoAA
@ejustin46 - Emmanuel
7) Dendritic cells were shown to capture antigens, mature via TLR signals, and present to T cells, linking innate and adaptive responses. https://t.co/OaiZYR3mbC
@ejustin46 - Emmanuel
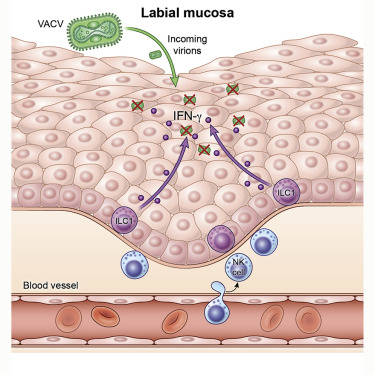
8) Innate lymphoid cells (ILCs) were characterized as innate counterparts to T cell subsets without rearranged receptors. https://t.co/yDhTUsUDDg
@ejustin46 - Emmanuel
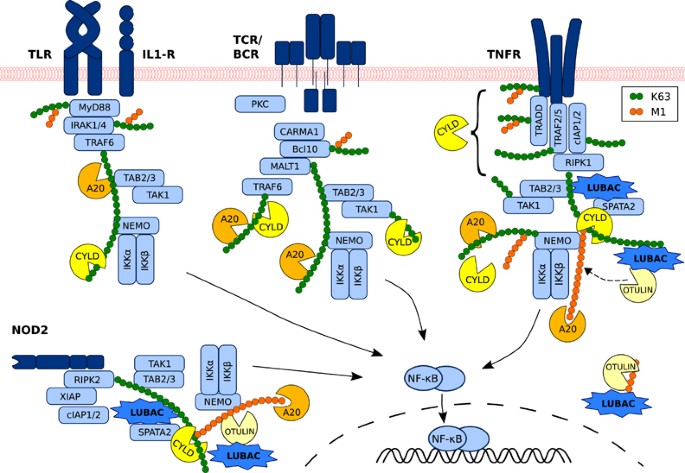
9) Complex controls on signaling were discovered including A20, CYLD and SOCS1 negative regulators and how ubiquitination shapes responses. https://t.co/7TxmOXhWFm
@ejustin46 - Emmanuel
10) MicroRNAs and long noncoding RNAs emerged as key post-transcriptional regulators of innate immunity genes. https://t.co/9HYcUC8pNw
@ejustin46 - Emmanuel
11) Therapeutics have targeted cytokines and aim to modulate PRR pathways for vaccines, sepsis, and autoinflammation. NLRP3 inhibitors show promise.
@ejustin46 - Emmanuel
12) In summary, detailed study over decades has transformed our understanding of innate immunity from a simple barrier system to a sophisticated network central to health and disease. https://t.co/nQcwzHknua

@ejustin46 - Emmanuel
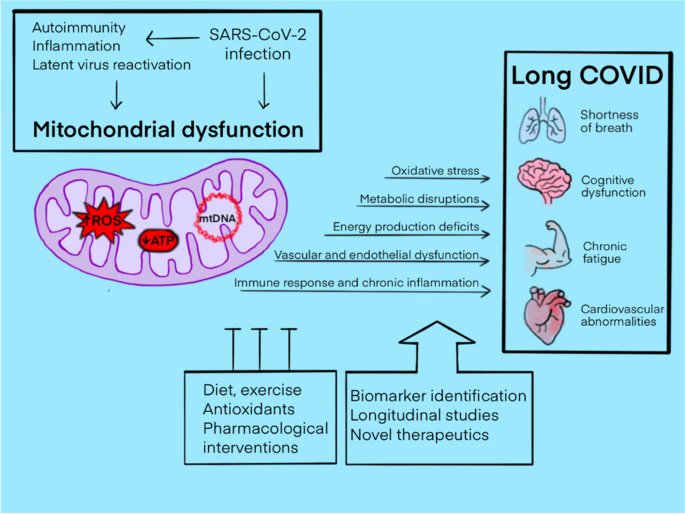
𝗠𝗶𝘁𝗼𝗰𝗵𝗼𝗻𝗱𝗿𝗶𝗮𝗹 𝗱𝘆𝘀𝗳𝘂𝗻𝗰𝘁𝗶𝗼𝗻 𝗶𝗻 𝗹𝗼𝗻𝗴 𝗖𝗢𝗩𝗜𝗗 https://link.springer.com/article/10.1007/s11357-024-01165-5

@ejustin46 - Emmanuel
2) Mitochondrial dysfunction has emerged as a prominent factor contributing to the diverse and persistent symptoms observed in patients with long COVID syndrome. Impaired mitochondrial function could underlie symptoms like chronic fatigue, cognitive issues ... https://t.co/SND0qt9xbx
@ejustin46 - Emmanuel
3) ...and muscle weakness through mechanisms like reduced energy production and increased oxidative stress. Evidence of mitochondrial dysfunction in long COVID comes from studies showing abnormalities in mitochondrial respiration, gene expression, and ...
@ejustin46 - Emmanuel
4) ... metabolite levels in patient samples. Biomarkers of oxidative stress and mitochondrial damage have also been found to be elevated. Mitochondrial dysfunction may persist via mechanisms like direct viral damage, immune-mediated effects, impaired biogenesis pathways ... https://t.co/UtIwFIK1qQ
@ejustin46 - Emmanuel
5) ...or secondary impacts on metabolism and vascular health. Similar mitochondrial abnormalities have been observed in other post-infectious conditions like myalgic encephalomyelitis/chronic fatigue syndrome, post-treatment Lyme disease, and persistent Epstein-Barr infection.
@ejustin46 - Emmanuel
6) Targeting mitochondrial function through pharmacological interventions, lifestyle modifications, exercise, and nutritional support holds promise as a therapeutic approach for managing long COVID symptoms. Some mitochondrial antioxidants are already being tested clinically. https://t.co/Twf0wiKb91


@ejustin46 - Emmanuel
𝗦𝗔𝗥𝗦-𝗖𝗢𝗩-2, 𝗩𝗜𝗥𝗔𝗟 𝗣𝗘𝗥𝗦𝗜𝗦𝗧𝗘𝗡𝗖𝗘 𝙏𝙞𝙢𝙚 𝙙𝙤𝙚𝙨𝙣'𝙩 𝙥𝙖𝙨𝙨, 𝙞𝙩 𝙨𝙚𝙩𝙩𝙡𝙚𝙨 ! (𝘮𝘦𝘨𝘢-𝘵𝘩𝘳𝘦𝘢𝘥) Time and the SARS-CoV-2 virus do share some similarities in terms of how they affect our lives. Time, as a concept, cannot be eliminated ... https://t.co/atcg9uYE4C

@ejustin46 - Emmanuel
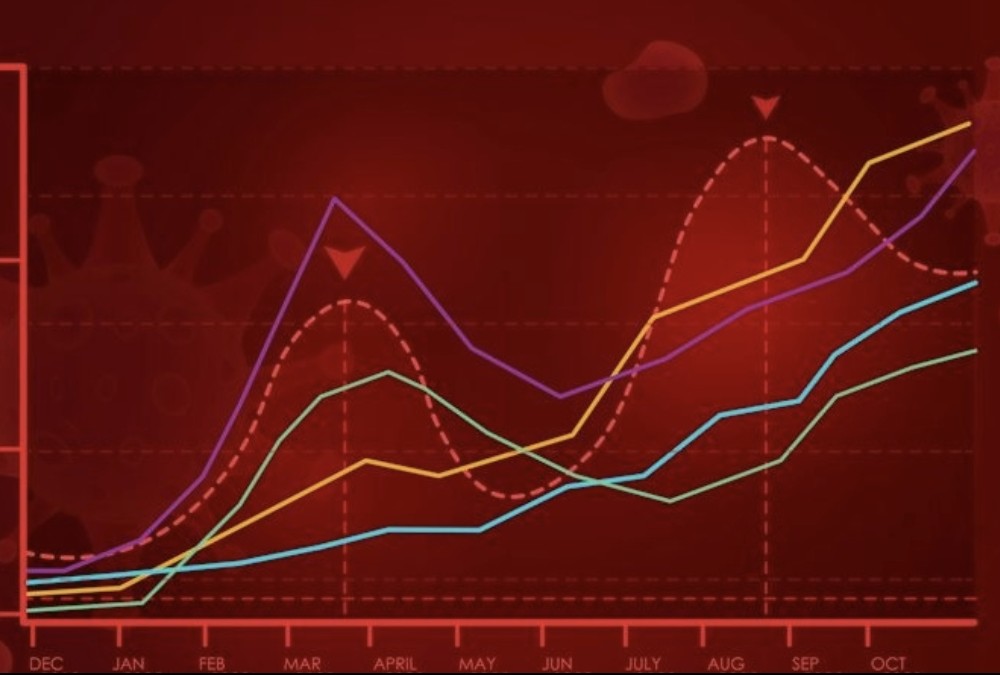
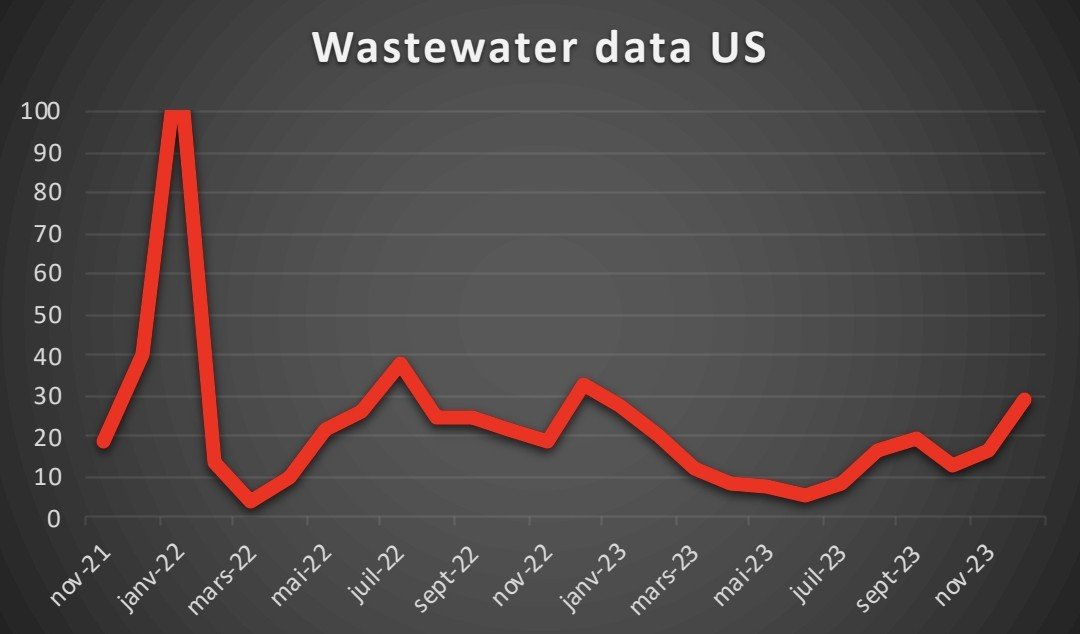
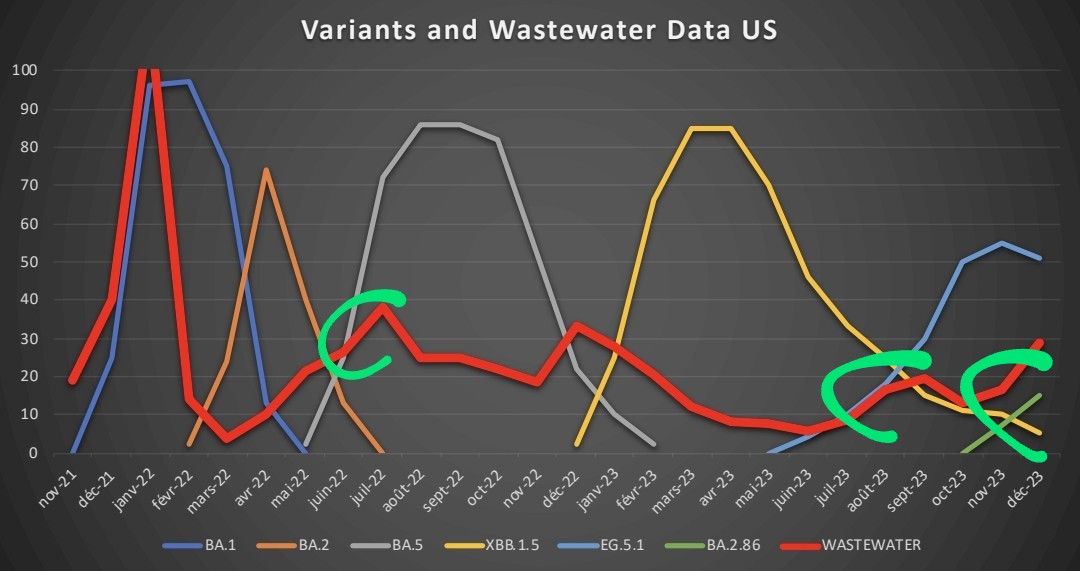
VARIANTS and WASTEWATER : SOMETHING HAS CHANGED ! Since Omicron, we have witnessed a "desynchronization", between the emergence of variants and the waves, between the intra-host and inter-host transmission. We took the example of the US to try to explain this phenomenon.
@ejustin46 - Emmanuel
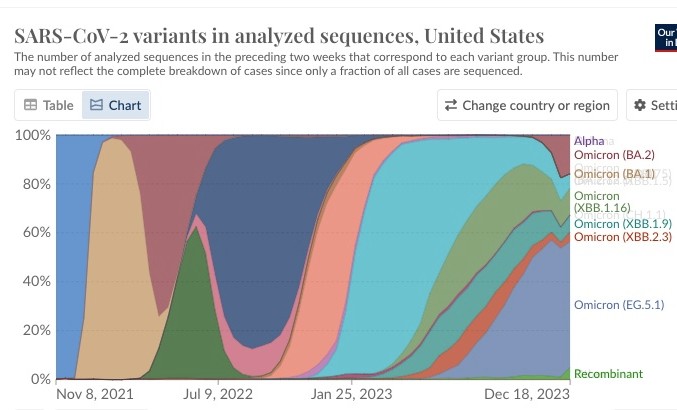
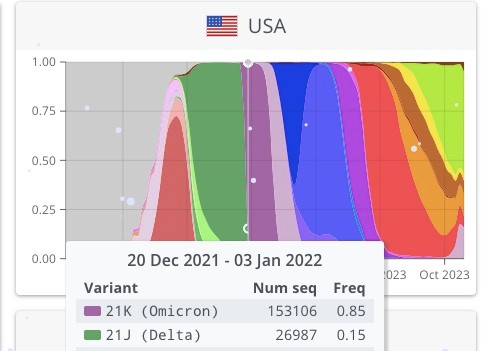
2) After BA.1, we have seen a succession of variants, detected thanks to the great work of "variants trackers".
@ejustin46 - Emmanuel
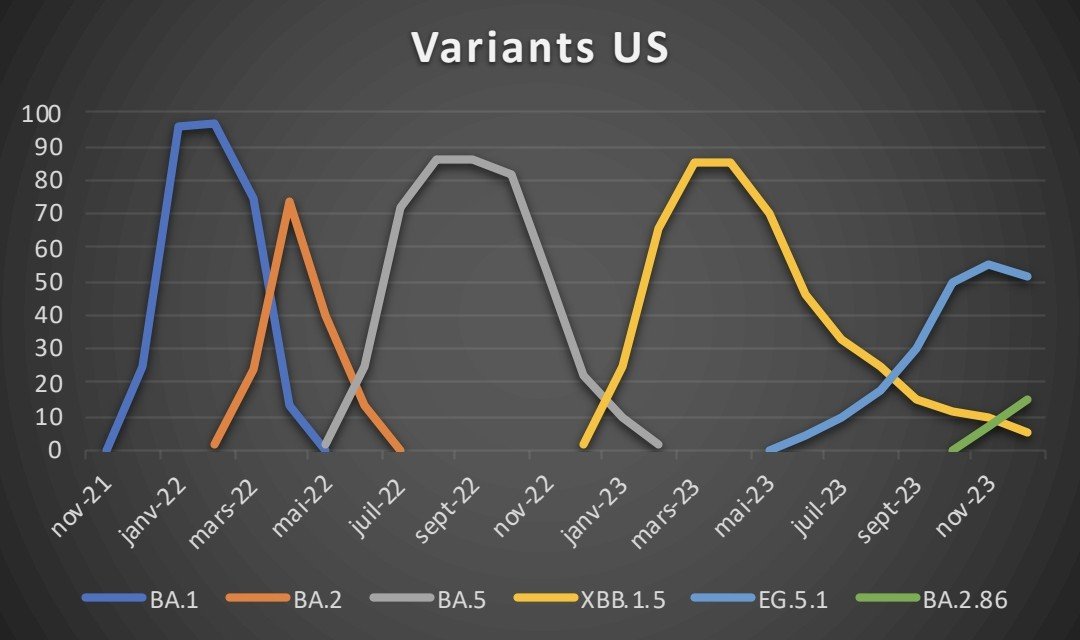
3) For this analysis, we retained the 5 large families of variants in the US post BA.1*: BA.2*, BA.5*, XBB.1.5*, EG.5.1* and BA.2.86* For simplicity we have inputed the % of sequences on a biweekly frequency.
@ejustin46 - Emmanuel
4) Then we re-processed the Biobot data by taking 3.665 copies/ml as base 100, which is almost the highest value of viral circulation since 2 years.
@ejustin46 - Emmanuel
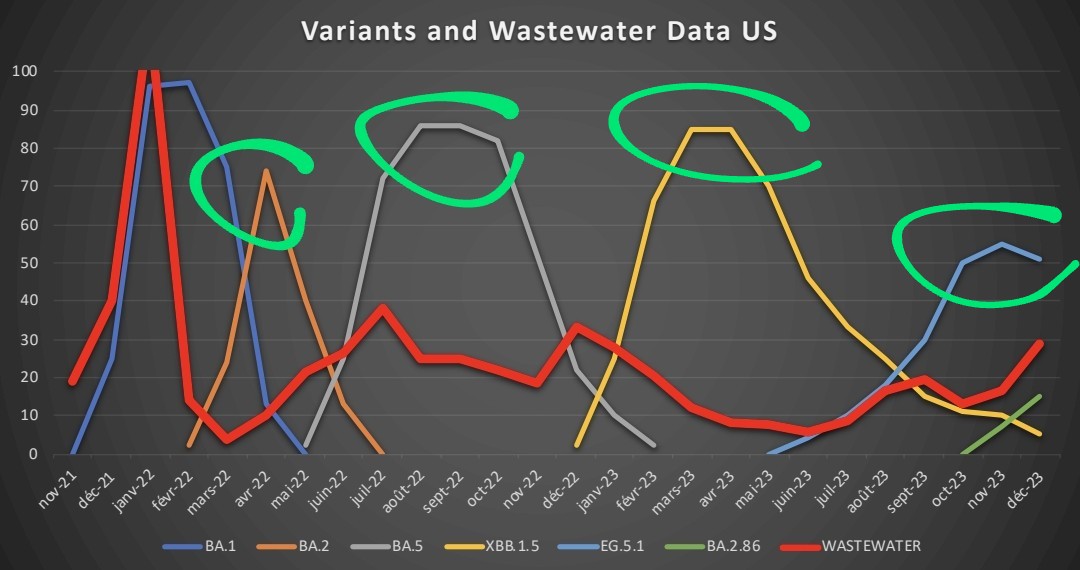
5) When we superimpose the two graphs, we see that over very short periods, the emergence of a variant "can give" the impression to be the driver of a wave.
@ejustin46 - Emmanuel
6) But overall, the periods where the % of sequences is the highest, are disconnected from the waves. How to explain this?
@ejustin46 - Emmanuel
7) DISCUSSION. We have been widely criticized (and even blocked by some) who accuse us of minimizing the impact and danger of the new variants, which is totally absurd ! If inter-host transmission (transmission of the virus from one infected individual to another and not within
@ejustin46 - Emmanuel
8) ... an individual) has become predominant, it is because the landscape in which the variants evolve has profoundly changed. When in less than a year you have an incredible increase in the nb of antibodies within the population, we cannot ignore this change of the landscape.
@ejustin46 - Emmanuel
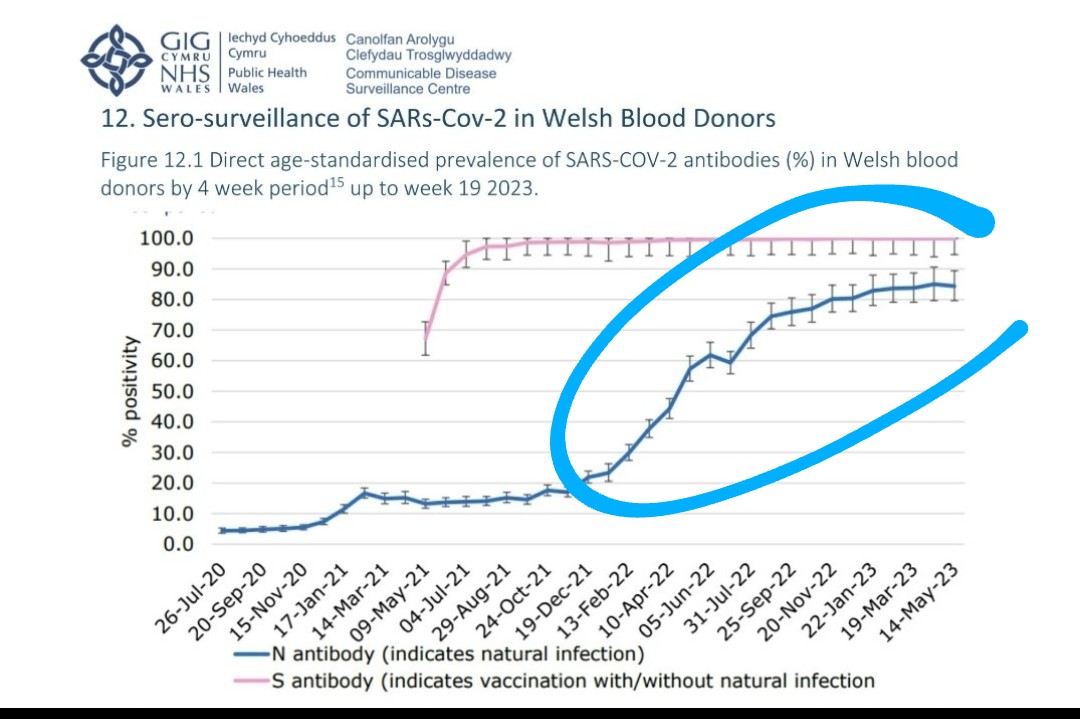
9) Certainly we have a very rapid waning immunity, but immunity is not limited to the sole action of N and S antibodies. There is also the action of B cells and those of T cells. https://www.biorxiv.org/content/10.1101/2023.12.19.572339v1

@ejustin46 - Emmanuel
10) Far be it from us, to minimize the weakening of the immune system following multiple reinfections, and the abandonment of protective measures which allow the virus to circulate on a large scale throughout the planet. https://t.co/Sj1nYAJyQo
@ejustin46 - Emmanuel
11) We could also mention environmental factors, the increase of the pollution, the transmission of the virus in areas with high population density, the change of population movement, or the role of superspreaders, etc. https://t.co/cNn6qxGJce
@ejustin46 - Emmanuel
12) By mixing protective measures such as vaccines, and those of absence of protection such as stopping the masks, we have created an "epidemiological chaos" and totally disrupted the way the virus circulates. https://t.co/jVZGKT3JQd
@ejustin46 - Emmanuel
13) CONCLUSION Let those who challenge these analyzes provide contradictory data. I was in Eastern countries when the Berlin Wall fell, in Bucharest when Ceausescu fell, in Shanghai when Google Search was blocked, and in so many countries where you live on the ground ... https://t.co/HeyoPgNg96
@ejustin46 - Emmanuel
14) ... what means the restrictions of fundamental freedoms. Let's hope that X/Twitter remains a place of debate and exchange ...and not of exclusion of those who express a different analyzes of the pandemic. https://t.co/AO6pL14YG6
@ejustin46 - Emmanuel
15) Thanks for reading 🙏 FYI @DavidJoffe64 @UseBy2022 @C_A_G0101 @gianlucac1 @gwladwr @falsel_net @RadCentrism @LongDesertTrain @SolidEvidence @xabitron1 @shay_fleishon @siamosolocani @1goodtern @_CatintheHat @GourlaySyd @MeetJess @LauraMiers @michael_hoerger @outbreakupdates

@ejustin46 - Emmanuel
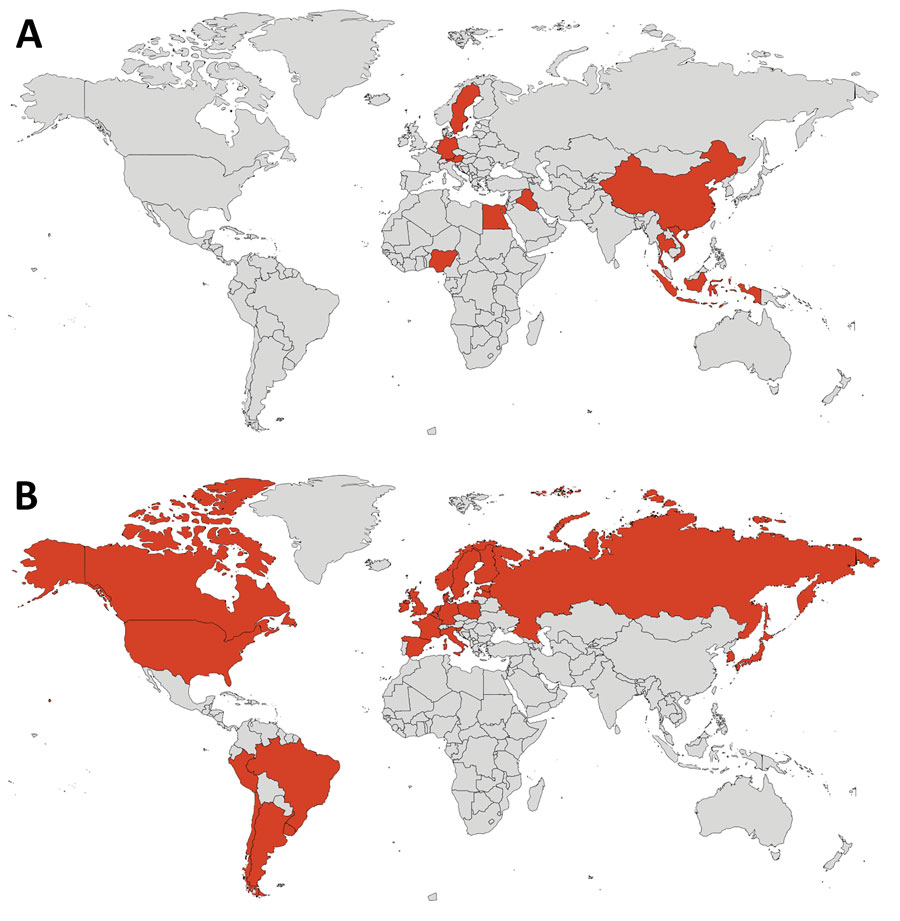
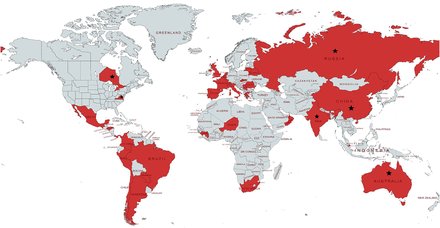
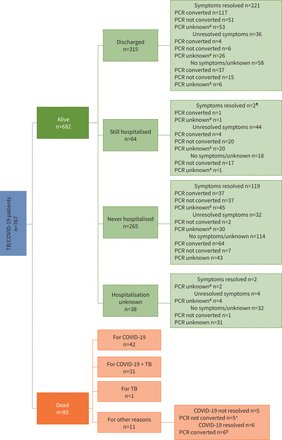
2) The study, (a recent version of which unfortunately is paywalled), raised the problem of tuberculosis and COVID-19 coinfection https://erj.ersjournals.com/content/59/3/2102538 Fig. Global distribution of the countries/states/regions participating in the study.

@ejustin46 - Emmanuel
3) Fig. Clinical outcome of coronavirus disease 2019 (COVID-19) among tuberculosis (TB)/COVID-19 patients https://t.co/wbEZKdoEV2
@ejustin46 - Emmanuel
4) 74% of the patients had TB diagnosed before COVID-19; 16.5% were diagnosed within the same week (the presence of signs and symptoms prompted the clinicians to undertake imaging, which revealed potentially pre-existing TB on top of COVID-19 and 9.5% had COVID-19 diagnosed first
@ejustin46 - Emmanuel
5) "A key question from our preliminary study was on the role of SARS-CoV-2 in the progression of TB infection to disease as observed in other viral diseases (e.g. HIV) A combination of post-COVID-19 and post-TB lung disease PTLD sequelae and the need for assessment ...
@ejustin46 - Emmanuel
6) and potential follow-up and rehabilitation can pose additional stress on health services in terms of human and economic resources. Thanks for reading 🙏 For those interested in this topic, here is the first mega-thread 👇 https://t.co/jIvYV0lk49

@ejustin46 - Emmanuel
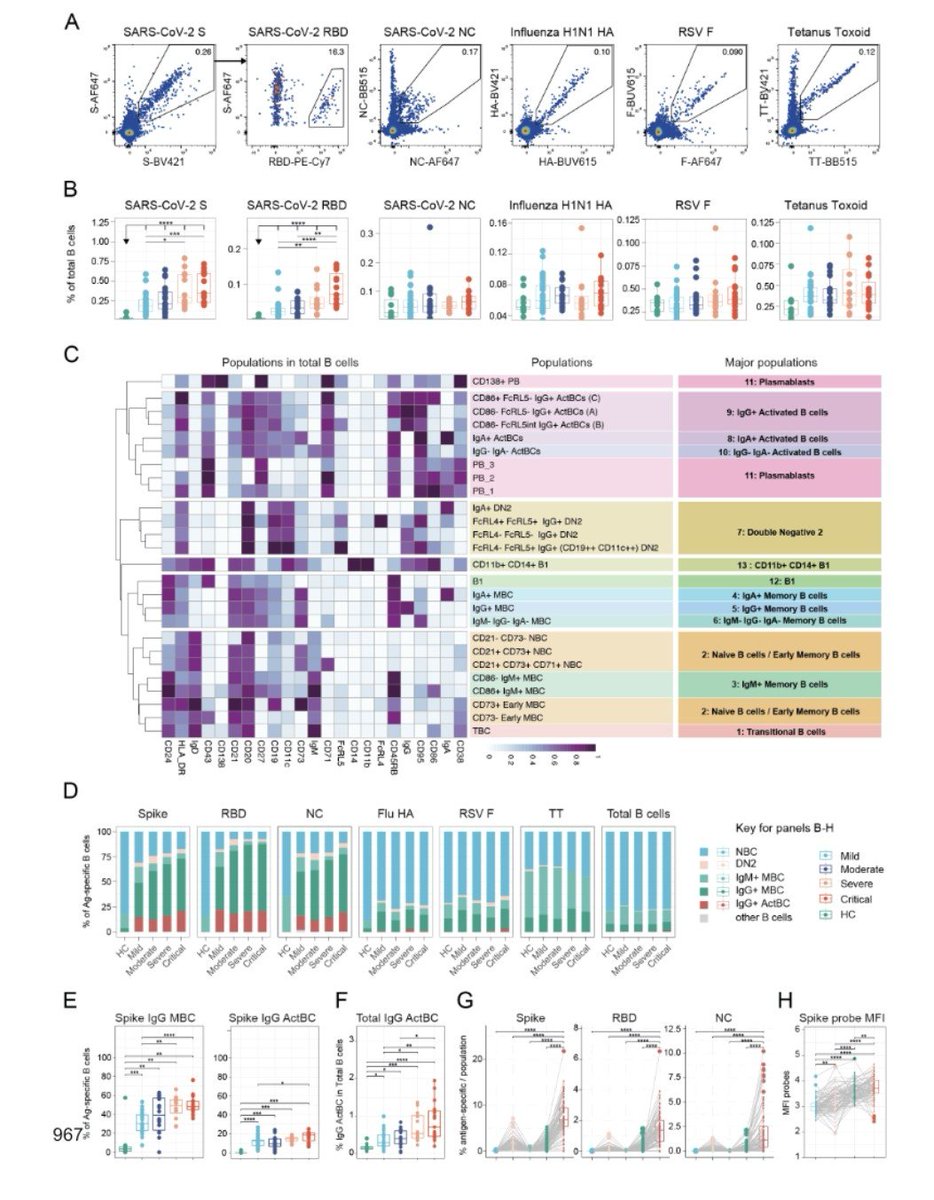
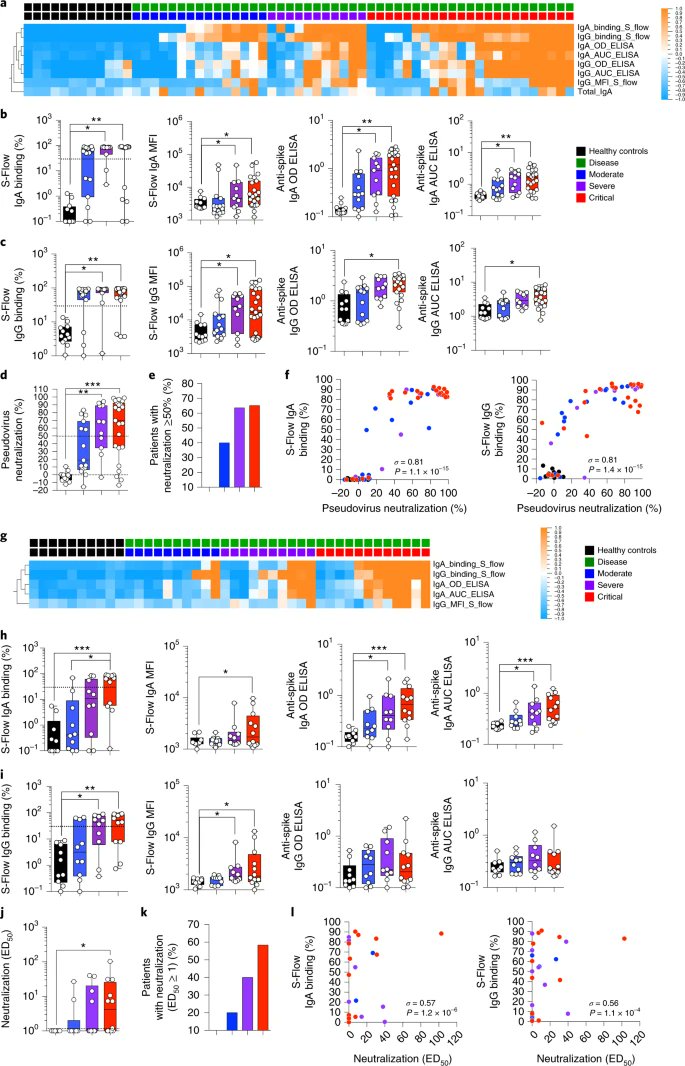
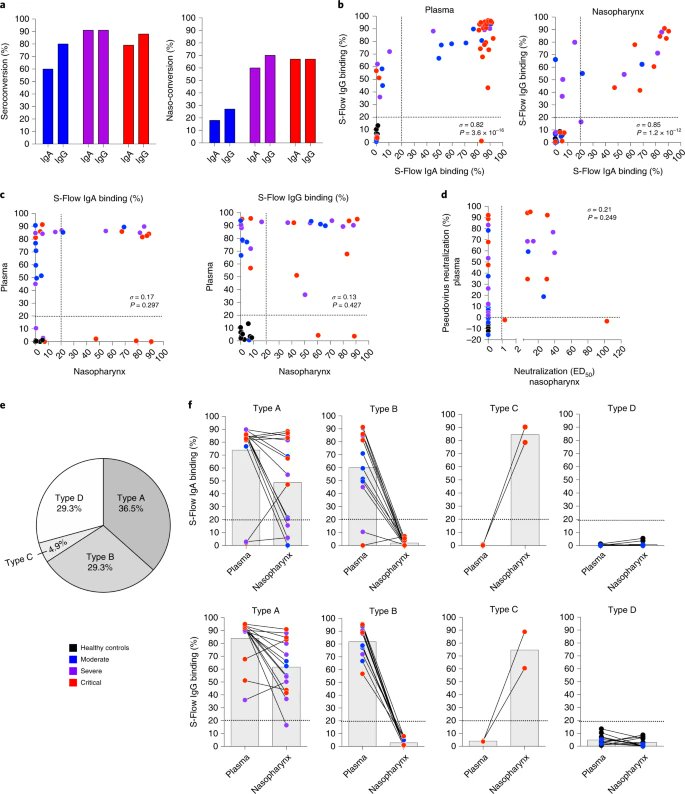
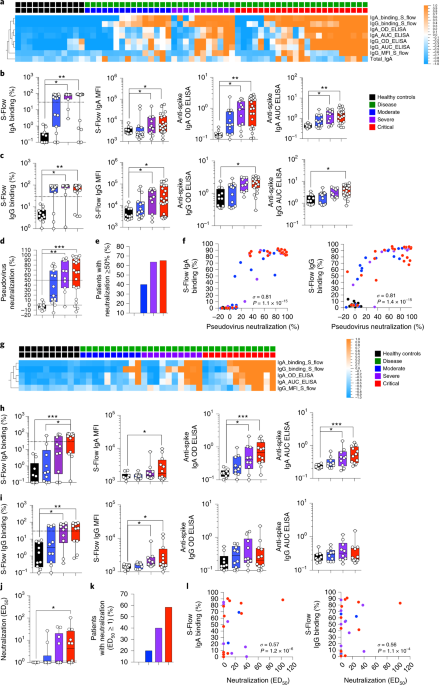
2) This study published 2 years ago already showed the heterogeneity of the immune response depending on the individual. "Distinct systemic and mucosal immune responses during acute SARS-CoV-2 infection"
@ejustin46 - Emmanuel
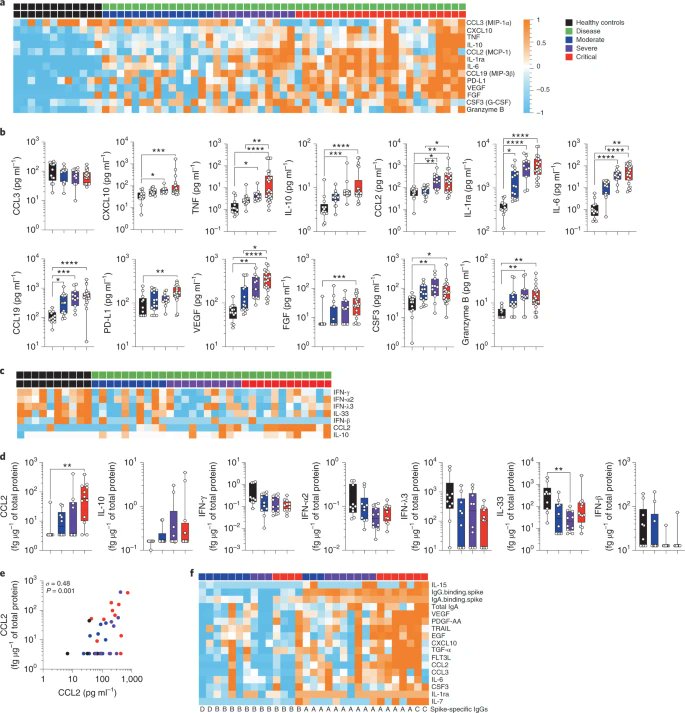
4) This difference in the immune response led to differential cytokine responses which stratify COVID-19 disease severity Fig. Systemic and mucosal cytokine production in patients with COVID-19.
@ejustin46 - Emmanuel
5) The most interesting part in our opinion was in the conclusion : "Analysis of the nasopharyngeal antibody response also revealed highly heterogenous responses. While the vast majority of patients generated systemic viral-specific antibodies,
@ejustin46 - Emmanuel
6) a surprisingly high proportion of patients had neither detectable viral-specific IgG nor IgA in their nasopharyngeal compartments"
@ejustin46 - Emmanuel
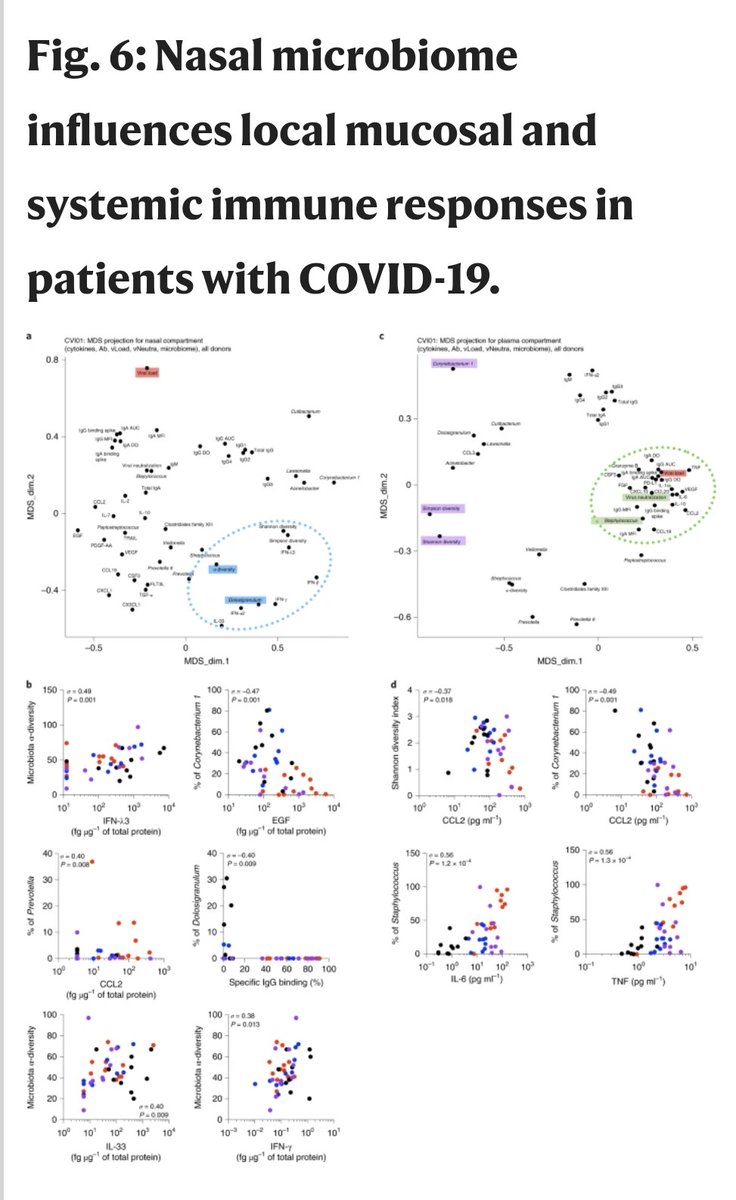
7) But above all : "Nasopharyngeal ‘dysbiosis’ may precede SARS-CoV-2 infection rendering these individuals more susceptible to COVID-19 morbidities. Previous studies have documented ‘pathobiont’ carriage (including Staphylococcus aureus, Streptococcus pneumoniae
@ejustin46 - Emmanuel
8) and Haemophilus influenzae) in up to 40% of healthy individuals. Our results suggest that these individuals may be at higher risk of developing severe COVID-19 disease, as SARS-CoV-2 infection would result in a breakdown of local epithelial barrier function" Thanks 🙏
@ejustin46 - Emmanuel
9) Reference https://www.nature.com/articles/s41590-021-01028-7

@ejustin46 - Emmanuel
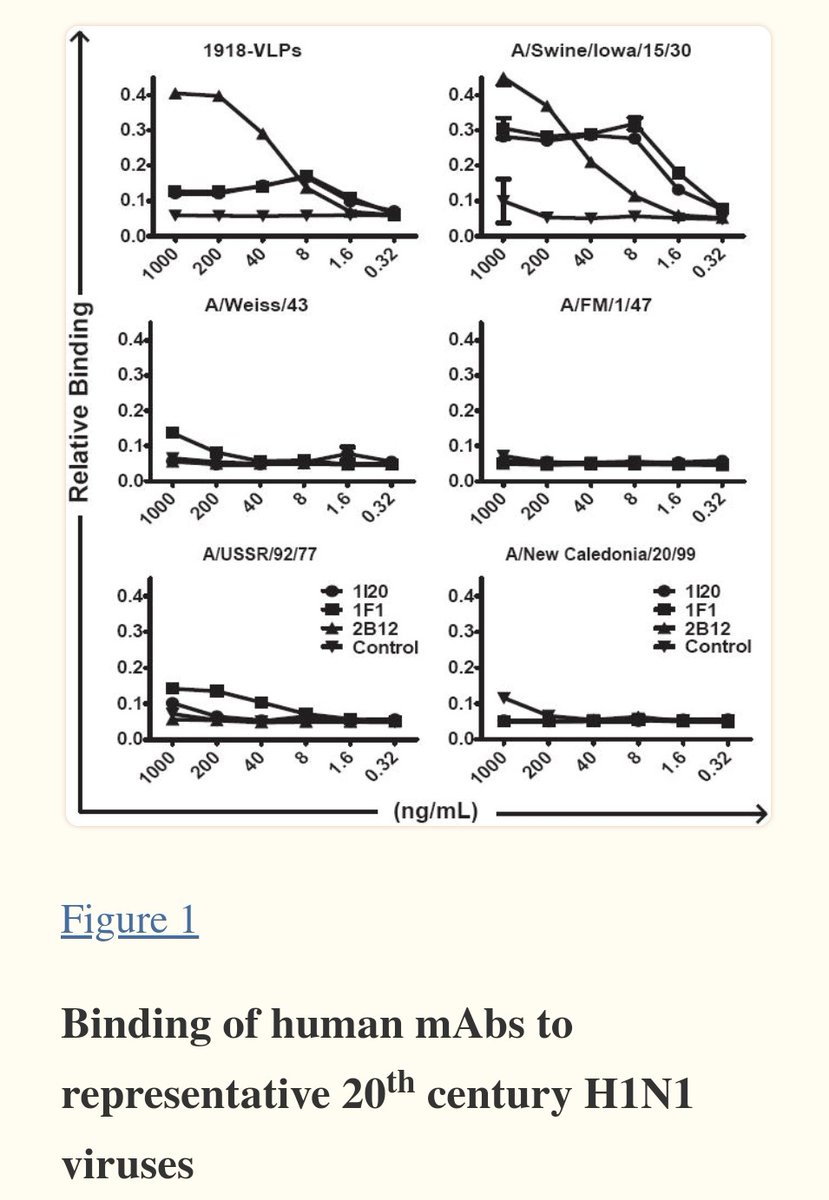
UNDERSTANDING IMMUNE DIVERSITY (part 4) : BACK to the PAST We still have antibodies from the 1918 pandemic flu !
@ejustin46 - Emmanuel
2) Scientists "demonstrate that survivors of the 1918 influenza pandemic possess functional, virus-neutralizing antibodies to this uniquely virulent virus, and that humans can sustain circulating B memory cells to viruses for many decades after exposure" https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2848880/

@ejustin46 - Emmanuel
3) In another study they "establishes links between past evolutionary events, such as natural selection or Neanderthal admixture, and current population disparities in immune responses and COVID-19 risk."
@ejustin46 - Emmanuel
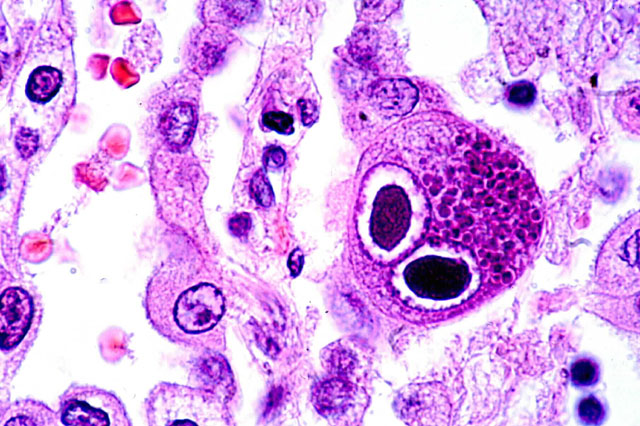
4) Scientists of Pasteur recently studied "that blood cell composition can be influenced by environmental factors such as exposure to cytomegalovirus (a human infection of the herpes family, which is usually harmless) and cytomegalovirus prevalence ...
@ejustin46 - Emmanuel
5) ... varies widely among populations: Central Africans present 99% seropositivity, in contrast to only 50% in East Asians and 32% in Europeans. The team found that an individual’s environment, specifically latent cytomegalovirus infection ...
@ejustin46 - Emmanuel
6) ...will thus influence the immune cell response to SARS-CoV-2." "SARS-CoV-2: how the history of human populations influences their immune response" https://www.pasteur.fr/en/press-area/press-documents/sars-cov-2-how-history-human-populations-influences-their-immune-response

@ejustin46 - Emmanuel
7) Scientists showed also that some specific T cells induced by other coronaviruses (such as common colds) may provide some protection against SARS-CoV-2. https://www.science.org/doi/10.1126/sciimmunol.abd2071 https://t.co/EPUDxn10Cw
@ejustin46 - Emmanuel
8) It is the past that allows us to understand the present, and try to predict what tomorrow will be like. Thanks for reading 🙏 https://t.co/kTSkJTecR4 https://t.co/IzScKCcN8i

@ejustin46 - Emmanuel
ARE SOME PEOPLE IMMUNE to COVID-19 or ALWAYS ASYMPTOMATIC ? (understanding immune diversity - part 3) Immunity is diverse and we are not all equal when it comes to infection or disease
@ejustin46 - Emmanuel
2) Let's start with a few examples. In 2021 was published a study of 86 couples in Brazil, in which one partner developed severe COVID-19, the other showed no symptoms, and they shared bedrooms. Why wasn't their partner sick? https://www.medrxiv.org/content/10.1101/2021.04.21.21255872v1

@ejustin46 - Emmanuel
3) Let's take another example than COVID, that of HIV with Stephen Crohn, a New York artist, which had numerous HIV-positive sex partners, several of whom died from AIDS and never get sick. Why ? https://www.npr.org/sections/health-shots/2013/09/21/224506556/in-life-man-immune-to-hiv-helped-scientists-fight-virus

@ejustin46 - Emmanuel
4) There was also a recent study which tried to understand why some individuals never had COVID-19 ?
@ejustin46 - Emmanuel
5) What all of these examples have in common, is what we call the homeostatic control of infection. This control depends on various host factors, which include the immune system (the primary defense mechanism) but also on many other factors https://t.co/bkPROQuUi4
@ejustin46 - Emmanuel
6) ... which make it possible to understand the differences from one individual to another when it comes to infection, but also over time. Given that it is complex, we will address this subject including the risks following repeated infections, through several threads. Thanks🙏 https://t.co/hgnIdM5yjA

@ejustin46 - Emmanuel
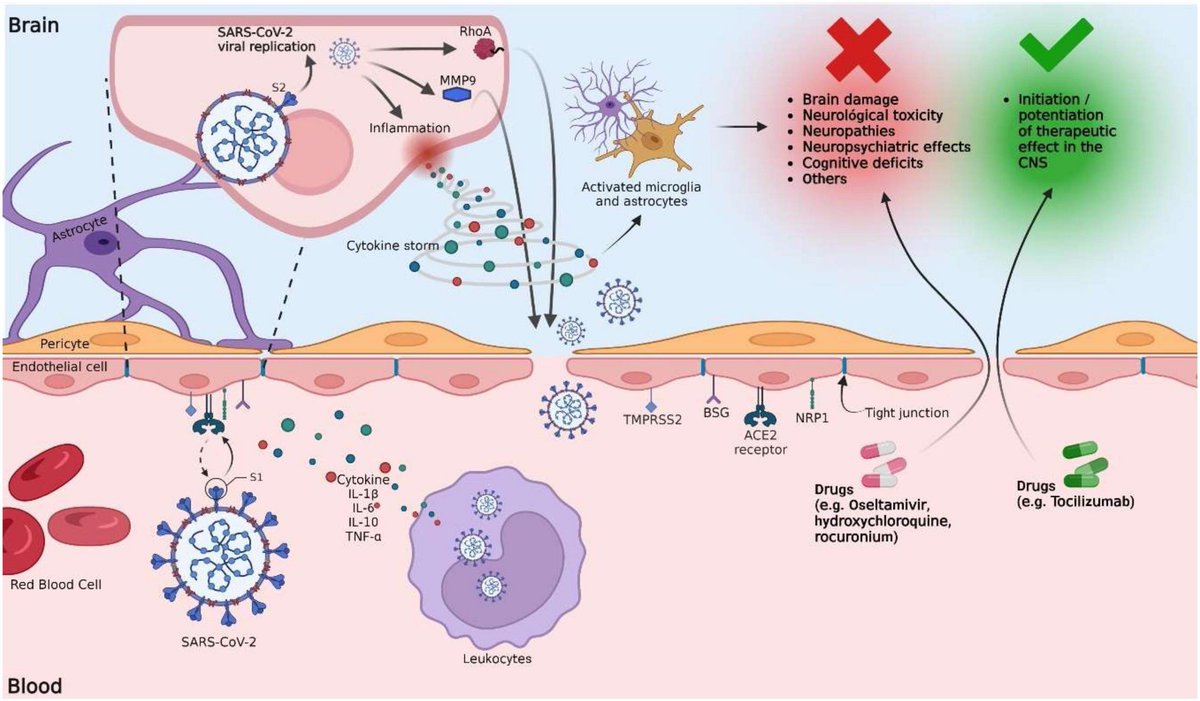
8) "Alteration of the blood-brain barrier by COVID-19 and its implication in the permeation of drugs into the brain" https://www.frontiersin.org/articles/10.3389/fncel.2023.1125109

@ejustin46 - Emmanuel
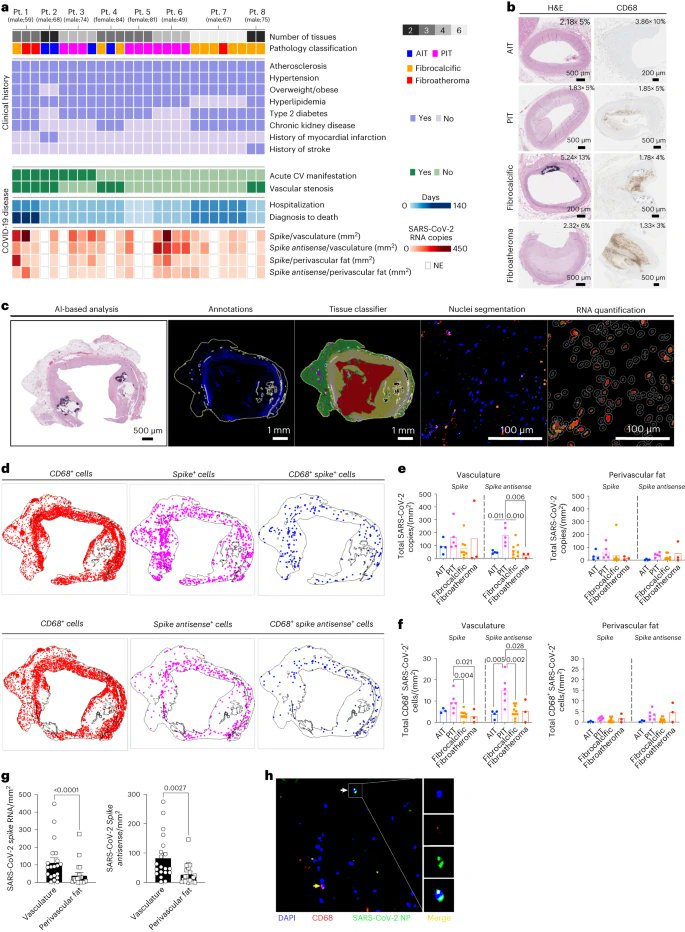
9) NEW KEY STUDY ! H/t @MarionKoopmans "SARS-CoV-2 infection triggers pro-atherogenic inflammatory responses in human coronary vessels" https://www.nature.com/articles/s44161-023-00336-5#Sec7
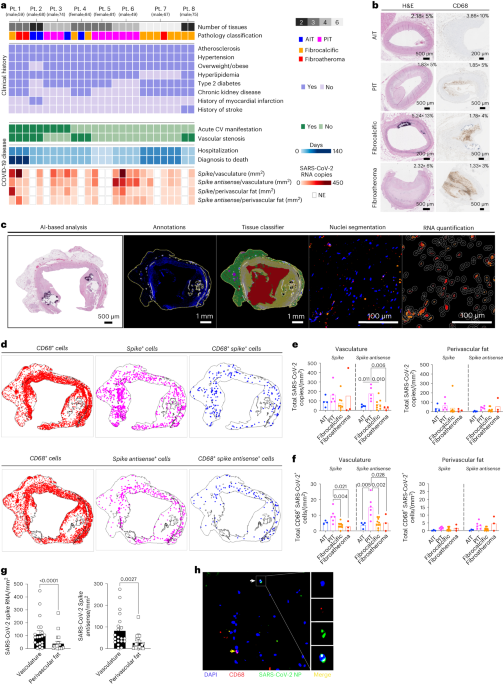
@ejustin46 - Emmanuel
10) Thanks for reading 🙏 FYI @MeetJess @LauraMiers @KatePri14608408 @DavidJoffe64 @RadCentrism @C_A_Gustave @arijitchakrav @HarrySpoelstra @1goodtern @outbreakupdates @RolandBakerIII @AltenbergLee https://t.co/wpqkabOhws